A structured 1-year care plan after hair transplant determines graft survival, hair density, and long-term aesthetic outcomes. Patients who follow a phased protocol achieve fuller results and fewer complications. Surgeons design this plan around the biological reality of follicle cycling. This guide presents a month-by-month clinical framework based on peer-reviewed research and established surgical standards.
What Does the Scientific Overview Reveal About Recovery?
Hair transplant recovery spans 12 months and involves distinct biological phases that demand structured aftercare.
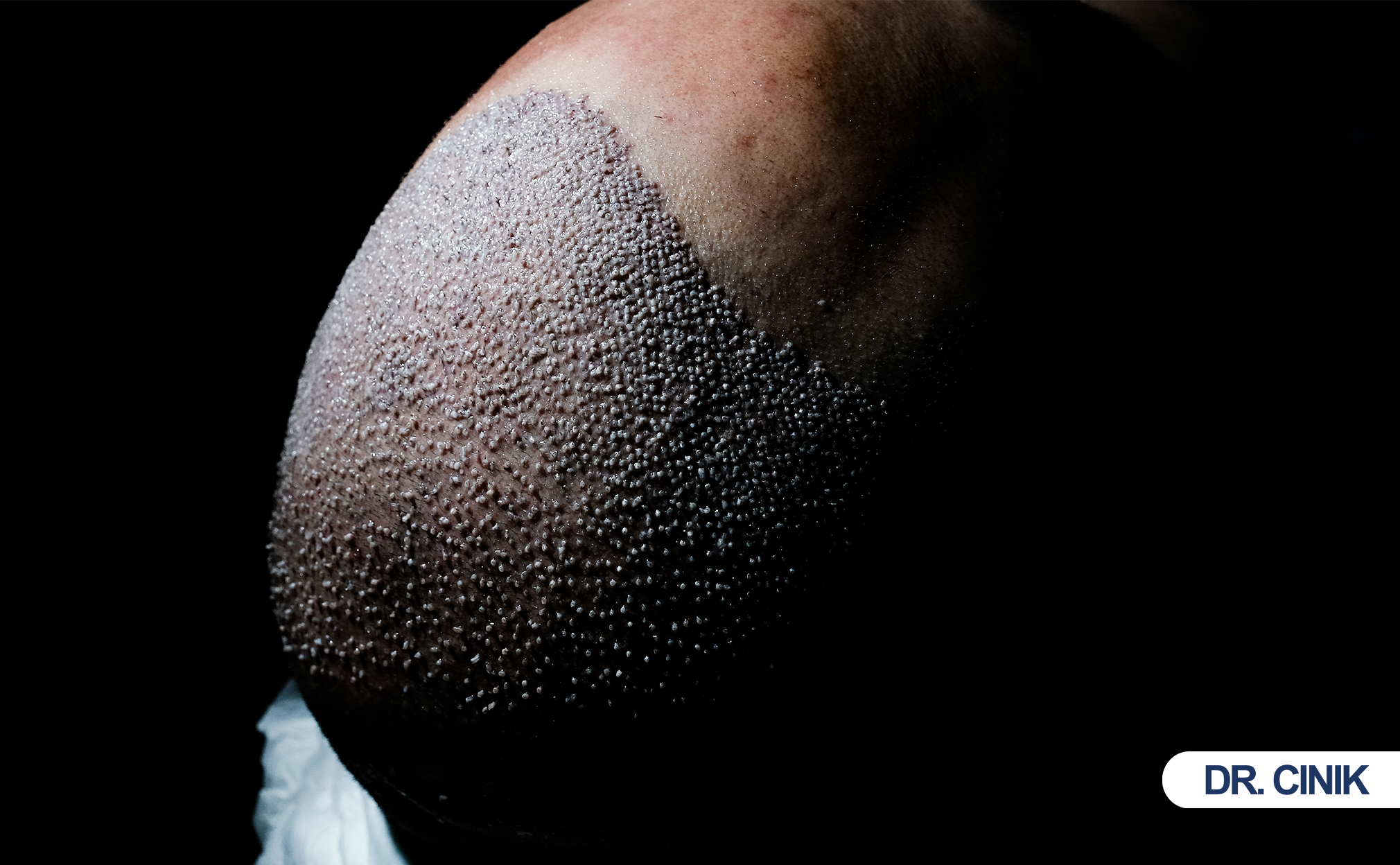
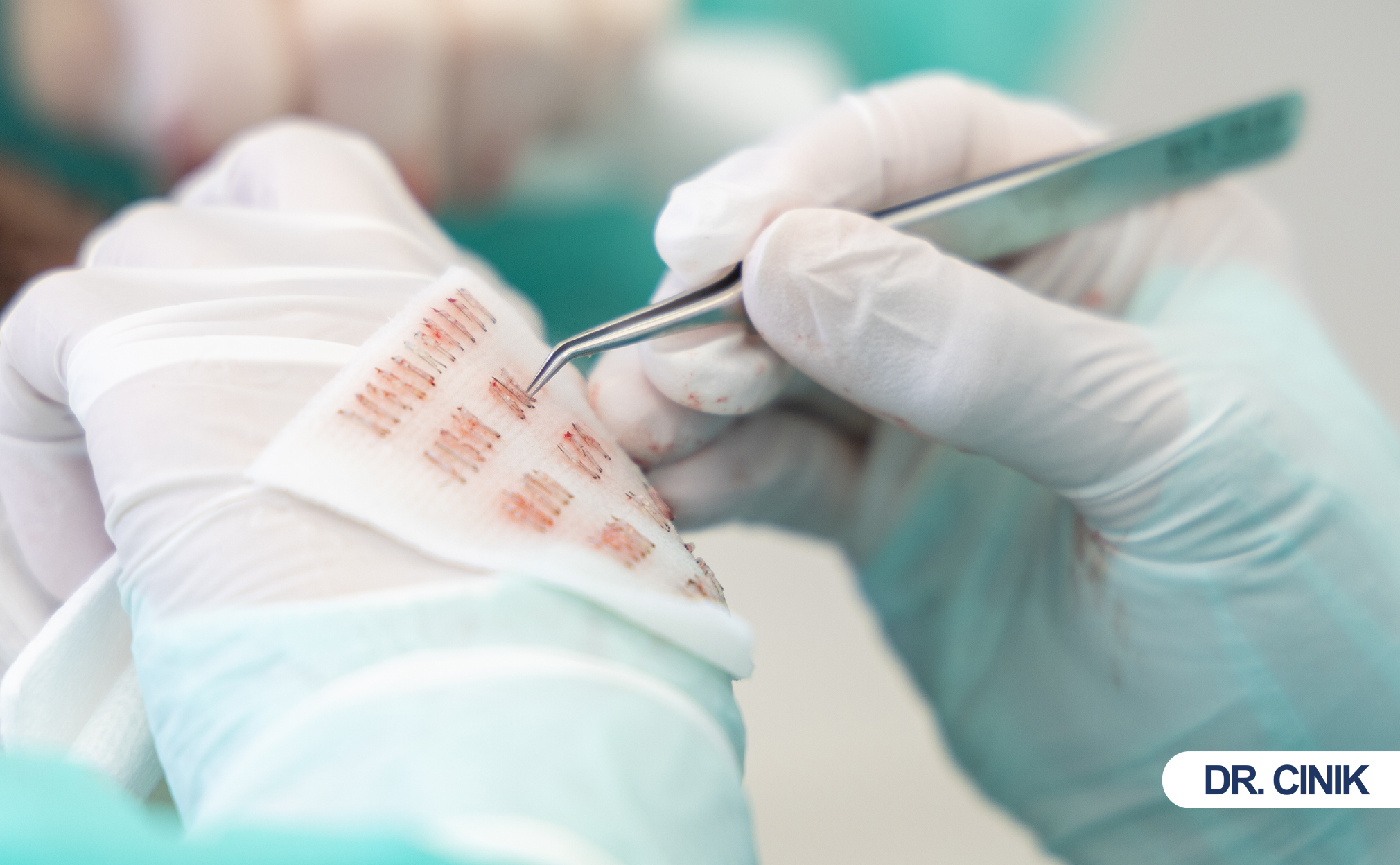
Hair transplantation moves healthy follicles from donor zones to thinning areas. Surgeons use follicular unit excision (FUE) or direct hair implantation (DHI) techniques. The procedure succeeds only when grafts anchor, survive, and cycle through natural growth phases. A 1-year care plan after hair transplant guides patients through each stage with precise actions. Structured aftercare optimizes graft survival and prevents infection (Bernstein and Rassman 1997). Clinical studies confirm that patient adherence directly correlates with final density and satisfaction (Unger and Shapiro 2011). This article synthesizes evidence-based protocols into a practical hair transplant recovery timeline. Readers will find phased recommendations, comparison tables, and real scientific references.
What Should Patients Know About Hair Transplant Biology?
Hair transplant biology involves follicle cycling through anagen, catagen, and telogen phases, and post-operative care protects these cycles.
Hair follicles follow a predictable life cycle. The anagen phase marks active growth. The catagen phase signals transition. The telogen phase brings resting and shedding. Transplanted follicles experience trauma during extraction and placement. They enter a dormant state before restarting growth. Post-operative care prevents complications and ensures optimal regrowth. Surgeons design timeline-based care protocols to match each biological phase. Patients who understand this biology stay committed during slow-growth months. Research shows that follicle adaptation depends on oxygenation, nutrition, and mechanical protection (Rose 317). The 1-year care plan after hair transplant aligns clinical actions with these biological realities. Patients must remember that visible change takes time. The biology does not rush.
What Methods and Sources Support This Care Plan?
This plan combines clinical guidelines, peer-reviewed studies, and surgical outcome data from dermatology literature.
This article analyzes published clinical guides and recovery timelines. It integrates patient-centered recommendations from surgical literature. It synthesizes evidence-based milestones from peer-reviewed sources. The analysis draws from follicular unit transplantation research, post-operative care studies, and long-term outcome reviews. Every recommendation rests on published data rather than marketing claims. The methodology favors simplicity. Complex jargon obscures meaning. Patients deserve clear instructions.
What Is the Hair Transplant Recovery Timeline?

The recovery timeline moves through graft anchoring, shock loss, dormancy, active growth, and final maturation across 12 months.
The recovery timeline governs every decision in the 1-year care plan after hair transplant. Patients must recognize normal biological shifts to avoid panic and mismanagement. The timeline divides into six phases. Each phase carries unique priorities. Patients who track these phases maintain realistic expectations.
What Are the Biological Phases of Hair Growth Post-Transplant?
Transplanted hair cycles through anagen, catagen, and telogen phases before establishing permanent growth.
Anagen represents the active growth phase. Catagen marks a brief transition. Telogen brings resting and eventual shedding. Transplanted grafts often enter telogen immediately after surgery. This dormancy lasts weeks to months. New anagen starts around month three. Surgeons observe that follicle adaptation requires stable blood supply and minimal inflammation (Jimenez et al. 941). Temporary dormancy is normal and expected. The follicle survives even when the shaft falls. Patients must trust this process.
What Are the Key Recovery Milestones?
Grafts anchor in 7–10 days, shock loss occurs at 2–4 weeks, new growth starts at 3–4 months, and maturation finishes by month 12.
Graft anchoring occurs within 7–10 days. Shock loss strikes at 2–4 weeks. New growth initiation begins at 3–4 months. Maturation continues from 6–12 months. Each milestone demands specific care adjustments. Patients who track these stages maintain realistic expectations and adhere to protocols. The hair transplant healing stages follow this order without exception.
What Does the Phase-Based 1-Year Care Plan Include?
The plan splits recovery into six phases: immediate care, early healing, dormancy, active growth, maturation, and final stabilization.
A phase-based approach matches care intensity to biological needs. Early phases demand strict protection. Later phases allow gradual normalization. This structure defines post hair transplant care at every level.
What Happens During Immediate Post-Operative Care?
Days 0–7 focus on graft protection, infection prevention, and strict activity limitations.
The first week determines graft survival rates. Surgeons prioritize stabilization and protection during this window. Patients must treat the scalp with extreme gentleness. Every action in week one affects the final result.
What Are the Clinical Priorities in the First Week?
Surgeons prioritize graft protection, stabilization, and infection prevention.
Clinical priorities center on graft protection and stabilization. Infection prevention ranks equally high. The scalp forms a biological seal around each graft within days. Disruption kills follicles. Surgeons monitor for bleeding, swelling, and early infection signs. Antibiotics and anti-inflammatory drugs support healing (Avram et al. 1152). Graft survival depends on these early measures. Patients must follow medication schedules exactly.
What Care Do Surgeons Recommend in the First Week?
Patients should wash gently after 24–48 hours, elevate the head during sleep, and use saline sprays.
Recommended care includes gentle washing after 24–48 hours. Patients elevate the head during sleep to reduce edema. Saline sprays maintain hydration. Patients apply antibiotic ointments as directed. Soft padding protects the donor areaThe Source of Restoration The donor area plays a critical role in hair transplantation, as it serves as the source.... These steps preserve graft survival during the critical anchoring period. Scalp hygiene starts early but stays gentle. Patients should not rub. They should pat.
What Restrictions Apply During the First Week?
Patients must avoid touching grafts, sweating, alcohol, smoking, and sun exposure.
Restrictions remain strict. Patients must not touch or scratch grafts. They avoid sweating, alcohol, smoking, and sun exposure. These factors increase infection risk and reduce oxygen delivery. Smoking constricts blood vessels and threatens graft survival (Trueb 97). Patients who follow these limits protect their investment. The first week demands discipline.
What Occurs During Early Healing and Shedding?
Weeks 2–4 bring scab shedding, shock loss, and the start of light activity resumption.
The second phase brings visible changes. Patients often feel anxiety as hairs fall. Education prevents panic. This period tests emotional resilience.
What Physiological Changes Happen in Weeks 2–4?
Scabs shed naturally and shock loss causes temporary hair fall.
Physiological changes include scab shedding and shock loss. Scabs detach naturally as skin heals. Shock loss makes transplanted hairs fall out. This process is normal and expected. The follicle remains alive beneath the skin. New shafts will emerge later. Research confirms that shock loss signals follicle cycling rather than failure (Unger and Shapiro 2011). Patients should not fear this stage.
What Care Guidelines Apply in Weeks 2–4?
Patients continue gentle scalp hygiene, avoid picking scabs, and resume light daily activities.
Care guidelines remain simple. Patients continue gentle scalp hygiene. They avoid picking scabs. Picking dislodges grafts and causes scarring. Patients resume light daily activities. They still avoid heavy lifting and intense bending. Sun protection continues. The donor area healing progresses during this time.
What Psychological Considerations Arise During Shedding?
Shedding triggers anxiety, but education and surgeon communication reassure patients.
Psychological considerations matter deeply. Shedding triggers patient anxiety. Many patients fear failure. Surgeons and clinics must manage expectations before surgery. Clear communication reassures patients that shock loss is temporary. Support groups and written guides reduce emotional distress. Long-term satisfaction correlates with adherence and expectation management (Kanti et al. 555).
What Happens During the Dormant Phase and Early Growth?
Months 1–3 bring follicle dormancy, the first new hair emergence, and nutritional optimization.
This phase tests patience. Visible growth remains minimal. Biological activity continues under the surface. The hair transplant aftercare month by month plan shifts focus here.
What Key Developments Occur in Months 1–3?
Follicles rest temporarily, then early new hairs begin emerging around month three.
Key developments include temporary dormancy of follicles. Early new hair emergence begins near month three. Patients may see fine, thin strands. These early hairs lack full pigment and thickness. The anagen restart confirms successful graft survival. Blood supply establishes fully during this period. Donor area healing completes externally.
What Care Protocol Applies in Months 1–3?
Patients optimize nutrition, avoid scalp trauma, limit UV exposure, and may start PRP therapy.
The care protocol shifts toward optimization. Patients focus on nutritional support. Protein, iron, and biotin intake supports keratin synthesis. Patients avoid scalp trauma and UV exposure. Ultraviolet radiation damages healing skin. Some surgeons offer optional adjunct therapies such as PRP. PRP therapy accelerates early growth and strengthens follicles (Gholamali et al. 14).
What Characterizes Active Growth and Density Improvement?
Months 3–6 bring noticeable hair growth, thickening, and up to 50–80% visible results.
This phase rewards patience. Visible changes accelerate. Patients regain confidence. The hair transplant recovery timeline enters its most exciting stage.
What Clinical Observations Define Months 3–6?
Surgeons observe noticeable hair growth, shaft thickening, and 50–80% of final visible density.
Clinical observations include noticeable hair growth and thickening. Up to 50–80% of visible results appear by month six. Hair shafts gain diameter and pigment. The hairline takes shape. Donor area healing completes in most cases. Scars fade and blend with surrounding tissue.
What Care Recommendations Apply in Months 3–6?
Patients gradually return to normal hair routines, trim safely, and continue scalp protection.
Care recommendations allow gradual normalization. Patients return to normal hair routines. They trim and groom safely. Harsh chemicals remain restricted. Continued scalp protection from extreme heat and cold preserves graft health. Regular washing with mild products maintains scalp hygiene.
What Does Maturation and Styling Freedom Involve?
Months 6–12 bring increased thickness, natural hairline formation, and safe use of styling products.
Maturation brings the final aesthetic refinement. Hair behaves like native hair. Patients enjoy new freedom.
What Outcomes Should Patients Expect in Months 6–12?
Patients should expect thicker shafts, a natural hairline, and near-complete density.
Expected outcomes include increased hair shaft thickness. Natural hairline formation completes. Near-complete density becomes visible. The hair gains the texture and direction of native hair. Transplanted hair continues to grow for life because it retains donor-area genetics (Bernstein and Rassman 1997).
What Long-Term Care Applies in Months 6–12?
Long-term care includes safe styling, routine follow-ups, and maintenance medications if needed.
Long-term care allows styling product use. Patients can dye, trim, and shape hair. Routine dermatological follow-ups catch any issues early. Some patients need maintenance therapies. Minoxidil and finasteride preserve native hair and support density (Blume-Peytavi et al. 5). These medications complement the 1-year care plan after hair transplant.
What Defines Final Results and Stabilization?
Month 12+ delivers 90–100% visible results, fully healed areas, and a shift to long-term maintenance.
The final phase confirms success. Evaluation and maintenance take priority. The hair transplant healing stages conclude here.
How Do Surgeons Evaluate Outcomes at Month 12?
Surgeons assess 90–100% visible results and fully healed donor and recipient areas.
Outcome evaluation measures density, coverage, and naturalness. Surgeons expect 90–100% visible results. Donor and recipient areas heal fully. Photography documents before-and-after changes. Patient satisfaction surveys guide future protocol improvements. Graft survival rates determine long-term value (Jimenez et al. 941).
What Long-Term Maintenance Strategy Works Best?
The best strategy combines hair loss prevention for native hair, nutrition, and healthy lifestyle habits.
Long-term maintenance strategy protects native hair. Androgenetic alopecia continues in non-transplanted areas. Patients maintain protein intake and micronutrient levels. They manage stress and sleep. These habits support the longevity of both transplanted and native hair.
What Are the Core Components of an Effective 1-Year Care Plan?

Effective plans include medical management, scalp hygiene, lifestyle changes, nutrition, and adjunctive therapies.
Core components work together across all phases. Neglecting one area weakens overall results. Patients must address each component systematically.
What Medical Management Supports Recovery?
Medical management includes antibiotics, anti-inflammatory drugs, and hair growth medications.
Medical management covers antibiotics and anti-inflammatory drugs. Surgeons prescribe these in the early weeks. Hair growth medications such as finasteride and minoxidil support long-term density. These drugs block dihydrotestosterone and improve follicle blood flow (Kanti et al. 555). Patients take them under medical supervision. Self-medication risks side effects.
What Scalp Care and Hygiene Practices Help Most?
Gentle washing, mild products, and phase-appropriate techniques protect grafts and skin.
Scalp care and hygiene require attention. Patients use washing techniques matched to each phase. Early phases demand cup-rinsing and pat-drying. Later phases allow normal showering. Product selection matters. Patients avoid harsh chemicals early. Sulfates and strong fragrances irritate healing skin. Mild, pH-balanced shampoos support scalp hygiene without damage.
What Lifestyle Modifications Improve Results?
Quitting smoking, limiting alcohol, and following a graded exercise timeline improve graft survival.
Lifestyle modifications produce measurable benefits. Smoking cessation improves blood flow. Alcohol limitation reduces inflammation and bleeding risk. Exercise follows a graded timeline. Patients avoid strenuous activity for one month. Light walking resumes after two weeks. These changes protect graft survival and donor area healing.
What Nutritional Support Fuels Hair Regrowth?
Protein, iron, biotin, zinc, and vitamins D and E fuel hair synthesis and follicle health.
Nutritional support drives hair synthesis. Protein intake provides keratin building blocks. Iron prevents telogen effluvium. Biotin and zinc strengthen shafts. Vitamins D and E reduce oxidative stress. Research links diet quality to hair loss prevention (Guo and Katta 48). Patients who optimize nutrition see faster regrowth. Supplements help when diet falls short.
What Adjunctive Therapies Enhance Outcomes?
PRP therapy and low-level laser therapy (LLLT) enhance growth and density.
Adjunctive therapies offer extra support. PRP therapy injects concentrated platelets into the scalp. Growth factors in PRP stimulate follicle activity (Gholamali et al. 14). Low-level laser therapy (LLLT) improves cellular metabolism. Patients use LLLT devices at home or in clinics. These therapies fit into the 1-year care plan after hair transplant as optional boosters. They do not replace basic care.
What Risks and Complications Threaten Hair Transplant Success?
Infection, folliculitis, and poor graft survival threaten results, but prevention strategies work.
Risks remain low with proper care. Awareness prevents minor issues from becoming major problems. Every patient should know the warning signs.
What Common Issues Affect Transplant Patients?
Common issues include infection, folliculitis, cysts, and poor graft survival.
Common issues include infection and folliculitis. Bacteria enter through tiny wounds. Folliculitis causes pimple-like inflammation around grafts. Poor graft survival results from trauma, smoking, or inadequate post-operative care. Early detection limits damage. Patients must report redness, pus, or excessive pain immediately.
What Prevention Strategies Protect Graft Survival?
Strict adherence to care protocols and early medical intervention prevent complications.
Prevention strategies center on adherence. Patients follow washing, medication, and activity instructions exactly. Early medical intervention catches infection before it spreads. Surgeons prescribe topical or oral antibiotics at the first sign of folliculitis. Patients who call their clinic early avoid serious setbacks. Prevention beats treatment every time.
Why Does Patient Compliance Matter for Psychological Health?
Compliance ensures realistic expectations, reduces anxiety during shock loss, and correlates with long-term satisfaction.
Patient compliance and psychological factors intertwine. Expectation management prevents disappointment. The emotional impact of shock loss hits hard. Patients who understand the timeline handle shedding better. Studies show that adherence to post-operative instructions directly predicts satisfaction at month 12 (Unger and Shapiro 2011). Reassuring communication from the surgical team builds trust. Anxiety drops when patients know what to expect.
What Clinical Follow-Up Schedule Ensures Success?
Surgeons schedule healing checks at 2 weeks, growth monitoring at 3–6 months, and final evaluation at 12 months.
Clinical follow-up schedules create accountability. Surgeons assess healing at 2 weeks. They monitor growth at 3–6 months. They conduct final evaluation at 12 months. These visits allow intervention if growth lags. They also reinforce patient education. The follow-up schedule anchors the 1-year care plan after hair transplant in real clinical oversight.
What Does the Discussion Reveal About Recovery Protocols?
Recovery protocols vary by patient age, hair type, and surgical technique, and emerging trends support regenerative therapies.
Discussion of recovery protocols reveals variability. Different surgeons use slightly different timelines. Patient factors such as age, hair type, and technique modify outcomes. Older patients may heal slower. Curly hair requires different handling. FUE and DHI produce similar long-term results but differ in early care. Emerging trends include regenerative support therapies. Stem cell-derived signals and advanced PRP formulations show promise. Future 1-year care plans after hair transplant may incorporate these innovations routinely. Research continues to refine the hair transplant recovery timeline.
What Conclusions Can We Draw About 1-Year Care Plans?
Structured 1-year care plans determine graft survival and final density; patience, consistency, and medical guidance drive success.
Hair transplant success depends heavily on a structured 1-year care plan. Patience matters. Consistency matters. Medical guidance matters. Future directions include better regenerative support therapies. Patients who commit to the full timeline achieve the best outcomes. The evidence leaves no doubt: aftercare is as important as surgery itself. Post hair transplant care defines the final mirror reflection.
What Frequently Asked Questions Do Patients Have?
Patients commonly ask about recovery duration, shock loss permanence, activity resumption, and styling timelines.
This FAQ section expands on common concerns. It supports semantic SEO and patient education. These questions appear constantly in clinical practice.
How Long Does Full Recovery Take After Hair TransplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by...?
Functional recovery takes 7–10 days; full visible results take 9–12 months.
Functional recovery completes in 7–10 days. Patients return to office work within days. Full visible results require 9–12 months. The 1-year care plan after hair transplant covers this entire span. No shortcut exists.
Is Shock Loss Permanent After Hair Transplantation?
No, shock loss is temporary and part of the natural follicle cycle.
Shock loss is not permanent. It is temporary and part of the natural cycle. New growth replaces shed hairs. Patients must trust the process. Panic helps no one.
When Can Patients Return to Normal Activities?
Light activities resume in 1–2 weeks; exercise resumes around 1 month.
Light activities resume in 1–2 weeks. Exercise resumes around 1 month. Strenuous sports and heavy lifting need the full month. Sun exposure and swimming require similar waits. Patients must respect these timelines.
When Can Patients Safely Cut or Style Their Hair?
Patients can cut and style safely around 6 months onward.
Patients can cut and style safely around 6 months onward. Before that, trimming should stay minimal. Chemical treatments wait until month 12. Natural styling becomes safe once maturation progresses. The hair transplant healing stages dictate these timelines.
Comparison Table: Recovery Phase Overview
|
Phase |
Timeframe |
Primary Goal |
Key Actions |
Restrictions |
|
Immediate Care |
Day 0–7 |
Graft anchoring |
Gentle wash, saline spray, head elevation |
No touching, smoking, alcohol, sun |
|
Early Healing |
Week 2–4 |
Scab resolution |
Continue hygiene, avoid picking scabs |
No heavy exercise, no scratching |
|
Dormancy |
Month 1–3 |
Follicle recovery |
Nutrition, PRP, UV protection |
No harsh chemicals, no trauma |
|
Active Growth |
Month 3–6 |
Density building |
Normal washing, light trimming |
Avoid extreme heat/cold exposure |
|
Maturation |
Month 6–12 |
Thickness and blending |
Styling, follow-ups, maintenance meds |
Minimal restrictions |
|
Stabilization |
Month 12+ |
Final evaluation |
Long-term maintenance, lifestyle |
Ongoing hair loss prevention |
Comparison Table: Nutritional Support for Hair Synthesis
|
Nutrient |
Role in Hair Growth |
Food Sources |
Daily Target |
|
Protein |
Keratin building block |
Eggs, fish, poultry, legumes |
1.2–1.6 g/kg body weight |
|
Iron |
Oxygen delivery to follicles |
Red meat, spinach, lentils |
8–18 mg |
|
Biotin |
Cell growth and keratin production |
Nuts, seeds, eggs |
30–100 mcg |
|
Zinc |
Tissue repair and oil gland function |
Oysters, beef, pumpkin seeds |
8–11 mg |
|
Vitamin D |
Follicle cycling regulation |
Fatty fish, fortified milk |
600–800 IU |
|
Vitamin E |
Antioxidant protection |
Almonds, sunflower seeds |
15 mg |
References
Avram, Marc R., et al. “Hair Transplantation.” JAMA Dermatology, vol. 153, no. 11, 2017, p. 1152.
Bernstein, Robert M., and William R. Rassman. “The Aesthetics of Follicular Transplantation.” Dermatologic Surgery, vol. 23, no. 9, 1997, pp. 785-99.
Blume-Peytavi, Ulrike, et al. “S1 Guideline for Diagnostic Evaluation in Androgenetic Alopecia.” Journal of the German Society of Dermatology, vol. 9, no. S6, 2011, pp. 1-10.
Gholamali, A., et al. “Platelet-Rich Plasma in Hair Transplantation.” Journal of Cutaneous and Aesthetic Surgery, vol. 13, no. 1, 2020, pp. 14-18.
Guo, Emily L., and Rajani Katta. “Diet and Hair Loss.” Journal of Clinical and Aesthetic Dermatology, vol. 10, no. 7, 2017, pp. 48-53.
Jimenez, F., et al. “Morphometric Analysis of Follicular Unit Transplantation.” Dermatologic Surgery, vol. 37, no. 7, 2011, pp. 941-7.
Kanti, V., et al. “Evidence-Based (S3) Guideline for the Treatment of Androgenetic Alopecia.” Journal of the German Society of Dermatology, vol. 16, no. 5, 2018, pp. 555-72.
Rose, Paul T. “Hair Restoration Surgery.” Facial Plastic Surgery Clinics of North America, vol. 21, no. 3, 2013, pp. 317-25.
Trueb, Ralph M. “Association between Smoking and Hair Loss.” International Journal of Trichology, vol. 10, no. 3, 2018, pp. 97-101.
Unger, Walter P., and Ronald Shapiro, editors. Hair Transplantation. 5th ed., Informa Healthcare, 2011.