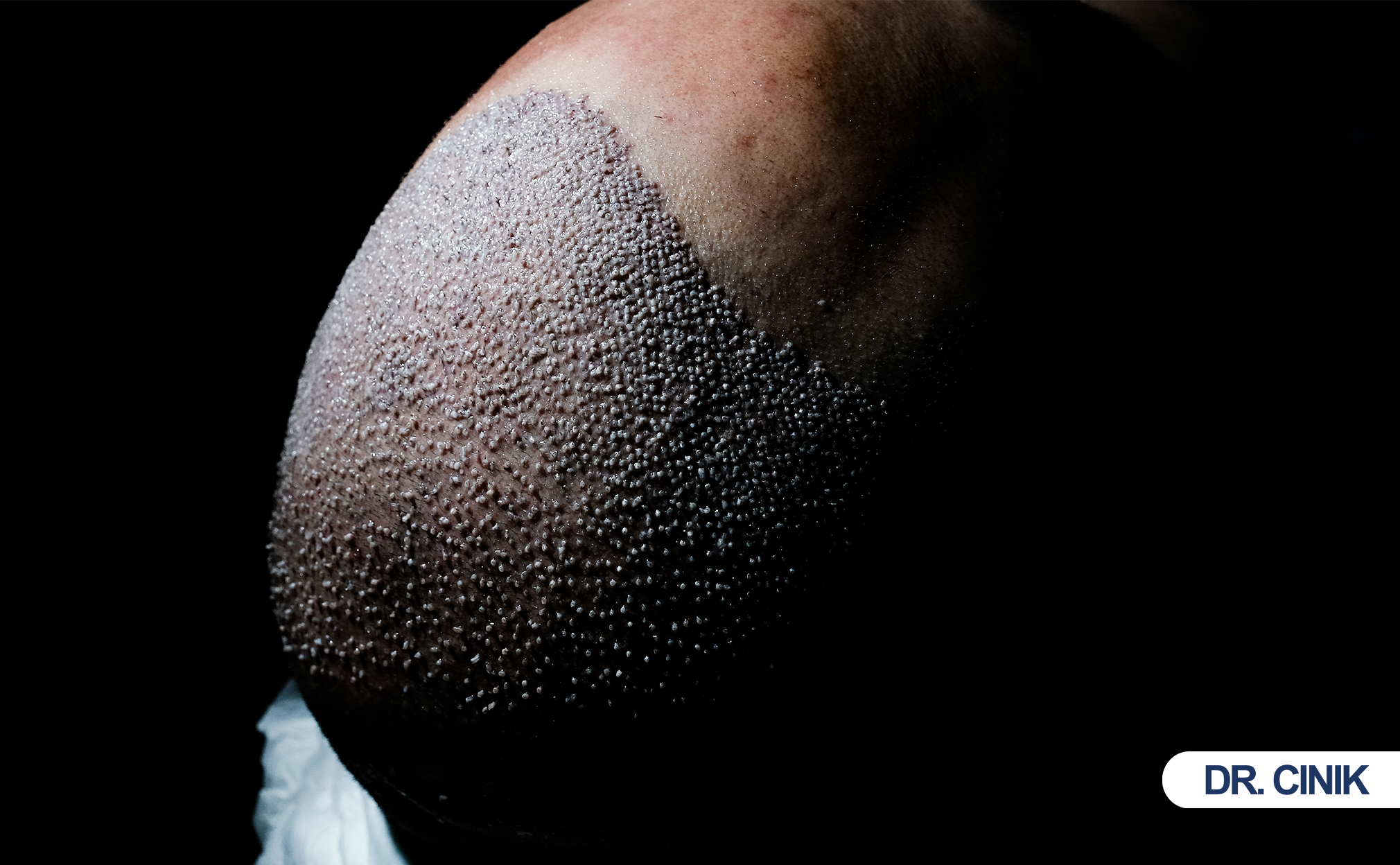
Your skin type directly controls healing speed, infection risk, and graft survival after FUE or DHI surgery. Oily scalps heal fast but face folliculitis risk. Dry scalps heal slowly and retain scabs longer. Thick, thin, and scarred skin each present unique challenges that demand personalized aftercare.
Hair transplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by... moves healthy follicles from donor areas to bald areas. Surgeons create thousands of micro-wounds in the scalp during this process. These wounds must heal perfectly for grafts to survive. Most patients focus on graft count and surgical technique. However, skin physiology plays an equally critical role. Sebaceous glands produce sebum. Blood vessels deliver oxygen. CollagenA structural protein found in the skin and other connective tissues, which is responsible for skin firmness and elasticity.... fibers provide structure. These biological factors vary by skin type. They determine how quickly scabs fall off, how firmly grafts anchor, and how soon new hair emerges. Romera de Blas et al. (2024) confirm that patient-related factors such as scalp condition and skin type significantly influence complication rates after follicular unit excision. This article evaluates how oily, dry, thick, thin, and scarred skin alters every stage of hair transplant healing.
What Is Hair Transplantation and Why Does Skin Type Matter?
Hair transplantation moves healthy follicles from donor areas to bald areas. Surgeons create thousands of micro-channels in the scalp. Your skin type determines how these wounds close, how grafts anchor, and how quickly you recover.
FUE extracts individual follicular units using tiny punches. DHI implants grafts directly with a specialized pen. Both techniques create controlled wounds in the epidermis and dermis. The scalp acts as the biological environment for these grafts. Sebaceous glands secrete sebum. Blood capillaries deliver nutrients. Collagen networks provide physical support. When skin type changes, these elements change too. Oily skin overproduces sebum. Dry skin lacks moisture. Thick skin resists needles. Thin skin tears easily. Scarred skin lacks blood flow. These variations alter wound healing phases. They change infection risk. They modify graft survival rates. Bernstein and Rassman (2000) established that recipient area health directly supports graft survival. Therefore, surgeons must assess skin type before surgery.
How Does Hair Transplantation Work as a Controlled Wounding Procedure?
FUE and DHI deliberately create tiny wounds in the scalp. These wounds trigger the body’s natural repair system. The surgeon controls wound size, depth, and density to maximize graft survival.
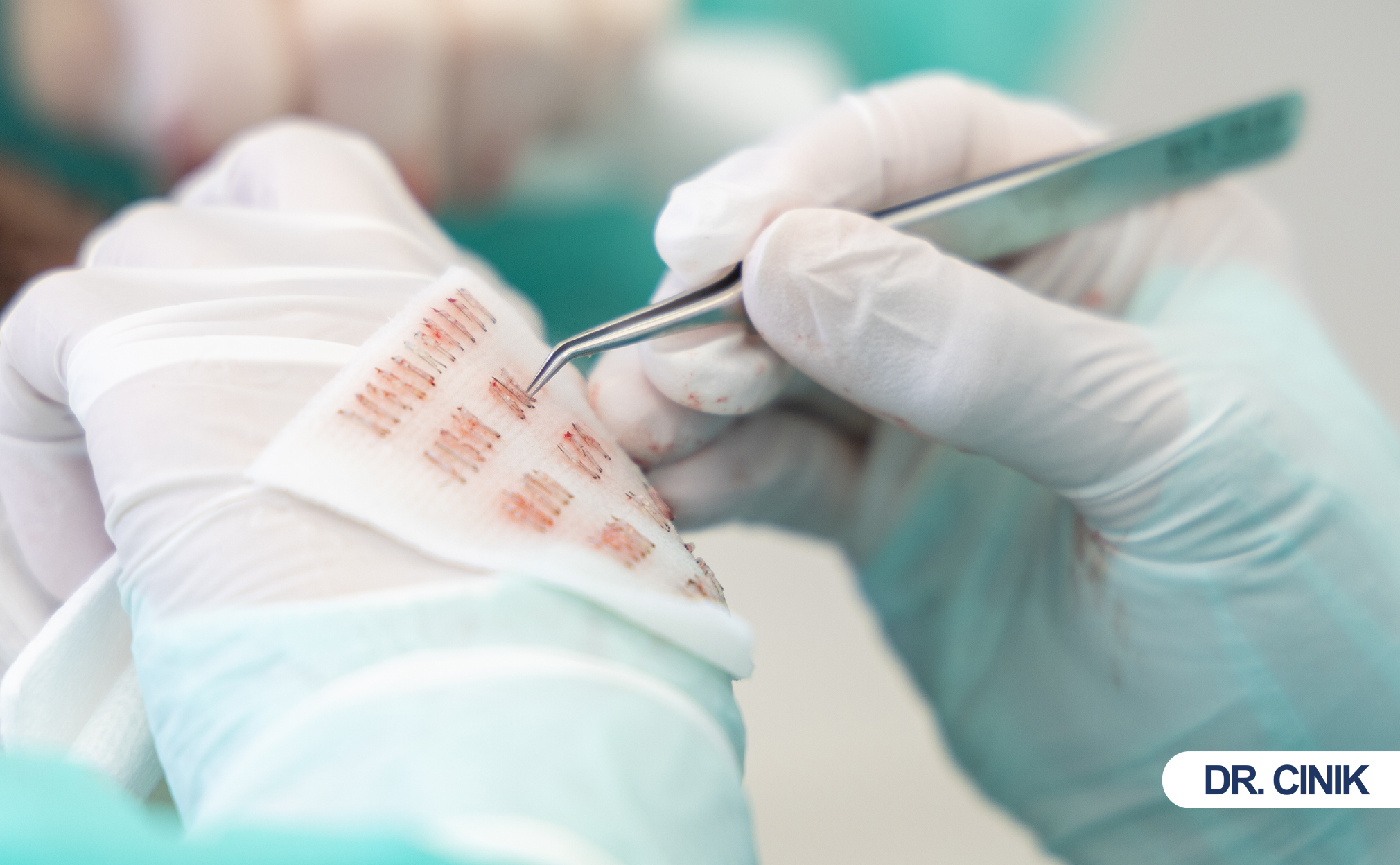
During FUE, the surgeon uses a punch tool to score the skin around each follicular unit. This action severs tiny blood vessels and nerve endings. During DHI, the surgeon loads grafts into a Choi implanter and inserts them into premade or simultaneous slits. Each incision disrupts the epidermis and reaches into the dermis. The body responds immediately. Platelets release clotting factors. Growth factors flood the area. Inflammatory cells migrate to the wound. This sequence constitutes normal healing. However, skin thickness determines incision difficulty. Sebum levels affect bacterial load. Hydration status controls scab formation. These factors explain why two patients with identical graft counts experience different recoveries.
Why Do Surgeons Overlook Skin Type During Consultation?
Many surgeons focus on graft count and technique while ignoring scalp physiology. This oversight increases complication rates and reduces patient satisfaction.
Standard protocols treat all scalps equally. Clinics issue the same shampoo and lotion to every patient. They recommend identical washing schedules. This approach ignores biological reality. Oily scalps need more frequent cleansing. Dry scalps need intensive moisture. Sensitive scalps need hypoallergenic products. Romera de Blas et al. (2024) note that both patient-related factors and technical variables influence complication development. When clinics ignore skin type, they raise the risk of folliculitis in oily patients. They increase scabbing in dry patients. They cause trauma in thin-skinned patients. Personalized assessment prevents these problems.
What Does the Research Say About Personalized Post-Operative Care?
Recent studies prove that tailored aftercare based on skin type reduces complications and improves graft survival. Clinics now recognize that one-size-fits-all protocols fail many patients.
Khatib et al. (2025) performed a systematic literature review and meta-analysis of hair transplantation complications. They found that proper preoperative assessment and meticulous technique remain essential to minimize adverse events. Kerure and Patwardhan (2018) documented that complications such as infection, poor growth, and prolonged erythema often stem from mismatched aftercare. When clinics adjust cleansing frequency, product selection, and hydration protocols to match skin type, patients experience fewer complications. Grafts survive at higher rates. Healing timelines shorten. Patient satisfaction rises.
What Are the Phases of Wound Healing in Hair Transplantation?

Wound healing follows four phases: hemostasis, inflammation, proliferation, and remodeling. Each phase interacts with skin type to determine recovery speed.
The scalp undergoes the same biological repair process as any other wounded tissue. However, the presence of thousands of simultaneous micro-wounds makes hair transplantation unique. Each graft site must heal individually. Each follicle must establish a new blood supply. Skin type modifies every phase. Oily skin accelerates some steps. Dry skin delays others. Scarred tissue blocks progress entirely. Understanding these phases helps patients appreciate why their aftercare must match their skin.
How Does Hemostasis Begin After FUE or DHI?
Blood platelets clot within minutes of incision. This stops bleeding and releases growth factors. Oily skin may bleed less due to thicker dermis. Thin skin bleeds more freely.
Immediately after the surgeon creates recipient sites, blood contacts collagen in the dermis. This contact activates platelets. Platelets stick together and form plugs. They release platelet-derived growth factor and transforming growth factor beta. These signals call other cells to the wound. Oily scalps often possess thicker dermis. This density sometimes reduces initial bleeding. Thin scalps lack this padding. Blood vessels sit closer to the surface. These patients experience more oozing. Surgeons must control this bleeding carefully. Excess blood forms thick crusts. Thick crusts block oxygen. They increase scab duration.
What Happens During the Inflammation Phase?
White blood cells rush to the wound site. They clear debris and fight bacteria. Oily scalps face higher bacterial growth. Dry scalps show prolonged redness.
Neutrophils arrive first. They engulf bacteria and dead tissue. Macrophages follow within 24 to 48 hours. They secrete cytokines and growth factors. These chemicals regulate the entire repair process. In oily scalps, abundant sebum feeds bacteria. Staphylococcus aureus and other microbes multiply quickly. This raises infection risk. It increases folliculitis probability. In dry scalps, inflammation persists longer. The skin barrier remains weak. Irritants penetrate easily. Redness lingers for weeks. Patients with seborrheic dermatitis face even greater inflammation. Romera de Blas et al. (2024) identify preexisting seborrheic dermatitis as a risk factor for postoperative pruritus and inflammation.
How Does Proliferation Rebuild Scalp Tissue?
New cells multiply and form fresh tissue. Fibroblasts create collagen. Keratinocytes resurface the epidermis. Skin thickness determines how quickly this occurs.
During proliferation, fibroblasts migrate into the wound bed. They synthesize type III collagen. This collagen provides temporary strength. Keratinocytes crawl across the wound surface. They restore the epidermal barrier. In thick scalps, abundant fibroblasts accelerate this process. In thin scalps, fewer cells participate. Healing slows slightly. In scarred scalps, fibroblasts produce disorganized collagen. This creates dense, poorly vascularized tissue. Grafts struggle to establish roots in this environment. Healthy proliferation requires adequate hydration. Gandelman et al. (2000) demonstrated that dehydration severely damages follicular unit grafts. This finding underscores why dry scalps need extra moisture during this phase.
Why Does Remodeling Determine Final Aesthetic Outcomes?
Collagen reorganizes and matures over months. Scarred skin remodels poorly. Thick skin produces dense collagen. This phase sets the final appearance.
Remodeling begins around three weeks after surgery. It continues for 12 to 18 months. During this time, type III collagen converts to type I collagen. Cross-linking increases. Tensile strength improves. The wound matures into its final form. In thick, healthy scalps, remodeling produces strong, elastic tissue. Grafts sit securely. In scarred scalps, remodeling creates rigid, avascular plaques. Hair growth looks patchy. In oily scalps, excess sebum may delay collagen maturation slightly. However, the abundant tissue usually compensates. Patients see final results around month 12. Skin type heavily influences whether those results look natural and dense.
How Do Dermatologists Classify Scalp Skin Types?
Dermatologists classify scalp skin into five types: oily, dry, thick, thin, and scarred. Each type carries distinct biological traits that alter healing.
Classification allows targeted treatment. It guides surgical planning. It shapes aftercare protocols. Surgeons assess sebum production, skin thickness, elasticity, and vascularity during preoperative exams. They palpate the scalp. They observe pore size. They check for flakes, redness, or scars. This evaluation takes only minutes. Yet it transforms patient outcomes.
What Defines an Oily or Seborrheic Scalp?
Oily scalps overproduce sebum. Sebaceous glands remain hyperactive. This creates a lipid-rich barrier that resists dehydration but traps bacteria.
Sebaceous glands sit next to hair follicles. They release sebum through the same duct that delivers the hair shaft. In oily scalps, these glands produce excessive lipid material. The scalp looks shiny. Pores appear enlarged. Hair clumps together. This sebum forms a protective acid mantle. It slows moisture loss. However, it also creates a warm, occlusive environment. Bacteria thrive here. After surgery, this bacterial load threatens grafts. Surgeons must balance the benefits of rapid healing against the risks of infection.
What Characterizes a Dry or Xerotic Scalp?
Dry scalps underproduce sebum. They lack moisture retention. The barrier function weakens. Cracks and flakes appear easily.
Xerotic skin contains fewer natural lipids. The stratum corneum loses water quickly. The scalp feels tight. Itch sensations dominate. Flaking resembles dandruff but stems from dehydration, not fungus. After FUE or DHI, this dryness intensifies. The trauma strips remaining lipids. Crusts form rapidly. They adhere tightly to the wound bed. Without moisture, they do not soften. They block oxygen. They prolong inflammation. Patients scratch. Scratching dislodges grafts. Dry scalps demand aggressive hydration from day one.
How Does Thick or Fibrotic Scalp Tissue Differ?
Thick scalps contain dense collagen and abundant tissue. They resist needle penetration. They hold grafts firmly but challenge insertion.
Dermal thickness varies by genetics, age, and sex. Men often possess thicker scalp skin than women. Certain ethnic groups develop denser collagen networks. This thickness provides excellent graft anchoring. Grafts sit deep and stable. However, thick skin requires more force during site creation. Surgeons must use larger blades or sharper punches. They must apply greater pressure. This increases transection risk. It also causes more tissue displacement. Postoperative swelling may last longer. Yet the final density often rewards these challenges.
Why Is Thin or Sensitive Scalp More Fragile?
Thin scalps possess minimal dermal padding. Blood vessels sit closer to the surface. The tissue tears easily under mechanical stress.
Sensitive scalps measure less than 2 millimeters in thickness. The dermis contains sparse collagen. The subcutaneous layer offers little cushioning. During surgery, needles penetrate too deeply easily. They damage underlying structures. Bleeding obscures the surgical field. Grafts sit precariously in shallow beds. Any trauma dislodges them. These patients need minimally invasive techniques. DHI often suits them because it reduces handling. Surgeons must use smaller instruments. They must implant at shallower angles.
What Challenges Does Scarred or Compromised Scalp Present?
Scarred tissue lacks normal blood vessels. It carries fibrotic bands. Regenerative capacity drops significantly.
Previous surgeries, burns, or inflammatory diseases destroy normal scalp architecture. Collagen becomes disorganized. Blood vessels disappear. The scalp feels hard and inelastic. Creating recipient sites proves difficult. The tissue does not stretch. Bleeding remains minimal because vessels are gone. This absence of blood flow starves grafts. Follicles need oxygen and nutrients. Scarred tissue delivers neither. Surgeons must assess vascularity before operating. They may use Doppler imaging. They may recommend PRP or vascular stimulation first. Graft survival in scarred areas often falls below survival in virgin scalp.
How Does an Oily Scalp Influence Hair Transplant Healing?
Oily scalps heal at moderate-to-fast speed. They shed scabs by day 8 to 10. However, excess sebum clogs follicles and triggers folliculitis.
Sebum dominates the postoperative course. It softens crusts. It lubricates the wound surface. It accelerates epithelial migration. These benefits speed visible recovery. Yet the same lipid layer traps bacteria. It occludes follicular openings. It causes pustules. Surgeons and patients must manage this dual nature carefully.
Why Does Sebum Overproduction Occur After Surgery?
Surgery triggers a rebound effect. Sebaceous glands compensate for trauma by increasing output. This overproduction peaks during the first week.
The trauma of punching and implantation disrupts local homeostasis. Sebaceous glands detect this disruption. They increase secretion as a protective response. This phenomenon resembles rebound oiliness seen after aggressive face washing. Patients notice their scalp becomes greasier than usual by day 3 or 4. This oiliness softens scabs. It helps natural detachment. However, it also mixes with blood and exudate. It forms a paste-like residue. This residue blocks follicular ostia. It creates a breeding ground for Staphylococcus aureus.
What Advantages Does Oily Skin Offer for Graft Anchoring?
Oily skin tends to run thicker and more elastic. This density provides a sturdy bed for grafts. Grafts anchor firmly during the critical first week.
Thicker dermis contains more collagen and elastinElastin A protein in connective tissue that allows tissues to resume their shape after stretching or contracting, contributing to skin.... These proteins grip grafts tightly. The graft sits in a snug pocket. It does not shift during sleep or washing. This stability protects the fragile new blood supply. Grafts in thick, oily skin survive at higher rates than grafts in thin, dry skin. The lipid layer also reduces water loss. It keeps the wound environment moist. Moisture supports cell migration. It prevents desiccation. These advantages explain why oily scalps often show faster early growth.
How Does Folliculitis Threaten Oily Scalp Patients?
Folliculitis inflames hair follicles. Bacteria multiply inside clogged pores. This infection jeopardizes graft survival and delays growth.
Folliculitis presents as red papules or pustules around grafts. It causes pain and itching. It disrupts the healing environment. Kolenda et al. (2020) conducted a retrospective study of 102 patients. They found that folliculitis occurred more frequently in patients with oily skin and poor postoperative hygiene. Zhou et al. reported an incidence of 12.1% in a large multicenter series. Infectious folliculitis usually stems from Staphylococcus aureus. Sterile folliculitis arises from inflammatory reactions to trapped hairs or sebum. Both types damage follicles. They cause premature shedding. They create scarring. Romera de Blas et al. (2024) note that delayed postoperative washing beyond 3 days significantly increases folliculitis risk in oily scalps.
What Is the Typical Healing Timeline for Oily Skin?
Scabs soften and fall off between day 8 and day 10. Redness fades by day 14. Patients must watch for folliculitis during days 3 to 14.
Day 1 to 3: The scalp feels greasy. Swelling peaks. Scabs form but remain soft. Day 4 to 7: Oil production increases. Patients start gentle washing. Day 8 to 10: Scabs detach naturally. The scalp looks clearer. Day 11 to 14: Redness diminishes. Most surface healing completes. Month 1 to 3: Shock loss occurs. New growth begins around month 4. Folliculitis, if it appears, usually surfaces during weeks 2 to 4.
Which Cleansing Protocols Protect Oily Scalp Patients?
Patients should wash daily with non-comedogenic medical shampoo. They must avoid vigorous scrubbing. They should keep pores clear without dislodging grafts.
Surgeons typically allow the first wash at 24 to 48 hours. Oily scalp patients should wash daily thereafter. They must use lukewarm water. They must pour shampoo gently. They should avoid rubbing. Non-comedogenic formulas prevent pore blockage. Salicylic acid or zinc pyrithione shampoos help regulate sebum. However, patients must avoid harsh sulfates. Harsh products strip too much oil. Stripping triggers even more rebound secretion. Patients should pat the scalp dry. They must never scratch. They must sleep on clean pillowcases. They should avoid touching the scalp with unwashed hands.
How Does a Dry Scalp Affect Hair Transplant Recovery?
Dry scalps heal slower. Scabs persist until day 10 to 12. Itching intensifies. Scratching risks graft loss. Intensive hydration prevents disaster.
Dry skin lacks the lipid layer that facilitates wound repair. It cannot retain moisture. It cannot flex easily. Every movement feels tight. The wound surface cracks. These cracks expose grafts to mechanical damage. They also create entry points for irritants. Patients with dry scalps face a longer, more uncomfortable recovery.
Why Does Lack of Sebum Impair Barrier Protection?
Sebum forms a protective lipid layer. Without it, moisture evaporates. The epidermis cracks. Pathogens penetrate more easily.
The stratum corneum relies on lipids to maintain its brick-and-mortar structure. Sebum fills gaps between corneocytes. It prevents transepidermal water loss. After surgery, this barrier function becomes critical. Grafts need a stable, moist environment. Dry scalps cannot provide it. Water escapes constantly. Cells dehydrate. Migration slows. Gandelman et al. (2000) showed that dehydration causes major damage to follicular unit grafts. Kim et al. (2002) confirmed that graft survival drops significantly after air exposure. These findings apply directly to dry scalp patients. Their wounds dry out faster. Their grafts face greater desiccation risk.
How Does Itching Increase Graft Dislodgement Risk?
Dry scalps itch intensely. Patients scratch unconsciously. Scratching pulls grafts from recipient sites. This mechanical disruption kills follicles.
Pruritus ranks among the most common postoperative complaints. Romera de Blas et al. (2024) attribute this itching to crust formation, scalp dryness, and epithelial regeneration. Dry scalps experience more pronounced itching than oily scalps. The sensation peaks at night when patients lose conscious control. They scratch in their sleep. Nails catch scabs. Scabs pull grafts with them. Even gentle rubbing dislodges newly anchored follicles. Each lost graft reduces final density. Patients must resist this urge. They should apply cold compresses. They should take oral antihistamines. They should keep nails short.
What Complications Arise from Persistent Scabbing?
Thick crusts block oxygen. They trap bacteria. They prolong inflammation. Grafts suffocate beneath persistent scabs.
Scabs consist of dried blood, serum, and dead cells. They protect wounds initially. However, they must fall off within 10 days. In dry scalps, they harden like cement. They adhere to hair shafts. They cover follicular openings. Oxygen cannot reach the graft. Bacteria multiply underneath. Inflammation continues. The graft enters a state of chronic hypoxia. If scabs remain beyond 14 days, surgeons worry about poor growth. They may recommend soaking with saline or emollient gels. They may gently lift stubborn crusts in the clinic. Prevention remains superior to treatment.
What Is the Expected Healing Duration for Dry Skin?
Scabs remain for 10 to 12 days. Redness lingers for 2 to 3 weeks. Full epithelial repair takes longer than oily skin.
Day 1 to 3: The scalp feels extremely tight. Swelling occurs. Hard crusts form quickly. Day 4 to 7: Itching peaks. Patients start washing. They must moisturize aggressively. Day 8 to 10: Scabs begin softening. They do not detach fully yet. Day 10 to 12: Scabs finally fall off. The scalp remains pink. Day 14 to 21: Redness persists. Surface healing completes. Month 1 to 3: Shock loss occurs. New growth often starts slightly later than in oily scalps. Full results still appear around month 12.
Which Hydration Strategies Support Dry Scalp Healing?
Patients should spray saline frequently. They should apply panthenol lotions. They must avoid alcohol-based products. They should use gentle, hydrating cleansers.
Surgeons recommend saline sprays every 2 to 3 hours during the first week. Saline hydrates without introducing irritants. Panthenol lotions soothe inflammation. Hyaluronic acid serums bind moisture. Patients should apply these products with clean hands. They must avoid products containing alcohol, fragrance, or menthol. These ingredients dry the scalp further. They trigger burning sensations. Washing should occur once daily with a mild, pH-balanced shampoo. Patients should rinse thoroughly. They should leave conditioner away from the graft area for the first two weeks.
How Do Other Skin Types Impact Surgical Outcomes?
Thick scalps challenge insertion but yield strong density. Thin scalps bleed easily and require gentle handling. Scarred scalps suffer reduced graft survival due to poor blood flow.
Each variant demands specific modifications. Surgeons cannot use identical punch sizes. They cannot apply uniform pressure. They must adapt their approach. Patients must understand their unique risks. This knowledge encourages compliance. It reduces anxiety.
Why Does Thick Scalp Tissue Create Surgical Resistance?
Dense dermis blocks needle advancement. Surgeons apply more force. This increases transection risk. However, thick tissue grips grafts securely once placed.
Thick scalps measure 4 to 6 millimeters in depth. The dermis contains tightly packed collagen bundles. Creating recipient sites requires sharper blades. The surgeon must press harder. This pressure risks cutting adjacent follicles. It also causes more postoperative discomfort. Swelling lasts longer. Numbness may persist for weeks. Despite these challenges, thick skin rewards patients. It holds grafts in perfect position. It provides robust blood supply. It produces dense, natural-looking results. Surgeons often prefer FUE with sapphire blades for thick scalps. These blades slice cleanly through dense tissue.
How Does Thin Scalp Increase Trauma Risk?
Minimal padding exposes vessels and follicles. Needles penetrate too deeply easily. Bleeding obscures the field. Grafts sit precariously.
Thin scalps measure less than 2 millimeters. The dermis sits directly atop the galea aponeurotica. Blood vessels run superficially. Any incision cuts multiple vessels. Bleeding floods the surgical field. The surgeon cannot see graft placement clearly. Grafts placed in shallow beds protrude. They dry out. They fall out. These patients need DHI or stick-and-place techniques. These methods minimize handling. They reduce trauma. Surgeons use 0.7-millimeter needles. They implant at shallower angles. They pack less densely to preserve vascularity.
Why Does Scarred Tissue Reduce Graft Survival?
Scars contain disorganized collagen and few blood vessels. Grafts receive inadequate oxygen and nutrients. Survival rates drop measurably.
Scar tissue replaces normal skin after injury. It lacks hair follicles. It lacks sebaceous glands. It lacks the rich capillary network of healthy scalp. Surgeons can transplant into scars. However, they must accept lower survival rates. Grafts placed in avascular tissue cannot establish anastomoses. They cannot draw nutrients. They slowly die. Preoperative vascular assessment helps. Surgeons may use fluorescein angiography. They may inject PRP to stimulate angiogenesis. They may perform test sessions before full transplantation. Patients with scarred scalps need longer healing periods. They need 3 to 4 weeks for epithelial closure. They need 6 to 12 months to judge true growth.
How Do Healing Outcomes Compare Across Different Skin Types?

Oily skin heals fastest but risks infection. Dry skin heals slowest but avoids oil-related pimples. Thick and thin skin fall in between. Scarred skin heals poorest.
Direct comparison clarifies expectations. It guides patient preparation. It justifies personalized protocols. The following table summarizes key differences.
|
Skin Type |
Healing Speed |
Scab Duration |
Major Risk |
Graft Anchor Strength |
|
Oily |
Moderate-fast |
8–10 days |
Folliculitis, infection |
High |
|
Dry |
Slow |
10–12 days |
Scabbing, itching, graft loss |
Moderate |
|
Thick |
Moderate |
Moderate |
Surgical difficulty |
Very high |
|
Thin |
Variable |
Short |
Trauma, bleeding |
Low |
|
Scarred |
Slow |
Long |
Poor vascularity |
Low |
Which Skin Type Heals Fastest After FUE?
Oily and thick skin types generally heal fastest. Their robust tissue and active sebum production accelerate epithelial closure.
Oily skin provides moisture and lipids. Thick skin provides cells and collagen. Together, they create an ideal healing environment. Scabs soften quickly. Redness fades promptly. Grafts anchor firmly. Patients with these skin types often return to normal social activities by day 10. They experience less anxiety. They require less intensive intervention. However, they must remain vigilant against folliculitis. Fast healing does not guarantee perfect healing.
How Do Graft Survival Factors Differ by Skin Type?
Skin elasticity, oxygenation, and inflammatory response vary by type. Thick oily skin offers the best survival environment. Scarred skin offers the worst.
Graft survival depends on three factors. First, the graft must avoid physical trauma. Second, the graft must receive adequate oxygen. Third, the graft must avoid prolonged inflammation. Thick, oily skin protects against trauma. It provides excellent oxygenation. It resolves inflammation quickly. Dry skin fails on moisture. Thin skin fails on trauma protection. Scarred skin fails on oxygenation. Surgeons must optimize the factors that each skin type lacks. They must supplement dry skin with hydration. They must protect thin skin with gentle technique. They must improve scarred skin with vascular stimulation.
Should Surgeons Adjust Technique Based on Skin Type?
Yes. Surgeons should select FUE or DHI based on scalp fragility. They should choose shaved or non-shaved approaches based on hygiene needs.
Technique selection changes outcomes. It affects healing speed. It affects complication rates. It affects patient comfort. One technique does not fit all. Customization separates expert clinics from standard practices.
When Does FUE Outperform DHI for Sensitive Scalps?
FUE suits tight or sensitive scalps because it allows precise extraction without strip removal. DHI suits fragile recipient skin because it minimizes handling.
FUE extracts grafts individually. It avoids the linear scar of FUT. It reduces tension on tight scalps. Surgeons control punch depth precisely. They avoid deep penetration. DHI implants grafts using a pen-like device. This device loads and places grafts in one motion. It reduces graft exposure to air. It reduces handling. It suits thin recipient skin because it causes less trauma than forceps insertion. However, DHI requires more skill. It takes longer. Surgeons must choose based on both donor and recipient characteristics.
Why Does Shaved vs. Non-Shaved Approach Matter?
Shaved approaches allow better cleansing on oily scalps. They improve access to dry scalps for hydration products. Non-shaved approaches hide existing hair but limit visibility.
Shaving the recipient area exposes all graft sites. Surgeons see placement clearly. Patients wash thoroughly. Oily scalps benefit enormously. Cleansers reach every pore. Dry scalps also benefit. Moisturizers penetrate evenly. Non-shaved or partially shaved approaches preserve existing hair. They hide grafts immediately. They suit patients who cannot shave for social reasons. However, they limit visibility. They make washing harder. They increase scab retention. They raise infection risk in oily patients. Surgeons must weigh cosmetic concealment against biological advantage.
How Should Post-Operative Care Vary by Skin Type?
Oily scalps need cleansing-focused protocols. Dry scalps need hydration-focused protocols. All patients need sterile conditions and gentle handling.
Personalization defines modern hair transplant aftercare. Clinics now recognize that product selection changes outcomes. Washing frequency changes outcomes. Moisture levels change outcomes. Patients must follow skin-specific instructions exactly.
What Does an Oily Scalp Aftercare Protocol Include?
Daily medical shampoo use. Non-comedogenic formulations. Frequent but gentle washing starting day 3. Strict hygiene.
Patients begin washing at 24 to 48 hours. They use a dermatological shampoo formulated for sensitive scalps. They apply it with circular movements. They use minimal pressure. They rinse thoroughly. They wash daily for the first two weeks. They avoid oily hair products. They avoid pomades or waxes. They keep the scalp cool. Heat increases sebum production. They sleep on clean, cotton pillowcases. They change pillowcases every two days. They avoid touching the scalp. These steps prevent folliculitis. They keep pores open. They support graft oxygenation.
What Does a Dry Scalp Aftercare Protocol Include?
Saline sprays every 2 hours. Panthenol or hyaluronic acid lotions. Alcohol-free products. Limited washing frequency but intense moisture.
Patients spray saline starting on day 1. They apply panthenol lotion twice daily. They use a gentle, hydrating shampoo every other day. They avoid hot water. Hot water strips lipids. They pat dry gently. They never rub. They run a humidifier in their bedroom. This adds ambient moisture. They drink 2 to 3 liters of water daily. Hydration starts from within. They avoid direct sun. Sunburn worsens dryness. They avoid saunas and steam rooms for one month. These protocols restore barrier function. They reduce itching. They prevent graft loss.
Which Universal Rules Apply to Every Patient?
Every patient must avoid scratching. Every patient must sleep with head elevated for 48 hours. Every patient must avoid direct sun and sweating for 14 days.
Scratching dislodges grafts. Elevation reduces swelling. Sun exposure damages new epithelium. Sweating introduces bacteria. All patients must avoid smoking. Nicotine constricts blood vessels. It starves grafts. All patients must avoid alcohol for one week. Alcohol dilates blood vessels. It increases bleeding. All patients must follow their surgeon’s washing schedule precisely. Consistency matters more than product choice. Patients who adhere to universal rules experience fewer complications regardless of skin type.
What Complications Link Directly to Skin Type?
Oily skin causes folliculitis. Dry skin causes excessive scabbing. Scarred skin causes delayed healing. Thin skin causes bleeding and trauma.
Complications frustrate patients. They delay results. They sometimes destroy grafts. Understanding the skin-type link helps patients spot problems early. It helps them seek timely intervention.
Folliculitis primarily strikes oily scalps. It appears as red bumps or white pustules. It causes pain and itching. It sometimes requires antibiotics. Excessive scabbing plagues dry scalps. Thick crusts cover grafts. They block oxygen. They require medical soaking. Delayed healing haunts scarred scalps. Wounds remain open for weeks. They need advanced dressings. They need growth factor therapy. Bleeding and trauma threaten thin scalps. Hematomas form. Grafts dislodge. Surgeons must manage these complications with skin-specific strategies. Kerure and Patwardhan (2018) document that most post-transplant complications relate directly to these biological variations.
How Does Skin Type Influence Long-Term Hair Growth?
Skin type affects redness duration, shock loss risk, and hair emergence timing. Oily skin may show faster emergence. Dry skin may show delayed growth. Final results appear at 12 months.
Long-term outcomes depend on how well the scalp healed initially. Oily scalps often resolve redness by week 2. Dry scalps may show pinkness for 4 to 6 weeks. This prolonged erythema signals ongoing inflammation. It sometimes delays the anagen phase. Shock loss affects native hairs adjacent to grafts. It occurs in 0.15% to 15% of patients. Romera de Blas et al. (2024) identify female sex and high implantation density as major risk factors. However, dry scalps with poor circulation may experience higher shock loss because native follicles lack resilience. Hair shaft emergence usually begins at month 3 or 4. Oily scalps sometimes show earlier breakthrough because sebum lubricates the follicular canal. Dry scalps may delay until month 5. By month 12, most patients see full results. Skin type influences the journey, not necessarily the destination.
What Future Innovations Will Personalize Hair Transplant Healing?
AI scalp diagnostics, biomarker testing, and regenerative therapies like PRP and exosomes will soon allow fully personalized healing protocols.
Technology transforms every medical field. Hair transplantation follows this trend. AI algorithms now analyze scalp images. They measure pore size. They quantify sebum output. They assess vascular patterns. These tools provide objective skin-type classification. They eliminate guesswork. Biomarker testing may soon predict healing speed. A simple swab could reveal a patient’s inflammatory profile. It could identify patients at high risk for folliculitis or delayed healing. Regenerative therapies add another layer. PRP injections deliver growth factors. They accelerate angiogenesis. They boost graft survival in scarred or dry scalps. Exosome therapy offers cell-free regeneration signals. These innovations will not replace surgery. They will enhance it. They will allow truly personalized protocols based on individual biology.
Why Is Preoperative Skin Assessment Essential for Success?
Preoperative skin assessment determines healing trajectory. It guides technique selection. It shapes aftercare. Personalized care based on skin type significantly improves graft survival and patient satisfaction.
Hair transplantation succeeds when biology and surgery align. Skin type represents a critical biological variable. It controls sebum levels. It controls hydration. It controls thickness and vascularity. These factors determine how wounds heal. They determine how grafts survive. They determine how hair grows. Surgeons must evaluate scalp skin before every procedure. They must document oiliness, dryness, thickness, sensitivity, and scarring. They must adjust their technique accordingly. They must prescribe tailored aftercare. Patients must understand their skin type. They must commit to the specific protocols that match their biology. When clinics and patients embrace this personalization, outcomes improve. Complications drop. Satisfaction rises. The future of hair restoration lies not in more grafts, but in better biological matching.
Frequently Asked Questions
Does Oily Scalp Reduce Hair Transplant Success?
No. Oily scalp does not reduce success if patients follow proper cleansing. The thickness of oily skin actually helps graft anchoring.
Oily scalps provide excellent graft support. They heal quickly. They resist dehydration. The primary risk involves folliculitis. Proper washing eliminates this threat. Patients who cleanse daily with medical shampoo achieve outstanding results. Their grafts often survive at higher rates than grafts in dry skin.
Is Dry Scalp Dangerous for Graft Survival?
Dry scalp poses risks if patients scratch or neglect hydration. Proper moisturizing eliminates most dangers.
Dry scalps challenge patients with itching and scabbing. However, they do not inherently kill grafts. Saline sprays, panthenol lotions, and gentle washing protect follicles. Patients who hydrate aggressively see normal growth timelines. They must resist scratching. They must follow their surgeon’s moisturizing schedule.
Which Skin Type Heals Faster After FUE?
Oily and thick skin types heal faster than dry or scarred types.
Oily skin softens scabs quickly. Thick skin provides abundant healing cells. Both types close wounds efficiently. Dry skin hardens crusts. Scarred skin lacks blood flow. These types require longer recovery periods. Individual genetics also play a role. However, oiliness and thickness generally predict faster surface healing.
Can Skin Type Be Treated Before Surgery?
Yes. Dermatologists can treat seborrheic dermatitis or xerosis weeks before surgery. This optimizes the scalp environment.
Preoperative optimization improves outcomes. Patients with seborrheic dermatitis can use ketoconazole shampoo. This reduces inflammation. It lowers bacterial load. Patients with xerosis can use emollient therapy. This restores barrier function. Surgeons should schedule consultations at least one month before surgery. This window allows skin conditioning.
How Long Does Healing Differ by Skin Type?
Oily scalps heal in 8 to 10 days. Dry scalps need 10 to 14 days. Scarred scalps may need 3 to 4 weeks for full epithelial closure.
These timelines describe surface healing. Complete remodeling continues for months. However, visible recovery varies significantly. Oily patients return to work by day 7. Dry patients may need 10 to 12 days. Scarred patients require extended monitoring. Surgeons must set realistic expectations based on preoperative assessment.
References
Bernstein, Robert M., and William R. Rassman. “In Support of Follicular Unit Transplantation.” Dermatologic Surgery, vol. 26, no. 2, 2000, pp. 160-162.
Gandelman, M., et al. “Light and Electron Microscopic Analysis of Controlled Injury to Follicular Unit Grafts.” Dermatologic Surgery, vol. 26, no. 1, 2000, pp. 25-31.
Kerure, A., and N. Patwardhan. “Complications in Hair Transplantation.” Journal of Cutaneous and Aesthetic Surgery, vol. 11, no. 4, 2018, pp. 182-189.
Khatib, M., et al. “Complications Following Hair Transplantation: A Systematic Literature Review and Meta-Analysis.” Aesthetic Plastic Surgery, vol. 49, 2025, pp. 6393-6405.
Kim, Jung Chul, et al. “The Effects of Dehydration, Preservation Temperature and Time on the Hair GraftsA hair graft refers to a small unit of hair-bearing skin taken from the donor area—typically the back or sides....” Annals of Dermatology, vol. 14, no. 3, 2002, pp. 149-152.
Kolenda, Dominika, et al. “Risk Factors and Prognosis of Folliculitis at Recipient Sites Following Hair Restoration Surgery.” Hair Transplant Forum International, vol. 30, no. 3, 2020, pp. 85-89.
Romera de Blas, Cristina, et al. “Complications in Follicular Unit Excision Hair Transplantation.” Facial Plastic Surgery, vol. 40, no. 2, 2024, pp. 234-244.