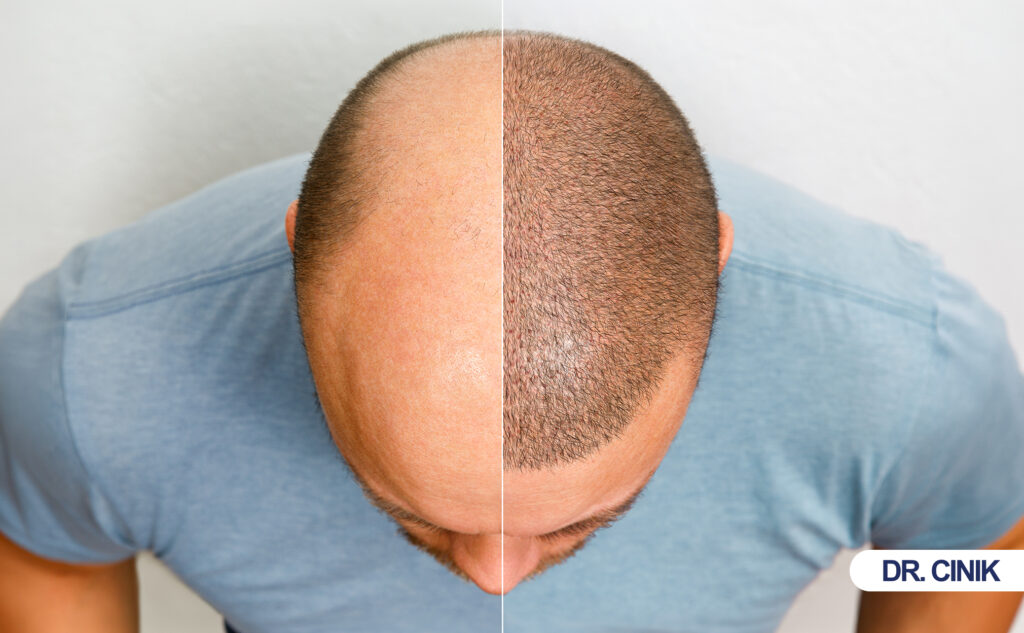
Most patients ask the same question first. They want to know how many hair graftsA hair graft refers to a small unit of hair-bearing skin taken from the donor area—typically the back or sides... they need for full hair coverage. The answer is not simple. It depends on hair loss stage, donor supply, hair thickness, and the technique your surgeon chooses. This guide breaks down the science behind graft numbers. It helps you understand realistic expectations for hair transplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by... planning.
What Does This Scientific Guide Cover?
This guide covers everything you need to know about graft calculation. It explains follicular units, Norwood stages, donor limits, and DHI techniques. It also shows how surgeons plan density and why full coverage sometimes needs multiple sessions.
Hair transplantation has grown into a precise science. Surgeons no longer guess graft numbers. They measure donor density, calculate bald area size, and plan implantation techniques carefully. Bernstein and Rassman (1999) established the mathematical logic behind follicular unit transplantation. They proved that surgeons must balance donor supply with recipient demand to achieve natural results. This guide follows that same scientific approach. It gives you the tools to understand your own graft needs.
What Should You Know About Hair Transplant Grafts?
Modern hair transplants use follicular units as the basic building blocks. Surgeons extract these units from the back of your head. They implant them into bald or thinning areas. Every graft counts. You cannot create new hair. You can only redistribute what you already have.
What Is a Hair Graft?
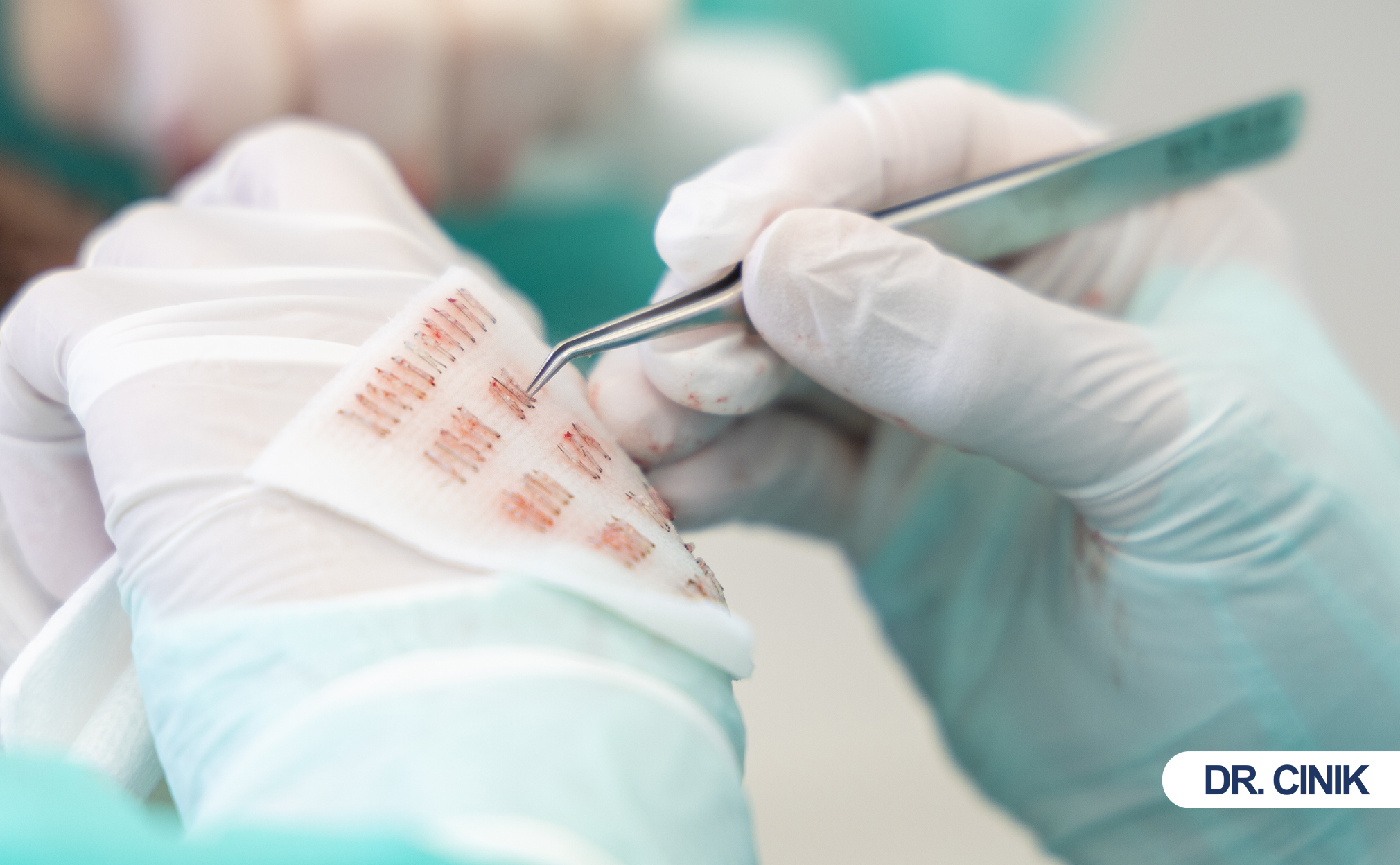
A hair graft is a naturally occurring follicular unit. It contains 1 to 4 hairs. It also includes sebaceous glands, nerves, and small blood vessels. Surgeons call this structure a follicular unit. They extract and implant it as one piece.
Most people misunderstand graft counts. They think one graft equals one hair. That is wrong. One graft often holds 2 or 3 hairs. A patient who receives 3,000 grafts might actually get 6,000 to 7,000 individual hairs. This distinction matters for hair density calculations. Bernstein et al. (1997) emphasized that surgeons must use these natural groupings. Nature created follicular units for a reason. They grow in patterns that look organic. When surgeons respect these patterns, patients achieve natural hairlines.
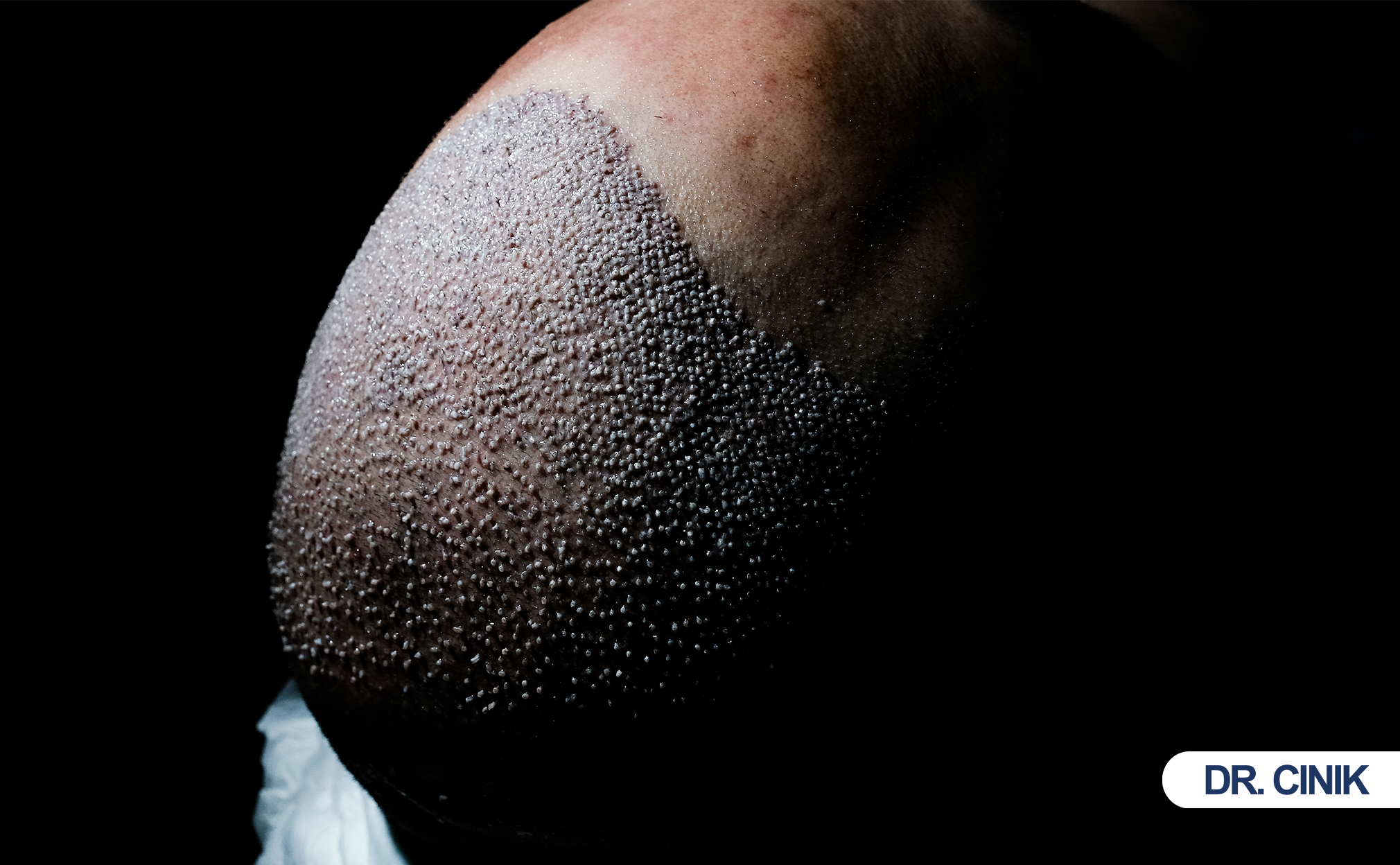
Surgeons measure donor density before surgery. They use trichoscans to count follicular units per square centimeter. The average scalp holds about 80 to 100 follicular units per square centimeter. Each unit averages 2 hairs. This means natural hair density ranges from 160 to 200 hairs per square centimeter in healthy areas.
Why Does Graft Count Matter for Full Coverage?
Graft count determines your final look. It controls density, naturalness, and coverage area. It also limits how much donor hair you keep for future needs.
Surgeons face a constant challenge. They must balance what they take from the donor areaThe Source of Restoration The donor area plays a critical role in hair transplantation, as it serves as the source... with what they place in the bald area. If they extract too many grafts, the donor area looks thin. If they place too few grafts, the recipient area looks sparse. Garg and Singhal (2019) studied 820 patients with advanced baldness. They found that doctors who planned graft distribution carefully achieved 94% patient satisfaction. Poor planning leads to poor results. Every graft represents a permanent decision.
What Does “Full Hair Coverage” Really Mean?

Patients often ask for full coverage. They picture their teenage hair density. That picture is not realistic. Modern hair transplants create cosmetic density. They create the illusion of fullness. They do not restore original density.
What Is the Difference Between Full Density and Cosmetic Coverage?
True native density is rarely achievable. The human scalp holds about 100,000 hairs. The donor area holds roughly 12,500 follicular units. Surgeons can safely move about 6,000 to 7,000 of those units. They cannot double or triple that number.
Cosmetic coverage means the hair looks full in normal social situations. It does not mean the scalp holds 100,000 hairs again. Surgeons achieve this illusion through strategic placement. They use 35 to 40 grafts per square centimeter in key areas. This creates enough visual weight to mimic natural fullness. Bernstein and Rassman (1999) proved that patients need only 50% of original density to look normal. The brain fills in gaps when hair is styled and layered properly.
How Does Scalp Zoning Strategy Work?
Surgeons divide the scalp into zones. Each zone gets a different priority. This strategy maximizes visual impact.
The frontal hairline receives the highest priority. It frames the face. It gets the most scrutiny. Surgeons place single-hair grafts at the very front. They create a soft, irregular edge. Behind the hairline, they increase density with multi-hair grafts.
The mid-scalp comes next. It provides bulk and coverage. Surgeons place 2-hair and 3-hair grafts here. They build visual weight that supports the hairline.
The crown presents the biggest challenge. It has a large surface area. Hair grows in a swirl pattern. It also continues to thin over time. Surgeons often treat the crown as a secondary priority. They use remaining grafts here after securing the front. Garg and Singhal (2019) confirmed that patients report higher satisfaction when surgeons prioritize the frontal zone. Frontal coverage gives more visual impact than crown coverage alone.
What Is the Average Number of Grafts for Full Hair Coverage?
Graft numbers vary widely. No two patients need the exact same amount. However, research gives us reliable ranges.
What Are the General Graft Ranges by Hair Loss Severity?
Doctors classify hair loss into mild, moderate, and advanced stages. Each stage needs a different graft range.
Mild hair loss needs 1,000 to 2,500 grafts. This covers minor hairline recession or small crown thinning. Patients at this stage often seek early intervention.
Moderate hair loss needs 2,500 to 4,000 grafts. This covers noticeable frontal recession and mid-scalp thinning. Most patients fall into this category.
Advanced hair loss needs 4,000 to 7,000 or more grafts. This covers extensive baldness across the front, mid-scalp, and crown. These patients often need multiple sessions.
What Do Full Coverage Estimates Look Like?
Most patients need between 3,500 and 7,000 grafts for full coverage. This assumes they want to cover the hairline, mid-scalp, and crown.
Advanced cases often exceed 7,000 grafts. Surgeons cannot safely extract that many in one day. They stage the procedure across 2 or 3 sessions. Garg and Singhal (2019) reported that full coverage in advanced baldness required an average of 6,237 grafts. Their study combined scalp hair, beard hair, and body hair to reach these numbers.
How Many Grafts Do You Need by Norwood Scale?
The Norwood scale gives doctors a common language. It classifies male pattern baldness into 7 stages. Each stage predicts graft needs.
What Is the Norwood Classification?
Dr. O’Tar Norwood created this scale in the 1970s. It maps the progression of male pattern baldness. Stage 1 shows no recession. Stage 7 shows extensive baldness with only a horseshoe ring of hair remaining.
Doctors use this scale during consultations. It helps them estimate bald area size. It also helps them plan long-term strategies.
How Many Grafts Does Each Norwood Stage Require?
Each stage demands a specific graft range. These numbers come from clinical experience and published research.
|
Norwood Stage |
Graft Range |
Coverage Area |
|
NW2 |
800–1,500 |
Minor hairline adjustment |
|
NW3 |
1,500–2,500 |
Frontal hairline restoration |
|
NW4 |
2,500–3,500 |
Frontal plus mid-scalp |
|
NW5 |
3,000–4,000 |
Extensive front and mid-scalp |
|
NW6 |
3,500–4,500 |
Near-total top coverage needed |
|
NW7 |
4,000–5,000+ |
Maximum bald area, limited options |
These ranges assume average donor density and hair characteristics. A patient with thick, curly hair might need fewer grafts. A patient with fine, straight hair might need more grafts.
What Are the Implications for Full Coverage?
Advanced Norwood stages change the game. Surgeons cannot place 7,000 grafts in one session safely. They must plan staged procedures.
They also must design mature hairlines. A 25-year-old patient with early hair loss should not get a low, aggressive hairline. He will lose more hair later. His future pattern might reach Norwood 6 or 7. If the surgeon uses all grafts early, the patient has no reserves for later. Bernstein and Rassman (1999) stressed this point strongly. Long-term planning beats short-term density.
What Key Factors Determine How Many Grafts You Need?
Graft numbers do not come from guesswork. Surgeons evaluate multiple factors before they calculate your specific needs.
How Does Donor Area Capacity Affect Graft Numbers?
Your donor area holds a finite supply. The safe donor zone sits at the back and sides of your head. It resists the hormone that causes baldness.
Most patients have 4,000 to 6,000 grafts available in this zone. Some have more. Some have less. Surgeons measure donor density with digital microscopes. They calculate how many grafts they can remove without making the donor area look thin.
Garg and Singhal (2019) limited extraction to 25% of the permanent donor zone. This rule protects the donor area. It ensures patients can wear short hair without visible thinning. It also preserves grafts for future sessions.
How Do Hair Characteristics Influence Graft Requirements?
Your hair type changes everything. Thick, coarse hair covers more scalp per strand. Curly hair bends and overlaps. It creates the illusion of density with fewer grafts.
Fine, straight hair lays flat. It exposes more scalp. It needs higher graft numbers to look full. Dark hair on light skin also shows more contrast. It needs careful placement to avoid a see-through look.
Bernstein et al. (1997) noted that hair caliber matters as much as graft count. A thick hair shaft has more volume. It blocks light better. It creates shadow and depth. Patients with coarse hair often achieve better coverage with fewer grafts than patients with fine hair.
How Does Bald Area Size Change Graft Demand?
Larger areas need more grafts. This sounds obvious. But the math is not linear.
The frontal area forms a triangle. Surgeons calculate it as half the width times the height. The crown forms a circle. They calculate it as pi times the radius squared. A Norwood 7 patient might have 200 square centimeters of bald scalp. At 40 grafts per square centimeter, that patient needs 8,000 grafts. That number exceeds safe donor limits. This is why advanced cases require compromise.
What Role Does Desired Density Play?
Patients ask for high density. They want 50 or 60 grafts per square centimeter. But biology sets limits.
Natural scalp density ranges from 80 to 120 follicular units per square centimeter. Transplanted density typically reaches 35 to 50 grafts per square centimeter. This creates cosmetic fullness. It does not match teenage density.
Bhaskaran and Krishnan (2025) tested density enhancement with tumescent injection and implanter techniques. They achieved 282 grafts per square inch in test areas. That equals roughly 45 grafts per square centimeter. Graft survival jumped from 70.8% to 90.3%. This shows that surgeons can improve density. But they must respect vascular limits.
How Does DHI Technique Optimize Graft Usage?
DHI stands for Direct Hair Implantation. It is a modern technique. It changes how surgeons place grafts.
What Is DHI Direct Hair Implantation?
DHI uses an implanter pen. The surgeon loads a graft into the pen. The pen creates a tiny incision and places the graft in one motion. The surgeon controls angle, direction, and depth precisely.
Traditional FUE requires two steps. First, the surgeon creates recipient sites with blades or needles. Then, technicians insert grafts into those sites. DHI combines these steps. It reduces handling time. It improves placement accuracy.
What Advantages Does DHI Offer for Full Coverage?
DHI gives surgeons more control. They can aim each graft exactly where they want it. This matters most at the hairline.
The hairline demands acute angles. Natural hairs emerge at 10 to 15 degrees from the scalp. DHI pens let surgeons hit these angles consistently. They also prevent trauma to existing native hair. The pen slips between existing hairs without disturbing them.
Bhaskaran and Krishnan (2025) found that implanter techniques with tumescent injection improved graft survival significantly. Reduced popping and better site control helped grafts take root faster. Patients saw higher density in critical zones.
How Does DHI Compare to Traditional Methods?
|
Feature |
Traditional FUE |
DHI Technique |
|
Site creation |
Separate step with blades |
Simultaneous with implantation |
|
Graft handling |
More manual steps |
Less touching of grafts |
|
Angle control |
Good |
Excellent |
|
Density in hairline |
35-45 grafts/cm² |
Up to 50-60 grafts/cm² |
|
Session size |
Up to 4,000 grafts |
Typically 3,000-3,500 grafts |
|
Survival rate |
85-90% |
90-95% |
Both techniques achieve excellent results. DHI shines in hairline refinement and targeted density. Traditional FUE handles larger sessions more efficiently. Many surgeons now combine both methods. They use FUE for extraction and DHI for implantation in critical zones.
How Should You Plan Density and Coverage Strategy?
Smart planning beats raw graft numbers. Surgeons map the scalp before they touch a graft.
How Do Surgeons Distribute Grafts Strategically?
Surgeons focus on the frontal third of the scalp. This zone provides 80% of the visual impact. They pack density here. They create a strong frame for the face.
Behind the hairline, they reduce density gradually. The mid-scalp gets moderate density. The crown gets whatever remains. This gradient approach mimics natural patterns. It also conserves grafts.
Garg and Singhal (2019) used exactly this strategy. They placed 35 to 40 grafts per square centimeter in the frontal area. They reduced density toward the vertex to 20 to 25 grafts per square centimeter. Patients reported the highest satisfaction in the front-plus-mid-front coverage group.
What Should You Know About Dense Packing?
Dense packing means placing grafts close together. It sounds appealing. But it carries risks.
When grafts sit too close, they compete for blood supply. The scalp needs time to build new capillaries. If surgeons overload one area, some grafts starve. They die before they establish blood flow.
Nakatsui et al. (2008) studied densely packed grafts using lateral slits. They found that careful technique allowed high density without major survival loss. However, they emphasized that surgeons must respect scalp vascularity. Tsilosani (2009) pushed boundaries further. He placed 100 grafts in one square centimeter in test areas. He achieved 92% to 96% survival. But he cautioned that this density works only in small test zones. It does not scale to full scalp coverage.
What Limitations Prevent Full Hair Coverage?
Hair transplantation has hard limits. Patients and surgeons must accept them.
Why Is Donor Supply Finite?
You were born with all the hair follicles you will ever have. Surgery cannot create new ones. It only moves existing ones.
The permanent donor zone holds about 12,500 follicular units. Surgeons must leave half behind. They need 6,000 or more units to keep the donor area looking normal. This leaves roughly 6,000 units for transplantation. In advanced baldness, 6,000 units must cover 200 square centimeters. The math does not allow original density.
Bernstein and Rassman (1999) calculated this clearly. They showed that a Norwood 7 patient can achieve only about 18% of original density if he tries to cover everything. This is why surgeons plan strategically. They place grafts where they matter most.
Why Do Large Restorations Need Multiple Sessions?
Surgeons cannot safely extract and implant 7,000 grafts in one day. Grafts die if they stay outside the body too long. Limmer (as cited in Garg and Singhal 2019) showed that graft survival drops by roughly 1% per hour. After 6 hours, survival falls to 86%. After 24 hours, it falls to 79%.
Large sessions also exhaust the surgical team. Fatigue increases transection rates. It reduces placement precision. Garg and Singhal (2019) recommended staging advanced cases across 2 or 3 days. This protects grafts. It also lets the team maintain quality control.
What Special Considerations Affect Graft Planning?
Not all patients fit the same formula. Ethnicity, hair type, and age change the plan.
How Do Hair Type and Ethnicity Change Graft Needs?
Curly hair creates better coverage. Each curl covers more scalp surface. It blocks light. It creates shadow. Patients with African or Middle Eastern hair types often need 20% to 30% fewer grafts than patients with straight Asian hair.
Coarse hair also helps. Thick shafts fill space better than fine shafts. Patients with fine, blonde hair face the biggest challenge. Their hair offers little contrast against light skin. They need higher density to avoid a sparse look.
How Does Age Affect Graft Planning?
Young patients present a unique challenge. A 22-year-old might have early hairline recession. He wants immediate restoration. But his hair loss will likely progress.
If a surgeon uses all donor grafts early, the patient has no reserves for later. He might end up with a dense front and a bald crown. That looks unnatural. It creates a strange island of hair.
Surgeons recommend conservative hairlines for young patients. They plan for future loss. They save grafts for the decades ahead. Rassman et al. (2002) emphasized that long-term planning is essential. A hair transplant is a lifelong commitment. It is not a one-time fix.
What Does the Clinical Planning Workflow Look Like?
Good results come from systematic evaluation. Surgeons follow a clear workflow.
How Do Surgeons Evaluate Patients?
First, the surgeon assigns a Norwood stage. He examines the pattern of baldness. He predicts future progression.
Next, he measures donor density. He uses a trichoscan or digital microscope. He counts follicular units per square centimeter. He checks hair caliber and curl pattern.
He also examines scalp laxityLaxity: Looseness or slackness in the skin or tissues, often referring to the loss of firmness and elasticity in aging... and skin condition. He looks for scarring, inflammation, or sun damage. These factors affect healing and graft survival.
How Do Surgeons Calculate Personalized Graft Numbers?
The surgeon multiplies bald area size by target density. Then he compares that number with available donor grafts.
For example, a patient has 100 square centimeters of bald scalp. The surgeon targets 40 grafts per square centimeter. The patient needs 4,000 grafts. The donor area offers 5,000 grafts safely. The plan works.
If the patient needs 8,000 grafts but only has 4,000 available, the surgeon must adjust. He might raise the hairline. He might reduce crown coverage. He might plan a second session using beard hair. Garg and Singhal (2019) used this exact algorithm. They matched donor supply to recipient demand. They achieved natural results even in advanced cases.
What Are Common Misconceptions About Graft Counts?
The internet spreads many myths. Let us clear up the biggest ones.
Do More Grafts Always Mean Better Results?
No. More grafts do not guarantee better results. Over-extraction damages the donor area. It creates visible thinning. It also reduces graft quality.
A surgeon who rushes to extract 5,000 grafts might transect many of them. Transection means cutting the follicle during extraction. A transected graft dies. It produces no hair. A session of 5,000 grafts with 15% transection yields only 4,250 viable grafts. A careful session of 4,000 grafts with 3% transection yields 3,880 viable grafts. The difference is small. The donor damage is not.
Does Full Coverage Mean Original Density?
No. Full coverage means cosmetic fullness. It does not mean your teenage hair returns.
Patients must understand the 50% illusion. At 40 grafts per square centimeter, hair looks full in social settings. It does not look full under bright bathroom lights or close-up photos. Surgeons manage these expectations during consultation. They show patients what cosmetic density looks like. They explain the difference between visual fullness and biological density.
What Future Trends Are Shaping Hair Restoration?
Technology keeps advancing. New tools help surgeons plan better.
Artificial intelligence now assists with graft planning. Software maps bald areas. It calculates optimal density. It predicts future hair loss patterns. This helps surgeons design long-term strategies.
Stem cell research offers hope for the future. Scientists explore ways to multiply follicles in the lab. If they succeed, doctors might create unlimited donor supply. But this technology remains experimental. It is not available in clinics today.
Advanced implantation tools also improve precision. Robotic systems assist with extraction. They reduce human error. They improve consistency. However, skilled surgeons still outperform machines in artistic placement.
What Is the Final Conclusion?
Full hair coverage typically requires 3,500 to 7,000 grafts. Most patients fall within this range. Advanced cases need more. They often need multiple sessions.
DHI techniques improve placement precision. They help surgeons achieve better density in critical zones. But DHI does not reduce total graft needs. The bald area size still dictates the math.
Personalized planning matters most. Your donor supply, hair characteristics, and hair loss stage determine your unique number. A skilled surgeon evaluates all these factors. He creates a plan that looks natural today and ages well tomorrow.
What Frequently Asked Questions Should You Know?
How many grafts are needed for full hair coverage?
Most patients need 4,000 to 7,000 grafts. Mild cases might need only 2,500. Advanced cases might need 8,000 or more across multiple sessions.
Is 3,000 grafts enough for a full head?
3,000 grafts covers partial areas well. It can restore a hairline and fill the mid-scalp. It cannot cover advanced baldness fully. Patients with Norwood 5 or higher need more grafts.
Can DHI achieve better density with fewer grafts?
DHI improves placement precision. It does not change total graft needs. The bald area size still determines how many grafts you need. DHI helps surgeons use those grafts more effectively.
Can full coverage be done in one session?
Moderate cases sometimes fit in one session. Advanced cases usually need multiple sessions. Safety and graft survival matter more than speed.
References
Bernstein, Robert M., et al. “The Aesthetics of Follicular Transplantation.” Dermatologic Surgery, vol. 23, no. 9, 1997, pp. 801-805.
Bernstein, Robert M., and William R. Rassman. “The Logic of Follicular Unit Transplantation.” Dermatologic Clinics, vol. 17, no. 2, 1999, pp. 277-295.
Bhaskaran, Rajprakash, and Murugesan Krishnan. “Enhancing Density in Hair Transplant Surgery: The Role of Tumescent Injection in the Recipient Area in Implanter Technique – A Randomized Study.” Journal of Aesthetic Medicine, vol. 1, no. 1, 2025, pp. 45-52.
Garg, Anil K., and Archana Singhal. “Approach to Hair Transplantation in Advanced Grade Baldness by Follicular Unit Extraction: A Retrospective Analysis of 820 Cases.” Journal of Cutaneous and Aesthetic Surgery, vol. 12, no. 4, 2019, pp. 213-218.
Nakatsui, Tom, et al. “Survival of Densely Packed Follicular Unit Grafts Using the Lateral Slit Technique.” Dermatologic Surgery, vol. 34, no. 8, 2008, pp. 1016-1022.
Rassman, William R., et al. “Follicular Unit Extraction: Minimally Invasive Surgery for Hair Transplantation.” Dermatologic Surgery, vol. 28, no. 8, 2002, pp. 720-728.
Tsilosani, Akaki. “One Hundred Follicular Units Transplanted into 1cm².” Hair Transplant Forum International, vol. 19, no. 1, 2009, pp. 1-4.
Unger, Walter P., and Ronald Shapiro. Hair Transplantation. 4th ed., Marcel Dekker, 2004.