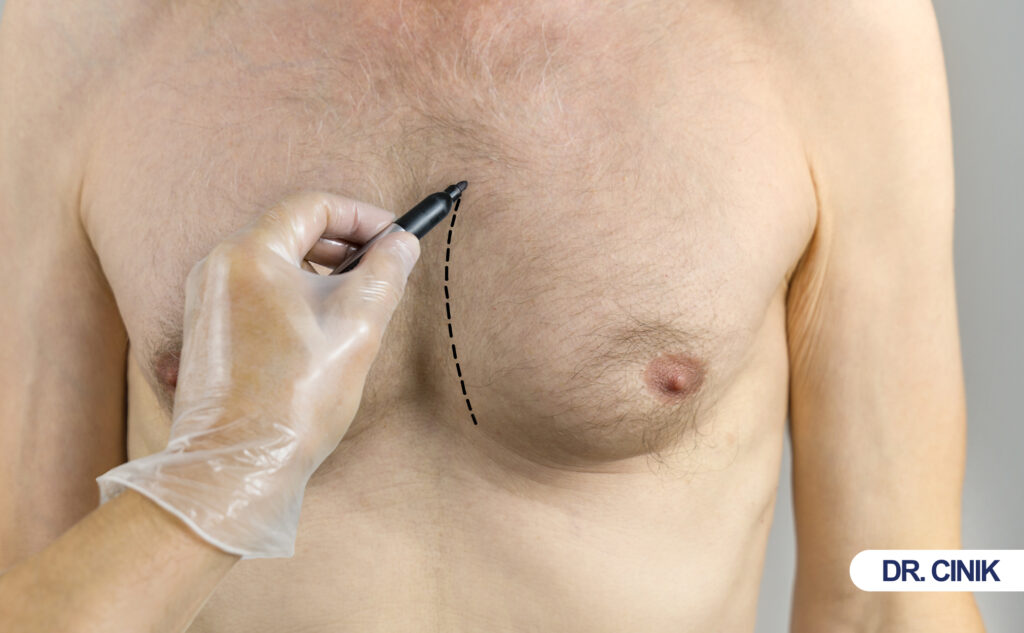
Gynecomastia surgery removes excess breast tissue from men. This procedure flattens the chest wall and restores a masculine contour. Men seek this surgery when breast enlargement persists despite diet and exercise.
Gynecomastia affects up to sixty-five percent of adolescent boys and thirty-five percent of adult men at some point in life (Nuzzi 2018). The condition creates physical discomfort and severe emotional distress. Many men avoid swimming, gym workouts, and intimate relationships because of enlarged breast tissue. Gynecomastia surgery offers a definitive solution. Surgeons remove glandular tissue and excess fat through small incisions. The procedure improves both physical appearance and psychological wellbeing.
Male breast reduction represents one of the most common aesthetic surgeries for men. The demand for gynecomastia treatment has risen steadily over the past decade. Social awareness and reduced stigma drive more men to seek help. Gynecomastia surgery delivers permanent results in properly selected patients.
What Causes Gynecomastia in Men?
Hormonal imbalance causes most cases of gynecomastia. Some medications and diseases also trigger breast tissue growth. Doctors must identify the root cause before recommending surgery.
How Does Hormonal Imbalance Trigger Breast Tissue Growth?
Estrogen stimulates breast tissue growth. Testosterone normally blocks this effect. When estrogen rises or testosterone drops, breast tissue grows.
The human breast contains both glandular tissue and fat cells. Estrogen binds to receptors in these cells and triggers enlargement. Testosterone normally counteracts estrogen in men. When this balance fails, gynecomastia develops (Kanakis 2019). Puberty causes temporary hormone swings. Up to seventy percent of boys develop some breast enlargement during adolescence. Most cases resolve within eighteen months. Adult men experience gynecomastia when aging reduces testosterone. Obesity also raises estrogen levels because fat cells convert testosterone into estrogen. This process fuels persistent breast growth.
What Medications and Health Conditions Cause Gynecomastia?
Anti-androgens, steroids, and some heart medications cause gynecomastia. Liver disease, thyroid problems, and kidney failure also trigger it.
Many prescription drugs disrupt the estrogen-to-testosterone ratio. Spironolactone, cimetidine, and some antidepressants raise estrogen activity. Anabolic steroids remain a major culprit among bodybuilders. Twenty-five percent of steroid users develop gynecomastia (Fagerlund 2003). Systemic diseases alter hormone metabolism. Cirrhosis reduces testosterone production. Hyperthyroidism increases estrogen binding. Chronic kidney failure changes how the body clears hormones. Substance use contributes too. Alcohol damages the liver and raises estrogen. Marijuana and amphetamines also affect hormone balance.
How Do Doctors Classify Gynecomastia Severity?
Doctors use the Simon system. It grades severity from I to III based on tissue amount and skin excess.
Simon and colleagues developed this classification in 1973 (Simon 1973). It guides surgical planning and helps doctors set realistic goals. True gynecomastia involves glandular tissue. Pseudogynecomastia involves only fat. Doctors distinguish these types during physical exam.
Table 1: Simon Classification of Gynecomastia
|
Grade |
Tissue Description |
Skin Excess |
Surgical Approach |
|
I |
Small glandular enlargement |
None |
Liposuction or minor excision |
|
II |
Moderate enlargement |
Minimal |
Combined liposuction and excision |
|
III |
Large enlargement |
Significant |
Excision plus skin removal |
Grade I patients need minimal intervention. Grade II patients require combined techniques. Grade III patients need extensive tissue removal and skin tightening.
Who Qualifies for Gynecomastia Surgery?
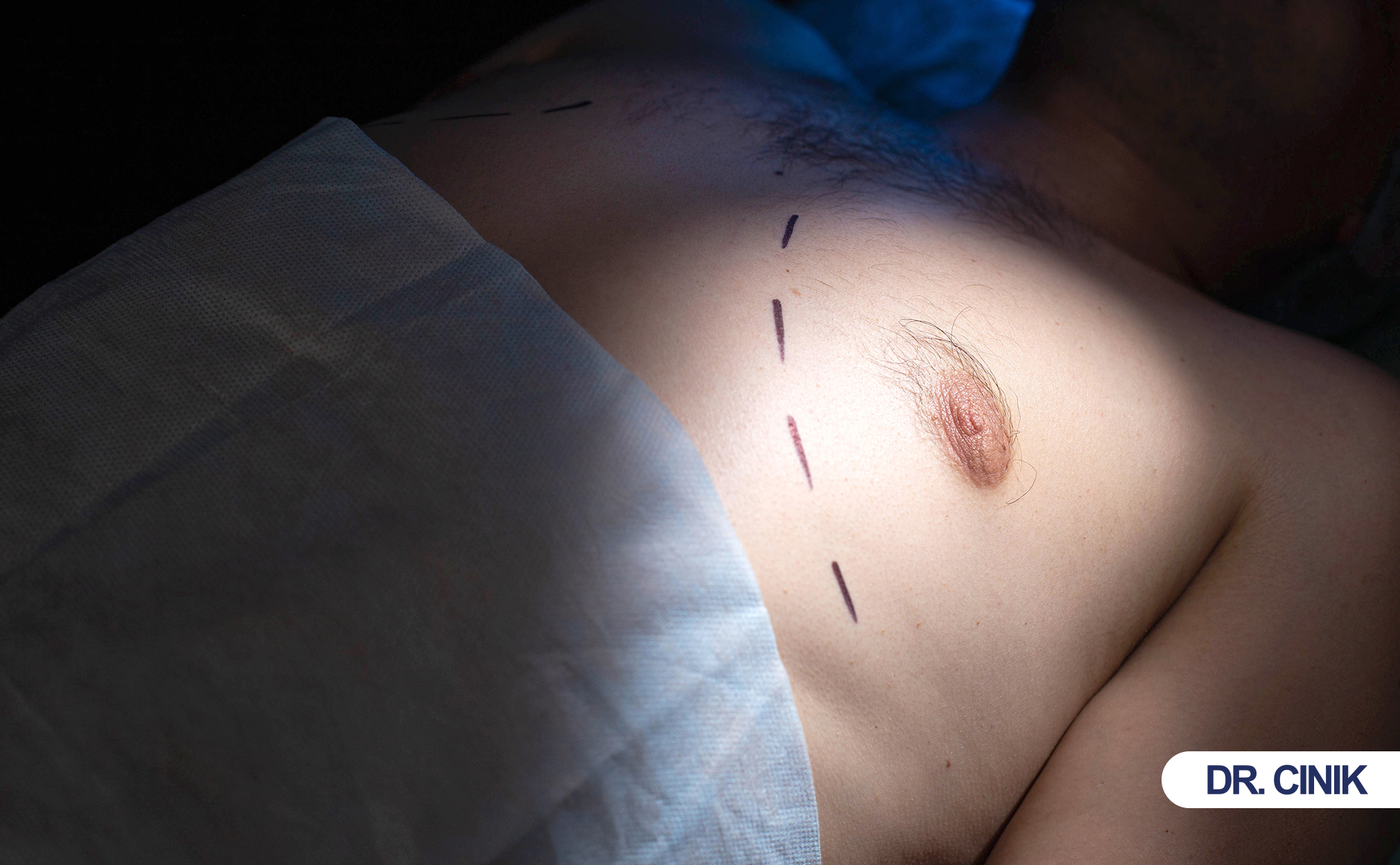
Men with persistent tissue growth, pain, or severe emotional distress qualify. Doctors screen for underlying diseases first. Proper patient selection ensures safety and satisfaction.
What Medical Signs Indicate Surgery?
Tissue persists beyond twelve months. Pain limits daily activities. The tissue feels firm and glandular.
Doctors recommend surgery when gynecomastia stabilizes and causes physical symptoms. Tenderness during exercise or clothing friction indicates true glandular tissue. Liposuction alone cannot remove this firm tissue. Excision becomes necessary. Doctors also consider surgery when asymmetry creates postural problems or skin irritation beneath the breast fold. Cordova and Moschella emphasize that stable, long-standing gynecomastia responds best to surgical correction (Cordova 2008).
What Psychological Factors Drive Men to Surgery?
Men feel shame, avoid social events, and refuse tight clothing. These emotional burdens justify surgery.
Gynecomastia severely impacts mental health. Teenagers skip physical education classes. Adults avoid beaches and gyms. Many men report social anxiety and depression. Studies show that gynecomastia surgery improves body image scores significantly. Men feel relief within weeks after the procedure. The psychological benefit often exceeds the physical improvement. Surgeons recognize emotional distress as a valid indication for male breast reduction.
What Conditions Prevent Surgery?
Untreated hormone disorders, active infections, and unrealistic expectations block candidacy.
Doctors must rule out fixable causes first. They treat hormone-secreting tumors before considering surgery. They stabilize thyroid and liver diseases. Active smokers face higher complication rates. Doctors require smoking cessation before scheduling surgery. Patients with unrealistic expectations also pose problems. Surgery improves contour but cannot create a perfect physique. Good candidates understand these limits.
What Happens During Preoperative Evaluation?
Doctors examine the chest, test hormone levels, and review medical history. They also assess skin quality. This evaluation ensures safe, effective treatment.
What Does the Physical Exam Reveal?
The exam shows glandular versus fatty tissue. It also reveals skin elasticity and nipple position.
Doctors palpate the breast tissue during the exam. Glandular tissue feels firm and rubbery. Fatty tissue feels soft and mobile. Doctors test skin elasticity by pinching the skin. Poor elasticity predicts sagging after tissue removal. Doctors also check nipple sensation and position. Severe gynecomastia stretches the nipple downward. This finding affects incision planning. Waltho and colleagues stress that careful physical exam prevents surgical surprises (Waltho 2017).
What Tests Do Doctors Order?
Doctors order hormone panels and breast ultrasound. Mammography helps in older patients.
Blood tests measure testosterone, estrogen, prolactin, and thyroid hormones. These tests reveal hidden endocrine problems. Imaging studies confirm tissue composition. Ultrasound distinguishes solid glandular tissue from fat. Doctors order mammography when they suspect breast cancer. Breast cancer remains rare in men but demands exclusion. Patients over forty years old need more thorough screening.
How Do Doctors Assess Surgical Risks?
Doctors review smoking status, obesity, and heart health. These factors affect healing and safety.
Obesity increases surgical risk and reduces aesthetic results. Doctors recommend weight loss before surgery when possible. Diabetes slows wound healing. Doctors demand good blood sugar control. Blood-thinning medications increase bleeding risk. Patients must stop these drugs before surgery. The American Society of Plastic Surgeons emphasizes thorough risk stratification for all cosmetic procedures.
What Surgical Techniques Correct Gynecomastia?
Surgeons use liposuction, excision, or both. The choice depends on tissue type and skin excess. Each technique addresses specific anatomical needs.
When Do Surgeons Use Liposuction?
Liposuction works best for fatty tissue. Surgeons use traditional, power-assisted, or ultrasound-assisted methods.
Pseudogynecomastia responds well to liposuction alone. Surgeons insert small cannulas through three-to-four-millimeter incisions. They break up fat cells and suction them out. Power-assisted liposuction uses rapid vibrations. This technology reduces surgeon fatigue and improves precision. Ultrasound-assisted liposuction melts fat with sound waves. It works well in dense, fibrous tissue. Liposuction alone cannot remove glandular tissue. It only removes fat cells.
When Do Surgeons Perform Excision?
Excision removes glandular tissue and excess skin. Surgeons place incisions around the nipple.
True gynecomastia requires direct tissue removal. Surgeons make a semi-circular incision along the lower half of the areola. This location hides scars effectively. They dissect out the glandular disc beneath the nipple. They preserve a thin layer of tissue to prevent contour deformities. In Grade III cases, surgeons remove excess skin through larger incisions. These incisions may extend across the chest fold. Excision creates more visible scars than liposuction. It remains necessary for glandular removal.
Why Do Surgeons Combine Both Methods?
Most men have both fat and glandular tissue. Combining methods delivers the flattest result.
Surgeons perform liposuction first. This step thins the fatty layer around the breast. Then they perform excision through the periareolar incision. This sequence removes the glandular core. The combined approach prevents the “crater deformity.” This complication occurs when surgeons remove too much tissue directly under the skin. Liposuction feathering blends the edges smoothly. Kasielska and Antoszewski report that combined techniques produce the most natural chest contours (Kasielska 2013).
Table 2: Comparison of Surgical Techniques
|
Technique |
Tissue Target |
Incision Size |
Best Candidate |
Recovery Speed |
|
Liposuction only |
Fat |
3-4 mm |
Pseudogynecomastia |
Fast |
|
Excision only |
Glandular + skin |
Periareolar |
True gynecomastia |
Moderate |
|
Combined |
Fat + glandular |
Multiple small |
Mixed gynecomastia |
Moderate |
|
Skin tightening |
Excess skin |
Extended |
Grade III |
Slower |
What New Techniques Improve Results?
Surgeons now use smaller incisions and energy devices. These advances tighten skin with less cutting.
Radiofrequency devices heat the underside of the skin. This heat stimulates collagenA structural protein found in the skin and other connective tissues, which is responsible for skin firmness and elasticity.... and tightens loose tissue. Surgeons use these devices through liposuction incisions. They avoid long excision scars in borderline cases. Endoscopic techniques allow gland removal through remote incisions. These approaches hide scars in the armpit. Laser lipolysis also melts fat and tightens skin simultaneously. These innovations expand treatment options for mild to moderate cases.
How Do AnesthesiaEnsuring Comfort During Hair Transplants Sedation is used in hair transplantation to help patients remain calm and comfortable throughout the... and Operating Room Protocols Work?
Most surgeons use general anesthesia. The procedure takes one to three hours. Patients go home the same day.
Anesthesia choice depends on tissue extent and patient anxiety. Minor liposuction cases tolerate local anesthesia with sedation. Most excision cases require general anesthesia. Board-certified anesthesiologists monitor vital signs throughout. Intraoperative safety protocols include compression stockings and warming blankets. These measures prevent blood clots and hypothermia. Surgeons mark incision lines while the patient sits upright. This positioning accounts for gravity and tissue shift. The operating team positions the patient with arms abducted. This exposure allows full chest access. Hammond notes that outpatient settings reduce cost and infection risk (Hammond 2009).
What Does Recovery Look Like After Gynecomastia Surgery?
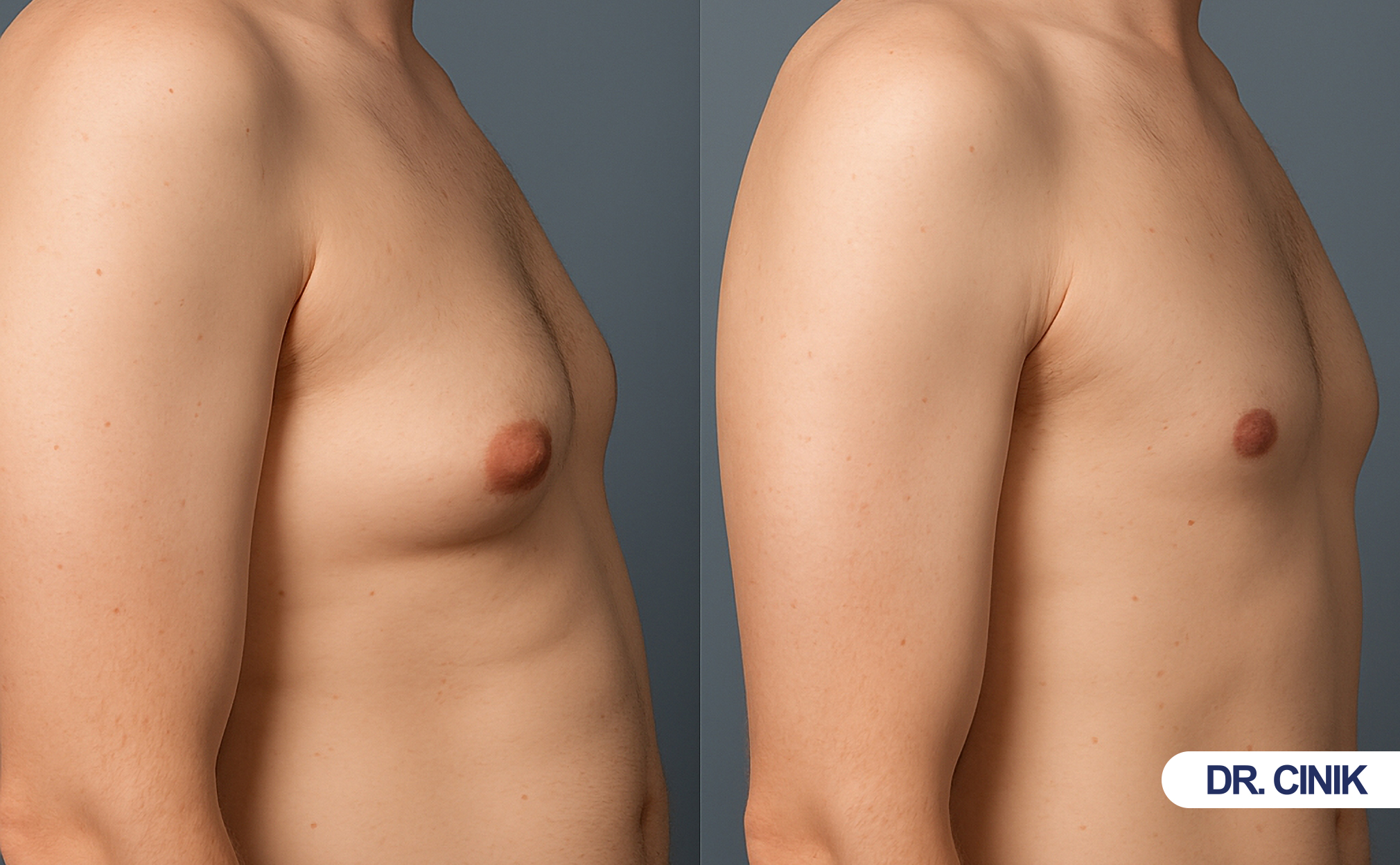
Patients wear compression garments. They return to work in one to two weeks. Full healing takes three to six months.
What Happens Immediately After Surgery?
Swelling and bruising appear. Pain remains mild to moderate. Compression garments control fluid buildup.
Nurses place dressings and a compression vest before the patient wakes. This garment applies steady pressure. Pressure reduces swelling and prevents fluid accumulation. Patients feel tightness and soreness for three to five days. Prescription pain medication controls discomfort. Most men switch to over-the-counter drugs within seventy-two hours. Bruising spreads across the chest and upper abdomen. It peaks at day three. Small drainage tubes may exit through the incisions. Doctors remove these tubes within twenty-four to forty-eight hours.
How Long Does Full Recovery Take?
Bruising fades in two to three weeks. Swelling drops by six weeks. The final chest shape appears at six months.
Healing progresses gradually. The chest looks swollen and firm during the first month. Patients often worry that tissue remains. This swelling masks the true result. By week six, fifty percent of swelling resolves. By month three, eighty percent resolves. The skin redrapes slowly. Scar tissue softens over four to six months. Patients must practice patience during this timeline.
Table 3: Recovery Timeline After Gynecomastia Surgery
|
Time Period |
Work Activity |
Exercise Level |
Chest Appearance |
|
Days 1-7 |
Rest only |
Walking only |
Very swollen, bruised |
|
Weeks 2-3 |
Desk work |
Light stretching |
Bruising fades, firm |
|
Weeks 4-6 |
Normal job |
Light cardio |
Swelling decreases |
|
Months 2-3 |
All activities |
Full exercise |
Contour improves |
|
Months 4-6 |
Unrestricted |
All sports |
Final shape visible |
What Activities Must Patients Avoid?
Patients avoid heavy lifting for four to six weeks. They also skip chest workouts during early healing.
Strenuous activity raises blood pressure. High pressure increases bleeding risk. Patients must keep their heart rate below one hundred beats per minute for two weeks. They must not lift anything heavier than ten pounds for four weeks. Chest-specific exercises like push-ups and bench presses remain off-limits for six weeks. Walking promotes circulation and prevents clots. Patients should walk several times daily starting on day one.
How Do Scars Heal Over Time?
Scars look red at first. They fade over twelve months. Silicone sheets and massage help.
Periareolar scars hide along the pigment border. They appear pink during the first month. They darken slightly before fading. Patients begin silicone gel or sheet therapy at week two. They massage scars daily after month one. Massage breaks down collagen bundles. It softens and flattens scar tissue. Sun protection remains critical. Ultraviolet light darkens scars permanently. Patients must cover chest scars for six months after surgery.
What Results Can Patients Expect?
The chest looks flatter and more masculine. Most patients report high satisfaction. Results last permanently.
How Does the Chest Look After Surgery?
The contour improves immediately. The final shape settles after swelling resolves. Symmetry matches the opposite side.
Surgeons aim for a flat, athletic chest contour. They preserve the natural slope from the nipple to the outer chest. They avoid over-resection. Over-resection creates a sunken, unnatural look. Good results show a smooth transition between the breast area and the upper abdomen. Nipples sit at the correct height and projection. Asymmetry corrections balance both sides. Patients see dramatic changes in clothing fit. T-shirts drape properly. Button-down shirts no longer gap.
How Does Surgery Improve Daily Life?
Men report less physical discomfort. They exercise freely. They also feel more confident in clothing.
Before surgery, many men wear multiple layers or compression shirts. They avoid beaches and locker rooms. After surgery, they participate fully in sports and social events. Physical symptoms disappear. Tenderness and chafing resolve. The psychological benefit often surprises patients. Men stand straighter. They make better eye contact. They report improved romantic confidence. Studies confirm that gynecomastia surgery raises quality-of-life scores significantly.
How Long Do Results Last?
Removed glandular tissue never returns. Weight gain can add fat. Hormone disorders may cause rare recurrence.
Surgeons remove the glandular disc completely. This tissue cannot regenerate. Fat cells removed by liposuction also disappear permanently. However, remaining fat cells can expand if the patient gains weight. Men must maintain stable weight after surgery. Untreated hormone disorders may stimulate new tissue growth. Patients who use anabolic steroids face recurrence. Proper hormone management prevents this problem. Rohrich and colleagues confirm that recurrence rates remain below five percent in compliant patients (Rohrich 2003).
What Risks and Complications Exist?
Bruising and swelling occur routinely. Serious risks include infection, bleeding, and contour problems. Understanding these risks helps patients prepare.
What Common Side Effects Occur?
Bruising covers the chest for two weeks. Swelling peaks at three days. Mild pain responds to medication.
Every patient experiences bruising and swelling. These side effects represent normal healing, not complications. Numbness around the incisions lasts several weeks. It resolves as nerves heal. Some patients develop firmness beneath the skin. This firmness represents deep scar tissue. It softens with massage over two to three months.
What Surgical Risks Should Patients Know?
Scars form around the nipple. Asymmetry affects some patients. Nipple sensation may change.
Scar quality varies by genetics and skin type. Darker skin types carry higher keloid risk. Asymmetry occurs when healing differs between sides. Minor contour irregularities may need revision. Nipple sensation changes happen in fifteen percent of patients. Most changes resolve within six months. Permanent numbness remains rare. Loss of blood supply to the nipple threatens tissue survival. Surgeons prevent this by preserving adequate vascular connections.
What Rare Complications Can Happen?
Blood clots and anesthesia reactions occur rarely. Tissue damage beneath the breast remains uncommon.
Deep vein thrombosis affects less than one percent of patients. Early walking prevents this complication. Pulmonary embolism remains extremely rare. Anesthesia reactions happen in one per ten thousand cases. Modern monitoring makes these events manageable. Injury to deeper chest muscles or ribs almost never occurs. Surgeons work above the muscle layer. They avoid these structures entirely.
When Do Patients Need Revision Surgery?
Revision corrects asymmetry, residual tissue, or scar problems. Fewer than ten percent of patients need this.
Residual glandular tissue causes persistent fullness beneath the nipple. Asymmetry becomes apparent after swelling resolves. Prominent scars may require steroid injections or laser therapy. Revision surgery typically involves less extensive work than the original procedure. Patients must wait at least six months before considering revision. This waiting period allows full healing and tissue settling.
How Does Surgery Affect Mental Health?
Anxiety drops after surgery. Self-esteem rises. Most men feel relief within one month.
Gynecomastia surgery transforms psychological wellbeing. Preoperative anxiety often centers on social exposure. Men fear judgment and ridicule. After surgery, this burden lifts. Patients report immediate mood improvement. They engage more actively in relationships and careers. Long-term studies show sustained confidence gains at five years post-surgery. The procedure addresses both body and mind.
How Much Does Gynecomastia Surgery Cost?
Costs range from three thousand to ten thousand dollars. Technique, location, and surgeon skill determine the price.
Insurance rarely covers gynecomastia surgery. They classify it as cosmetic. Some plans cover the procedure when patients document severe pain or psychological impairment. Patients should verify coverage before scheduling. Financing plans help spread costs over twelve to twenty-four months.
How Does Surgery Compare to Non-Surgical Options?
Non-surgical options help mild cases. Surgery remains the only permanent fix for glandular tissue. Patients should understand these limits.
Can Hormonal Therapy Fix Gynecomastia?
Drugs like tamoxifen shrink early tissue. They fail in long-standing cases. Side effects limit use.
Tamoxifen blocks estrogen receptors. It works best during the painful, proliferative phase. This phase occurs within the first twelve months. After tissue fibrosis sets in, drugs cannot reverse the enlargement. Aromatase inhibitors reduce estrogen production. They show mixed results. Side effects include mood swings, sexual dysfunction, and hot flashes. Endocrinologists reserve drug therapy for specific hormone disorders. They do not recommend drugs as primary treatment for established gynecomastia.
Can Exercise and Weight Loss Eliminate It?
Diet and exercise reduce fatty tissue. They cannot remove glandular tissue. Pseudogynecomastia responds better.
Weight loss shrinks fat cells throughout the body. It improves pseudogynecomastia significantly. It leaves true glandular tissue untouched. Bodybuilders with steroid-induced gynecomastia often have low body fat. Their chest tissue remains prominent despite peak fitness. Exercise cannot burn away glandular discs. It improves overall physique but not localized breast enlargement.
Table 5: Surgery vs. Non-Surgical Treatments
|
Treatment |
Removes Glandular Tissue |
Permanent Result |
Best For |
Limitations |
|
Surgery |
Yes |
Yes |
All grades |
Recovery time, cost |
|
Hormonal drugs |
No |
No |
Early phase only |
Side effects, limited success |
|
Weight loss |
No |
Partial |
Pseudogynecomastia |
Fails on glandular tissue |
|
Exercise |
No |
No |
General fitness |
Cannot target breast tissue |
Why Does Surgery Remain the Best Solution?
Surgery physically removes glandular tissue. No other method achieves this. Recurrence remains rare.
Gynecomastia surgery stands as the gold standard for persistent cases. It eliminates the root problem. It delivers predictable, visible results. It works regardless of tissue type. It also removes excess skin in severe cases. Non-surgical methods manage symptoms or reduce fat. They do not address glandular overgrowth. For men with long-standing gynecomastia, surgery offers the only definitive path forward.
What Future Innovations Will Improve Surgery?
Smaller scopes and radiofrequency devices tighten skin. Surgeons also refine scar therapies. These advances promise better results with less downtime.
Minimally invasive techniques continue evolving. Endoscopic gland removal through axillary incisions eliminates chest scars entirely. Radiofrequency skin tightening reduces the need for skin excision in borderline Grade II cases. Three-dimensional imaging helps surgeons plan tissue removal more precisely. Stem cell therapies may improve scar quality in the future. These innovations expand access and reduce recovery burdens.
Frequently Asked Questions
Patients ask about pain, permanence, scars, and recovery time. Doctors answer these at consultation. Clear answers reduce anxiety.
What is gynecomastia surgery?
Gynecomastia surgery removes excess male breast tissue. It combines liposuction and excision techniques. It creates a flatter, more masculine chest.
Is gynecomastia surgery permanent?
Yes, the surgery removes glandular tissue permanently. Weight gain or hormone disorders may cause rare recurrence. Stable patients enjoy lifelong results.
How painful is gynecomastia surgery?
Patients feel soreness and tightness for three to five days. Pain medication controls discomfort effectively. Most men describe the pain as mild to moderate.
How long is recovery?
Patients return to desk work in one to two weeks. They resume full exercise in four to six weeks. Final results appear at three to six months.
Are the scars visible?
Surgeons hide scars along the areola edge. They fade significantly over one year. Most men find scars nearly invisible after maturation.
Can gynecomastia return after surgery?
True recurrence remains rare. Removed tissue cannot grow back. New tissue may form if the patient uses steroids or develops hormone disorders.
What Should Men Remember About Gynecomastia Surgery?
Proper patient selection ensures safety. Experienced surgeons optimize outcomes. Realistic expectations prevent disappointment.
Gynecomastia surgery offers one of the most satisfying procedures in male aesthetic surgery. It resolves both physical and emotional suffering. It works for adolescents and adults alike. It requires careful evaluation, skilled technique, and dedicated aftercare. Men should choose board-certified plastic surgeons with specific gynecomastia experience. They should follow all preoperative and postoperative instructions. They should maintain stable weight and hormone levels after recovery. With these steps, gynecomastia surgery delivers permanent, life-enhancing results.
References
Cordova, A., and F. Moschella. “Algorithm for Clinical Evaluation and Surgical Treatment of Gynecomastia.” Journal of Plastic, Reconstructive & Aesthetic Surgery, vol. 61, no. 1, 2008, pp. 41-49.
Fagerlund, Anders, and Luigi Cormio. “Gynecomastia: A Review.” European Journal of Surgery, vol. 169, no. 2, 2003, pp. 106-110.
Hammond, D. C. “Surgical Correction of Gynecomastia.” Plastic and Reconstructive Surgery, vol. 124, no. 4, 2009, pp. 61e-68e.
Kanakis, George A., et al. “Endocrine Aspects of Gynecomastia.” Andrology, vol. 7, no. 6, 2019, pp. 778-788.
Kasielska, Anna, and Bogusław Antoszewski. “Surgical Treatment of Gynecomastia.” Polish Journal of Surgery, vol. 85, no. 5, 2013, pp. 261-267.
Nuzzi, Laura C., et al. “Adolescent Gynecomastia: Clinical Characteristics and Management.” Annals of Plastic Surgery, vol. 80, no. 2, 2018, pp. 135-140.
Rohrich, Rod J., et al. “Classification and Management of Gynecomastia.” Plastic and Reconstructive Surgery, vol. 111, no. 2, 2003, pp. 909-912.
Simon, Bernard E., et al. “Classification and Surgical Correction of Gynecomastia.” Plastic and Reconstructive Surgery, vol. 51, no. 1, 1973, pp. 48-52.
Waltho, Daniel, et al. “Gynecomastia: Etiology, Diagnosis, and Treatment.” Canadian Journal of Plastic Surgery, vol. 25, no. 4, 2017, pp. 261-266.