Does the Donor AreaThe Source of Restoration The donor area plays a critical role in hair transplantation, as it serves as the source... Play a Critical Role in Hair Transplant Success?
Yes. The donor area determines the entire outcome of your hair transplant. Surgeons extract hair follicles from this zone. They implant these follicles into thinning areas. The donor area sits at the back and sides of your scalp. Hair in this region resists dihydrotestosterone (DHT). This resistance makes donor hair permanent. FUE and DHI techniques both depend on this zone. Patients often misunderstand donor area hair regrow concepts. Some clinics promise full regrowth. Science proves otherwise. Extracted follicles do not return. Surrounding hair merely compensates visually. Understanding this reality helps you set proper expectations.
What Is the Donor Area in Hair TransplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by...?
The donor area is the permanent hair zone on your scalp. It spans from ear to ear across the lower back of your head. It also extends along the sides. Hair follicles here contain DHT-resistant genetics. These follicles survive indefinitely. Surgeons classify this region as the safe donor zone. They harvest grafts exclusively from this area. FUE extracts individual follicular units. DHI follows a similar extraction method. Both techniques remove complete follicular structures. The donor area provides the raw material for your transplant. Without adequate donor supply, surgeons cannot achieve full coverage. Density in this zone directly limits your restoration potential.
Why Does “Donor Area Hair Regrow” Confuse So Many Patients?
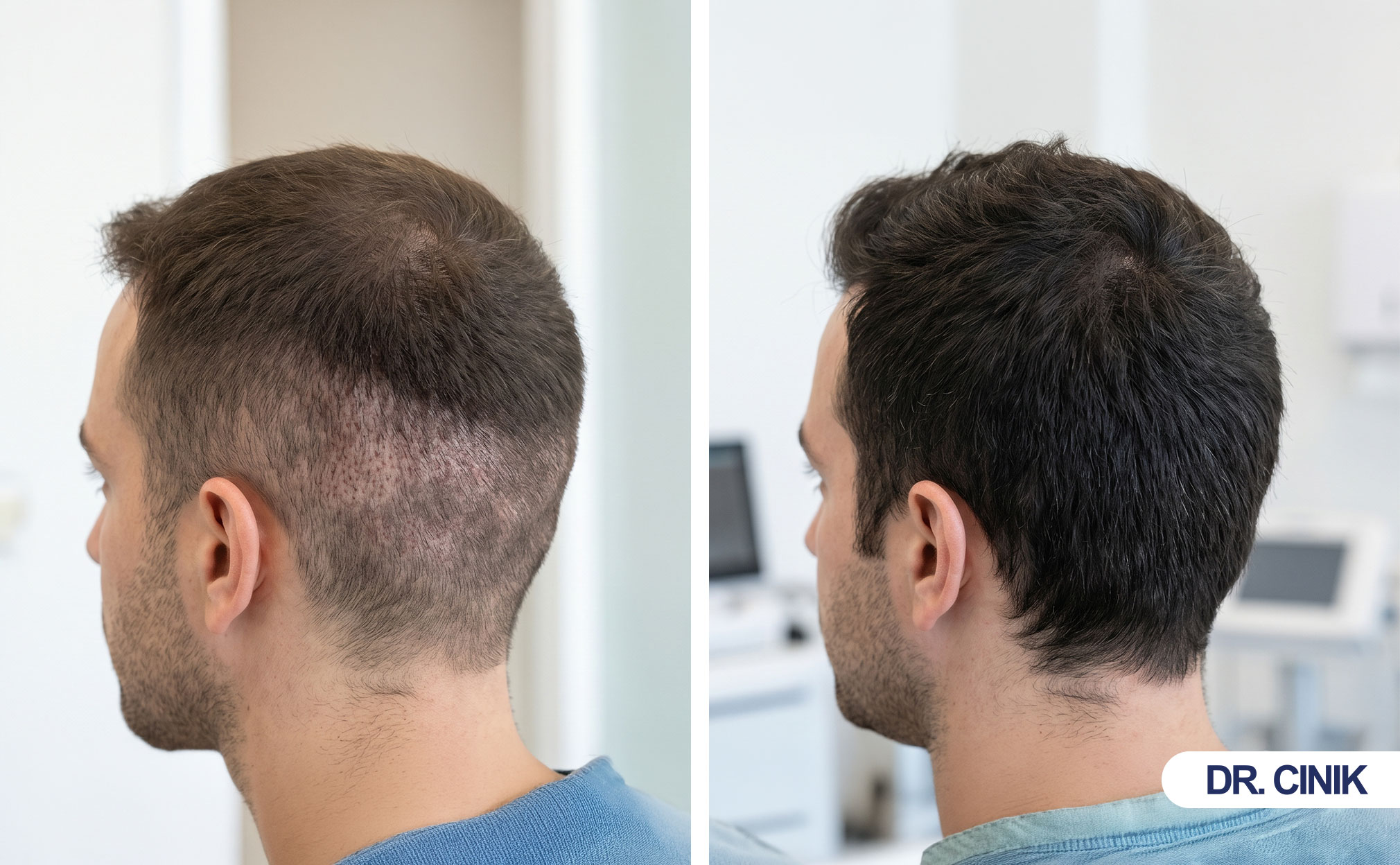
Marketing language creates this confusion. Some providers imply that hair returns naturally. Patients interpret “healing” as “regrowing.” Social media amplifies these myths. Before-and-after photos show improved density. Viewers assume extracted follicles regenerated. In reality, neighboring hairs grew longer. They covered extraction sites. The scalp healed. This healing creates an illusion of regrowth. Biology does not support true follicular regeneration. The dermal papilla leaves with the extracted graft. No structure remains to regenerate the same hair. Clear education prevents disappointment. You deserve accurate information before surgery.
What Does the Biology of Hair Follicles Reveal?
How Does a Hair FollicleA hair follicle is a small, tube-like structure embedded in the scalp that produces and grows individual strands of hair.... Actually Work?
A hair follicle is a mini-organ embedded in your skin. It contains multiple specialized components. The dermal papilla sits at the base. This structure feeds the growing hair. It contains blood vessels and signaling cells. Stem cells reside in the bulge region. These cells regenerate the lower follicle during each growth cycle. A complete follicular unit contains 1 to 4 hairs. It includes sebaceous glands and erector pili muscles. The anagen phase lasts 2 to 7 years. Hair grows actively during this time. The catagen phase follows. This transition period lasts 2 to 3 weeks. The follicle shrinks. The telogen phase is the resting stage. It lasts about 3 months. Then the cycle restarts. This biology governs every hair on your scalp (Unger and Shapiro 60).
Why Do Extracted Follicles Fail to Regenerate?
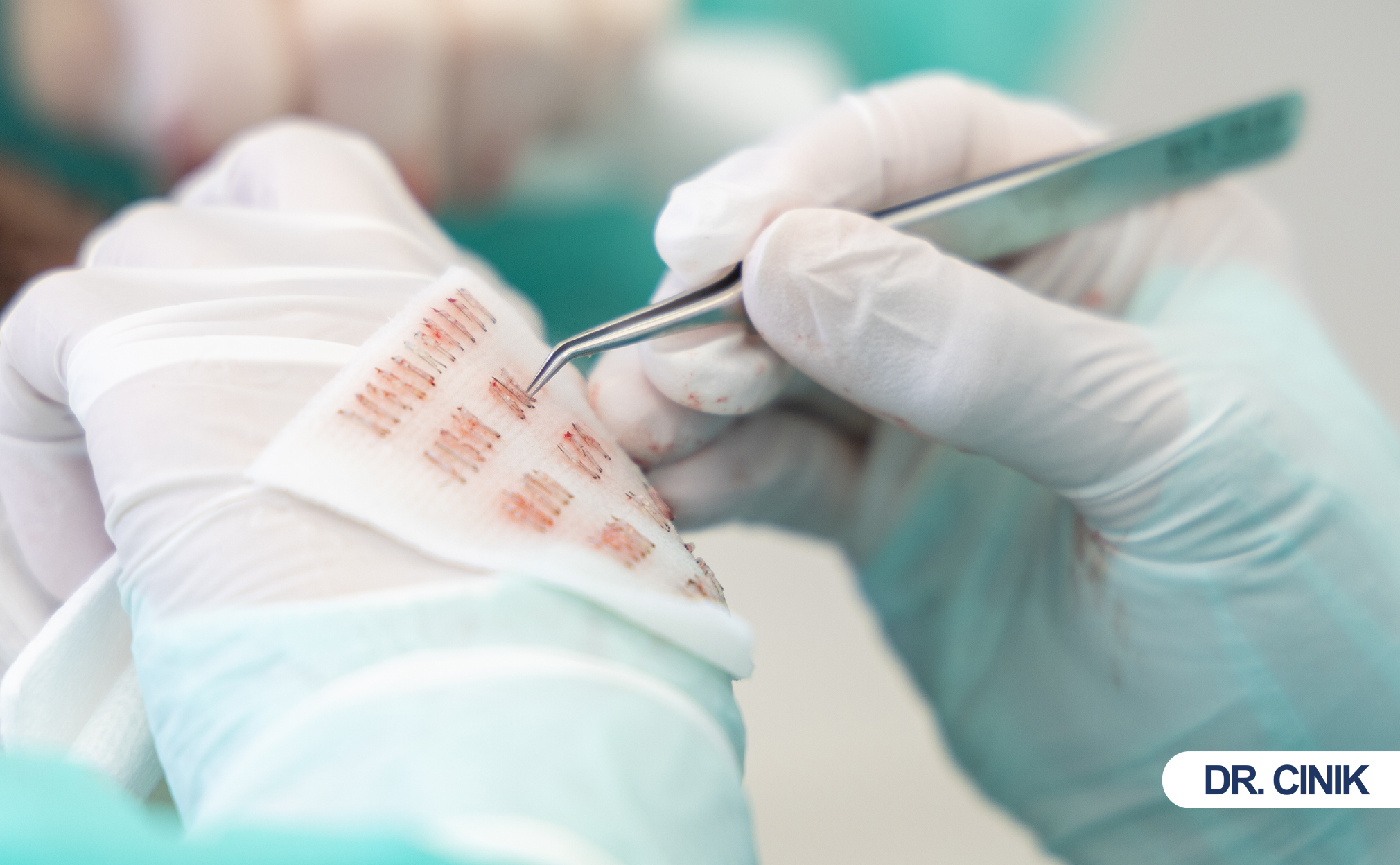
Surgeons remove the entire follicular unit during FUE. They use a circular punch tool. This tool cuts around the graft. They extract the complete structure including the dermal papilla. The dermal papilla is the engine of hair growth. Without it, no regeneration occurs. The follicle is an organ. Removing an organ ends its function permanently. Skin heals where the follicle once sat. New skin tissue fills the micro-wound. No new follicle forms. Scientists have not discovered a natural mechanism for follicular neogenesis in adult human scalps. Stem cells in surrounding skin cannot recreate a lost follicular unit. This fact is fundamental. It explains why donor area hair regrow claims are biologically impossible (Jimenez and Izeta 1247).
Does Donor Area Hair Regrow After Hair Transplant?
What Does Science Actually Say?
No. Extracted follicles do not grow back in the same spot. Researchers confirm this consensus across multiple studies. The follicle relocates permanently. It continues growing in the recipient area. The donor site loses that specific hair forever. This is not a controversial finding. It is established dermatological fact. Surgeons transplant living organs. They move them from one location to another. They do not copy or clone them. The donor area heals. It does not regenerate lost follicles. Every extracted graft represents a permanent reduction in donor supply (Bernstein and Rassman 57).
Why Do Some Sources Claim Donor Hair Grows Back?
Several factors create this false impression. First, surrounding hairs continue growing normally. These neighboring hairs increase in length. They partially cover extraction sites. Second, the scalp contracts slightly during healing. This contraction pulls nearby hairs closer together. Third, short remaining hair shafts may emerge from partially transected follicles. This happens when surgeons accidentally cut a follicle. A small hair may grow briefly. It lacks the full structure for sustained growth. It falls out quickly. Fourth, lighting and camera angles in photos hide thinning. Patients see improvement. They attribute it to regrowth. In reality, camouflage explains the visual change.
What Is the Real “Yes and No” Answer?
No removed follicle ever regenerates. Yes, the area can look better over time. These are separate facts. Follicle count drops permanently. Visual density may improve slightly. Surrounding follicles produce thicker hairs. They fill gaps optically. The scalp skin heals and flattens. Redness fades. Shadows disappear. These changes restore appearance. They do not restore follicle numbers. You must understand this distinction. Biological regrowth does not happen. Cosmetic recovery does happen. Both statements are true. They answer different questions.
What Is the Donor Area Healing Timeline?
What Happens in the First 10 Days?
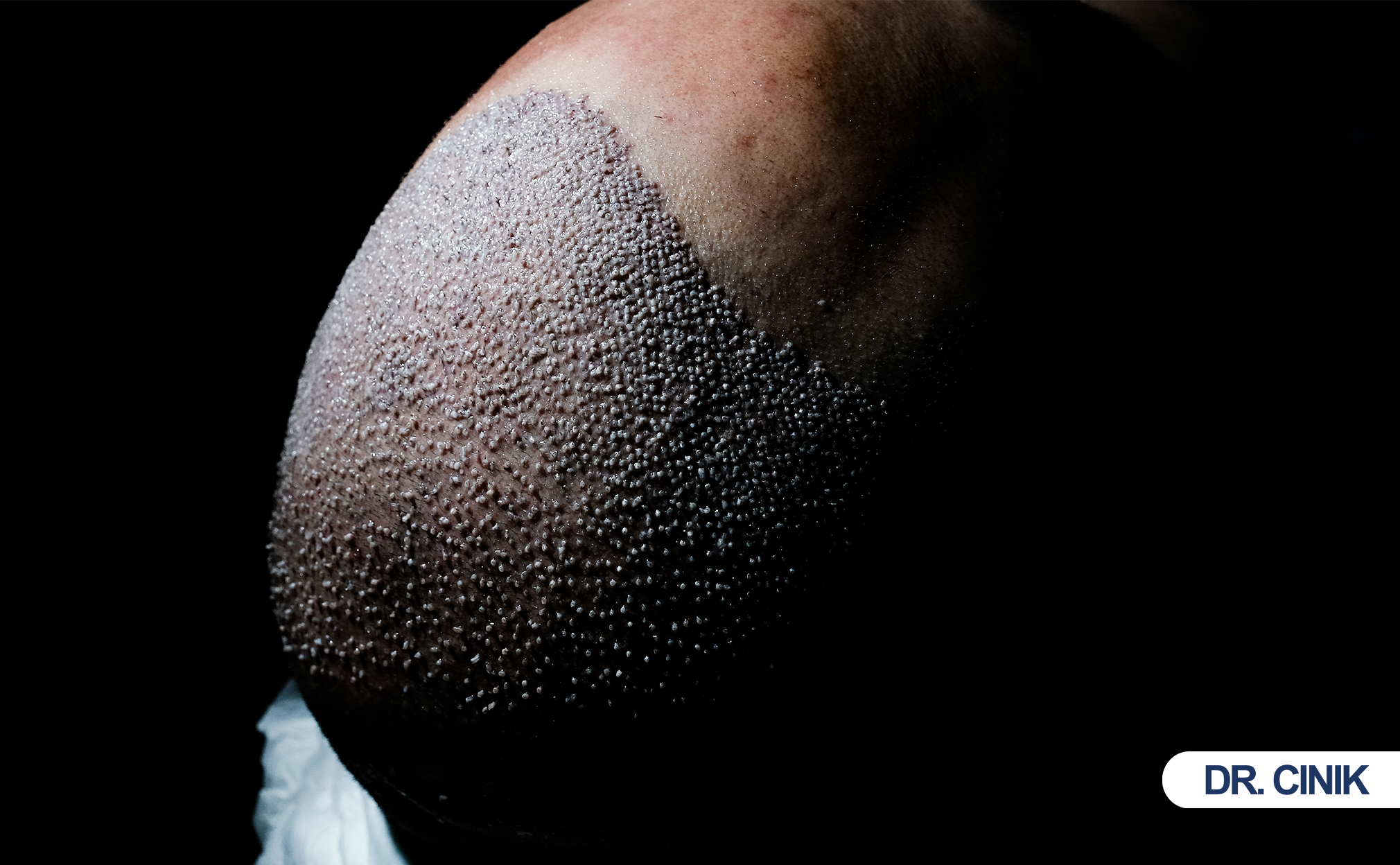
The scalp forms tiny scabs at each extraction site. These scabs protect the micro-wounds. Redness surrounds each point. This redness signals normal inflammation. Your immune system cleans the area. White blood cells remove debris. New skin cells migrate across the wounds. This process starts within 24 hours. The scabs begin falling off after 5 to 7 days. You must not pick them. Picking damages new tissue. It can cause infection. Most patients return to normal appearance within 10 days. The skin surface closes completely. Underneath, remodeling continues for months.
What Changes Occur Between 2 and 8 Weeks?
Hair around extraction sites grows longer. This growth provides natural coverage. The scalp loses all visible redness. Any shock loss in the donor area is rare. Unlike the recipient area, the donor zone rarely sheds hair from trauma. The follicles there are genetically strong. They resist shedding triggers. You can resume normal haircuts. The extraction sites become undetectable to casual observers. You might feel tiny bumps under the skin. These are normal healing nodules. They flatten over time. Massage helps break them down.
What Improvements Show at 3 to 6 Months?
Visual density increases significantly during this period. Neighboring hairs reach full length. They overlap extraction points. The skin completes most remodeling. CollagenA structural protein found in the skin and other connective tissues, which is responsible for skin firmness and elasticity.... reorganizes. The texture normalizes. You can wear short hairstyles confidently. Any slight irregularities in skin surface smooth out. The donor area looks largely uniform. However, microscopic analysis would still reveal reduced follicle density. The eye cannot detect this reduction easily. Photography from before surgery might show subtle differences. Overall, the zone achieves aesthetic recovery.
What Is the Final Result After 6 to 12 Months?
The donor area reaches stable appearance. All healing completes. The final density level sets in. You see a slight reduction compared to your pre-surgery state. This reduction is normal. It is the cost of transplantation. Good surgical planning makes this reduction invisible. Poor planning makes it obvious. The skin texture matches surrounding areas. No scars remain visible. You can shave your head if desired. Tiny dot marks may exist. These marks are usually invisible without magnification. The donor area functions normally. It simply contains fewer hair follicles.
What Factors Affect Donor Area Appearance?
How Does Surgical Technique Influence Results?
FUE extraction spacing matters enormously. Surgeons must distribute punches evenly. They avoid clustering extractions. Clustering creates visible patches. Punch size also affects outcomes. Smaller punches leave tinier wounds. They range from 0.7mm to 1.0mm. Larger punches remove more tissue. They create bigger gaps. Experienced surgeons select punch size based on hair characteristics. They match the tool to the follicle. Overharvesting destroys appearance. This happens when surgeons extract too many grafts from a small zone. They ignore safe density limits. The result looks moth-eaten. Proper technique preserves natural patterns. It maintains uniform distribution.
How Do Hair Characteristics Impact Visual Recovery?
Thick hair conceals extraction sites better than fine hair. Each thick hair covers more scalp surface. Curly hair provides additional coverage. It reflects light differently. It creates visual fullness. Straight, fine hair exposes the scalp more readily. Dark hair on light skin shows contrast. This contrast makes thinning visible. Light hair on light skin hides gaps better. Gray hair also camouflages well. Your natural density before surgery sets the baseline. Higher starting density allows more extraction. It leaves more remaining hairs. Lower starting density limits safe harvest numbers. Surgeons must adjust plans accordingly.
Why Does Surgeon Skill Matter So Much?
Strategic extraction patterns maintain natural aesthetics. Skilled surgeons study your hair growth direction. They follow natural part lines. They avoid extracting from obvious viewing angles. They stagger extraction points. This staggering mimics natural hair distribution. They preserve hairline framing at the nape. They maintain sideburn continuity. Poor surgeons extract randomly. They create visible tracks. They ignore aesthetic zones. Planning requires artistic vision. It requires mathematical precision. The best surgeons combine both. They treat the donor area as a finite resource. They budget every graft carefully.
How Does Post-Operative Care Help?
You must keep the donor area clean. Gentle washing removes crusts. It prevents infection. You should avoid direct sun exposure for weeks. UV radiation damages healing skin. It can darken scars. You must sleep carefully. Avoid rubbing the donor zone on pillows. Nutrition supports healing. Protein provides building blocks for skin repair. Vitamins A and C aid collagen formation. Zinc accelerates wound closure. You should avoid smoking. Nicotine constricts blood vessels. It delays healing. Alcohol causes dehydration. It impairs recovery. Follow every instruction precisely. Your behavior directly impacts final appearance.
What Is Donor Area Overharvesting?
Overharvesting means extracting too many grafts from the donor zone. Surgeons violate safe density thresholds. They prioritize graft numbers over donor health. This causes visible thinning. Patchy areas appear. The scalp looks moth-eaten. In severe cases, the skin shows through clearly. This damage is permanent. No treatment restores lost follicles. Overharvesting also destroys future options. You cannot undergo additional transplants. You have exhausted your supply. Young patients face special risks. Their hair loss may progress. They need donor reserves for future procedures. Aggressive harvesting in youth creates disaster later. Ethical surgeons refuse to overharvest. They explain realistic limits. They accept lower graft counts to preserve long-term donor health (Cole 89).
How Do FUE and DHI Compare in Donor Area Recovery?
What Do FUE and DHI Share?
Both techniques extract follicles from the donor area. Both use mechanical tools. Both remove complete follicular units. Both leave micro-wounds in the donor zone. Both follow the same biological rule. Neither technique causes follicular regeneration. The donor area loses grafts permanently in both cases. Healing timelines are nearly identical. Post-operative care requirements match closely. The fundamental donor area impact remains the same regardless of implantation method.
How Do FUE and DHI Differ?
DHI focuses on implantation technique. Surgeons use a Choi implanter pen. They insert grafts directly. This tool does not change the extraction process. FUE focuses on extraction methodology. Surgeons may use manual or motorized punches. The extraction determines donor area appearance. DHI does not improve donor healing. It improves graft placement precision. Some DHI practitioners use smaller punches. This choice affects donor wounds slightly. However, the difference is minimal. The key distinction lies in implantation, not extraction. Patients should not choose DHI expecting better donor recovery. They should choose it for recipient area benefits.
What Are the Common Myths and Facts?
|
Myth |
Scientific Reality |
|
Donor hair grows back fully after extraction. |
Only surrounding hair continues growing. Extracted follicles are gone permanently. |
|
The donor area fully restores to its original state. |
Density drops slightly forever. Good surgery hides this drop visually. |
|
The donor supply is unlimited. |
Donor hair is finite and non-renewable. Each person has a fixed budget. |
|
Special products can regenerate donor follicles. |
Biology limits regeneration. No lotion or serum creates new follicles. |
|
Shaving the donor area makes hair grow back thicker. |
Shaving does not alter follicle biology. It only blunts hair tips temporarily. |
|
Young patients can donate more because they have more hair. |
Young patients need to preserve donor hair for future loss progression. |
What Do Clinical Studies Reveal?
Research emphasizes donor management over regrowth fantasies. Studies focus on preserving density. They examine optimal extraction spacing. They analyze safe harvest numbers. One study tracked donor area changes after FUE. Researchers found permanent density reduction of 15% to 30% in extracted zones. They noted that visual appearance recovered well in most cases. Another study evaluated overharvested patients. It found irreversible thinning in 12% of cases with high graft numbers. Research consistently shows that surgeon planning determines aesthetic success. Studies also examine wound healing at extraction sites. They confirm that 0.8mm punches heal faster than 1.0mm punches. They document that motorized extraction causes more transection than manual methods in some comparisons. The scientific community agrees on one point. Donor area hair regrow is not a realistic goal. Density preservation is the achievable objective (Avram and Watkins 442; True and Dorin 115).
How Can You Maximize Donor Area Appearance?
What Are the Best Practices?
Choose your surgeon carefully. Verify their experience with donor area management. Ask to see donor area photos from past patients. Insist on conservative graft estimates. Demand explanations of their extraction plan. Follow every post-operative instruction without exception. Keep the scalp clean. Avoid trauma. Do not scratch. Sleep on your back initially. Protect the zone from sun. Maintain overall health. Control blood sugar. Manage blood pressure. These factors affect healing. Be patient. Full visual recovery takes months. Do not judge results at 2 weeks.
What Supportive Treatments Help?
PRP therapy accelerates healing. It delivers growth factors to the scalp. It reduces inflammation. It may improve surrounding hair quality. Microneedling stimulates collagen. It smooths skin texture. It breaks down minor fibrosis. Nutritional optimization supports tissue repair. Eat adequate protein. Consume omega-3 fatty acids. Take vitamin D if deficient. Consider zinc supplementation. Low-level laser therapy may improve scalp health. It increases blood flow. It reduces inflammation. These treatments support the environment. They do not regenerate follicles. They optimize what remains.
Frequently Asked Questions
Does Donor Hair Grow Back After FUE?
No. The extracted follicle does not return. Surrounding hairs grow longer. They cover the extraction point. The skin heals completely. This creates the appearance of recovery. The actual follicle count drops permanently. You cannot regenerate what the surgeon removed.
Can the Donor Area Look Exactly the Same as Before?
No. The area can look nearly similar. It cannot look identical. Microscopic density decreases. Visual density may appear unchanged. This depends on your starting hair characteristics. It depends on surgical technique. It depends on healing quality. Expect improvement, not perfection.
How Long Does Donor Area Recovery Take?
The skin surface heals in 7 to 10 days. Visual recovery takes 3 to 6 months. Final appearance stabilizes at 12 months. You can resume normal activities within 2 weeks. Full aesthetic blending requires patience. Everyone heals at different speeds.
Is Donor Hair an Unlimited Resource?
No. Your donor supply is finite. Surgeons estimate your total available grafts. This number typically ranges from 4,000 to 8,000. It varies by individual density. Once extracted, these grafts are gone forever. Plan carefully. Preserve donor hair for potential future needs.
Can Overharvesting Be Fixed?
No. Overharvesting causes permanent damage. Surgeons cannot implant hair back into the donor zone. They cannot regenerate lost follicles. Body hair transplantation offers limited coverage. Results are usually unsatisfactory for donor repair. Prevention is the only cure. Choose conservative surgery from the start.
Does the Donor Area Thin Naturally Over Time?
Yes. Natural aging reduces scalp density gradually. This process is separate from transplantation. It affects everyone. Transplantation accelerates density reduction in extracted zones. Combined with aging, this can become noticeable decades later. Good initial planning accounts for long-term changes.
What Is the Final Conclusion?
Donor area hair does not biologically regrow. Surgeons remove complete follicular organs during extraction. No natural mechanism replaces them. Visual recovery occurs through different means. Surrounding hairs grow longer. They cover extraction sites. The skin heals and remodels. These processes restore appearance. They do not restore follicle count. Success depends entirely on surgical planning. It depends on density management. It depends on patient aftercare. You must approach hair transplantation with realistic expectations. Understand that donor hair is a precious, finite resource. Protect it. Respect its limits. Work with qualified professionals. They will preserve your donor area while maximizing your aesthetic result. Science provides clear answers. Trust biology. Plan wisely. Your donor area determines your hair restoration future.
References
Avram, Marc R., and Rachel Watkins. “Donor Area Management in FUE Hair Transplantation.” Dermatologic Surgery, vol. 45, no. 3, 2019, pp. 438–445.
Bernstein, Robert M., and William R. Rassman. “Follicular Unit Extraction: Minimally Invasive Surgery for Hair Transplantation.” Dermatologic Surgery, vol. 28, no. 8, 2002, pp. 720–728.
Cole, John P. “Donor Area Depletion: The Risks of Overharvesting in FUE.” Hair Transplant Forum International, vol. 26, no. 3, 2016, pp. 87–91.
Jimenez, Francisco, and Ander Izeta. “Reflections on How Nature Engineers the Human Hair Follicle.” Journal of Investigative Dermatology, vol. 132, no. 5, 2012, pp. 1244–1248.
True, Robin H., and Robert Dorin. “Long-Term Donor Area Changes Following FUE Hair Transplantation.” Journal of Cosmetic Dermatology, vol. 17, no. 2, 2018, pp. 112–118.
Unger, Walter P., and Ronald Shapiro. Hair Transplantation. 5th ed., Marcel Dekker, 2011.