Hair transplant infection develops when bacteria, fungi, or other microbes invade surgical wounds created during follicular unit extraction or direct hair implantation. Poor sterilization, inadequate aftercare, and patient health conditions increase risk. Prevention requires strict surgical hygiene and disciplined postoperative care.
A hair transplant transforms thinning areas into fuller, natural-looking hairlines. Yet every surgical procedure creates entry points for microbes. Understanding infection risks protects both graft survival and overall health. Modern hair restoration maintains infection rates below one percent, but patients must recognize warning signs early (Rose, 2019).
Medical tourism draws thousands of international patients to Turkey annually for affordable, high-quality hair restoration. Istanbul clinics perform hundreds of procedures daily using advanced FUE and DHI techniques. Foreign patients face unique challenges including travel-related fatigue, unfamiliar climates, and limited follow-up access. These factors make infection awareness especially critical for medical tourists seeking hair transplant in Turkey or similar destinations.
What Is a Hair Transplant Infection?
A hair transplant infection occurs when pathogenic microorganisms colonize donor or recipient sites, triggering localized inflammation, pus formation, or systemic symptoms requiring medical intervention.
Clinicians define hair transplant infection as a clinically significant inflammatory response caused by microbial contamination of surgically created wounds. The condition ranges from mild folliculitis after hair transplant to severe abscess formation threatening graft viability. Surgeons classify infections based on timing, severity, and microbial cause (Unger, 2021).
Healthy immune systems typically prevent bacterial invasion during minor skin trauma. Hair transplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by..., however, creates thousands of micro-incisions simultaneously. Each incision breaches the skin barrier. This volume of wounds multiplies infection risk despite individual incisions remaining small. The scalp also hosts commensal bacteria including Staphylococcus aureus and Cutibacterium acnes, which exploit compromised skin defenses (Rose, 2019).
International patients must understand that “infected hair transplant” does not indicate surgical failure automatically. Infection represents a known, manageable complication. Early recognition and prompt treatment resolve most cases without permanent damage. Delayed intervention, however, risks graft loss, scarring, and rare systemic spread.
How Do Hair Transplant Procedures Create Infection Risk?

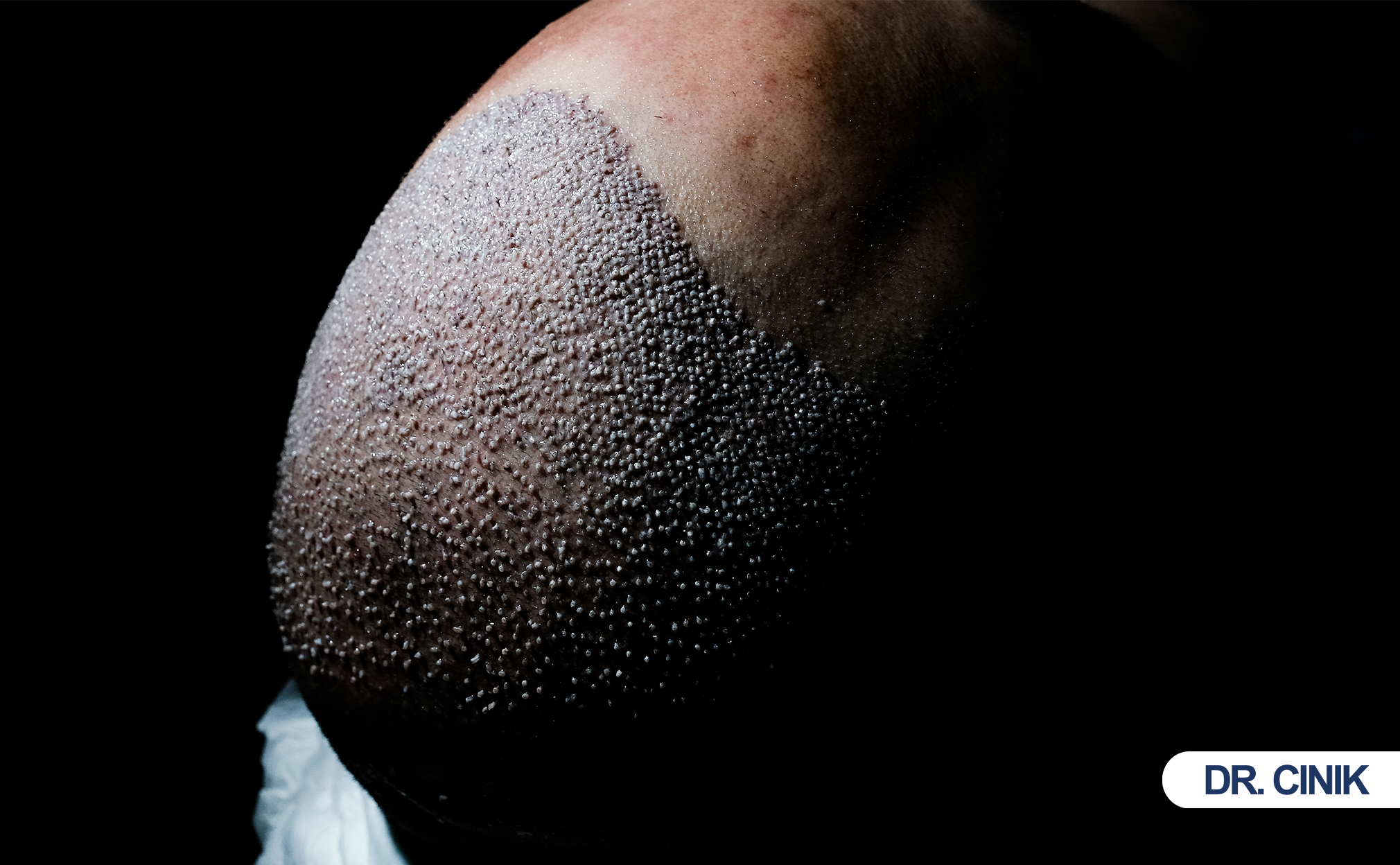
FUE and DHI techniques create thousands of micro-wounds in donor and recipient areas. These openings provide direct pathways for bacteria and fungi to enter deeper tissue layers.
What Happens During Follicular Unit Extraction?
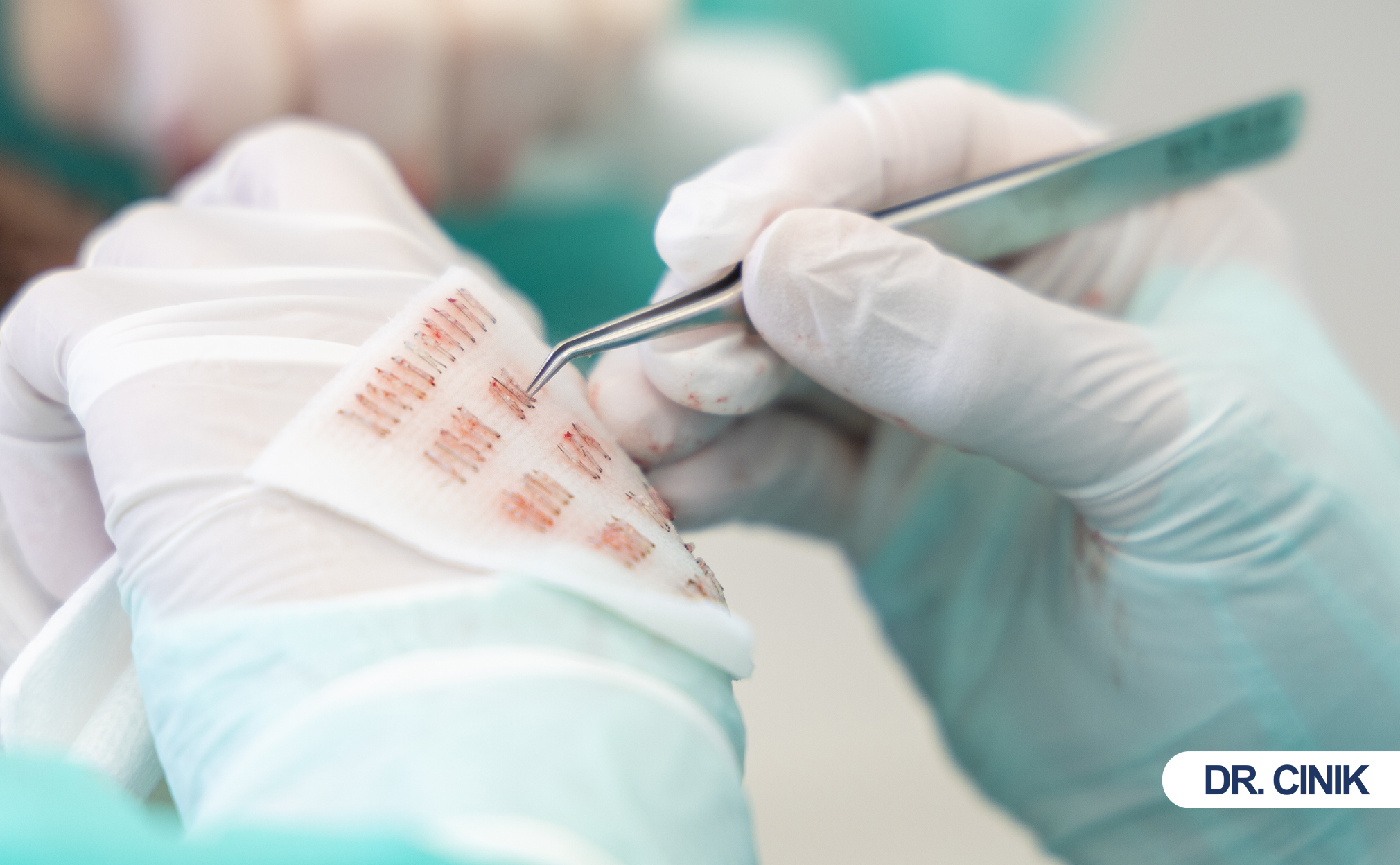
Surgeons extract individual follicular units from the donor zone using micro-punches, leaving tiny circular wounds that heal within days under normal conditions.
Follicular Unit Extraction (FUE) dominates modern hair restoration. Technicians use 0.8 to 1.0-millimeter punches to harvest grafts one by one. This method avoids linear scarring but generates hundreds to thousands of puncture wounds across the donor scalp. Each extraction site remains open briefly before clotting and epithelialization seal the breach (Unger, 2021).
The FUE infection risk remains low in sterile environments. However, non-sterile extraction tools, contaminated storage solutions, or improper graft handling introduce pathogens directly into dermal tissue. Once inside, bacteria multiply rapidly in the warm, nutrient-rich environment.
What Happens During Direct Hair Implantation?
DHI uses a specialized Choi implanter pen to insert grafts immediately after extraction, reducing outside-air exposure but requiring precise instrument sterilization.
Direct Hair Implantation (DHI) streamlines the process by implanting grafts without pre-made incisions. The implanter pen creates recipient sites and places follicles simultaneously. This technique minimizes graft-out-of-body time. Yet the pen tip contacts both scalp surface and deep tissue repeatedly. Without rigorous sterilization between loads, cross-contamination spreads microbes across multiple implantation sites (Kolenda, 2020).
Both techniques require creation of recipient sites. Whether using blades, needles, or implanters, surgeons breach the epidermis and dermis. These channels remain patent until clotting occurs, offering a window for microbial entry.
How Common Are Hair Transplant Infections?
Modern hair transplant procedures report infection rates below one percent, with most cases presenting as mild, localized folliculitis rather than severe complications.
Epidemiological data from accredited surgical centers consistently show infection incidence under one percent. A 2019 review analyzing over 10,000 hair restoration procedures found only 0.4 percent developed clinically significant infections requiring antibiotic therapy (Rose, 2019). Most post hair transplant complications involve temporary redness or minor pustules rather than deep tissue infection.
|
Procedure Type |
Infection Rate |
Typical Severity |
Resolution Time |
|
0.3–0.8% |
Mild folliculitis |
5–10 days |
|
|
0.2–0.6% |
Mild folliculitis |
5–10 days |
|
|
FUT (Strip) |
0.5–1.2% |
Localized abscess possible |
7–14 days |
Table 1: Comparative infection rates by technique. Data synthesized from multiple cohort studies (Rose, 2019; Unger, 2021).
Despite low overall rates, individual risk varies dramatically. Patients with diabetes, obesity, or immunosuppression face three to five times higher infection likelihood. Smoking doubles complication rates by reducing scalp blood flow and oxygen delivery (Kolenda, 2020).
Which Patient Factors Increase Infection Risk?
Diabetes, obesity, smoking, immunosuppression, poor nutrition, and systemic diseases significantly elevate postoperative infection risk by impairing wound healing and immune defense.
How Does Diabetes Affect Healing?
High blood glucose impairs white blood cell function and collagenA structural protein found in the skin and other connective tissues, which is responsible for skin firmness and elasticity.... synthesis, slowing wound closure and allowing bacterial colonization to progress unchecked.
Diabetic patients experience microvascular damage that reduces nutrient delivery to surgical wounds. Elevated glucose levels also compromise neutrophil chemotaxis and phagocytosis. These patients require extended antibiotic coverage and more frequent monitoring during hair transplant aftercare (Kolenda, 2020).
Why Does Smoking Create Problems?
Nicotine constricts blood vessels and reduces oxygen saturation in scalp tissue, starving healing sites of the resources needed to fight infection.
Smokers face documented higher rates of wound dehiscence and infection across all surgical specialties. In hair transplantation, compromised vascularization delays graft anchoring and epithelial migration. Surgeons strongly recommend smoking cessation at least two weeks before and four weeks after surgery (Unger, 2021).
What Role Does Immune Status Play?
HIV, cancer chemotherapy, and immunosuppressive medications blunt the body’s ability to recognize and destroy invading microbes at transplant sites.
Immunocompromised patients require individualized protocols. Some may need prophylactic antibiotics before surgery. Others might postpone elective transplantation until immune function recovers. Clinicians must evaluate CD4 counts, viral load, or neutrophil levels before scheduling procedures (Rose, 2019).
Which Surgical and Aftercare Factors Cause Infection?
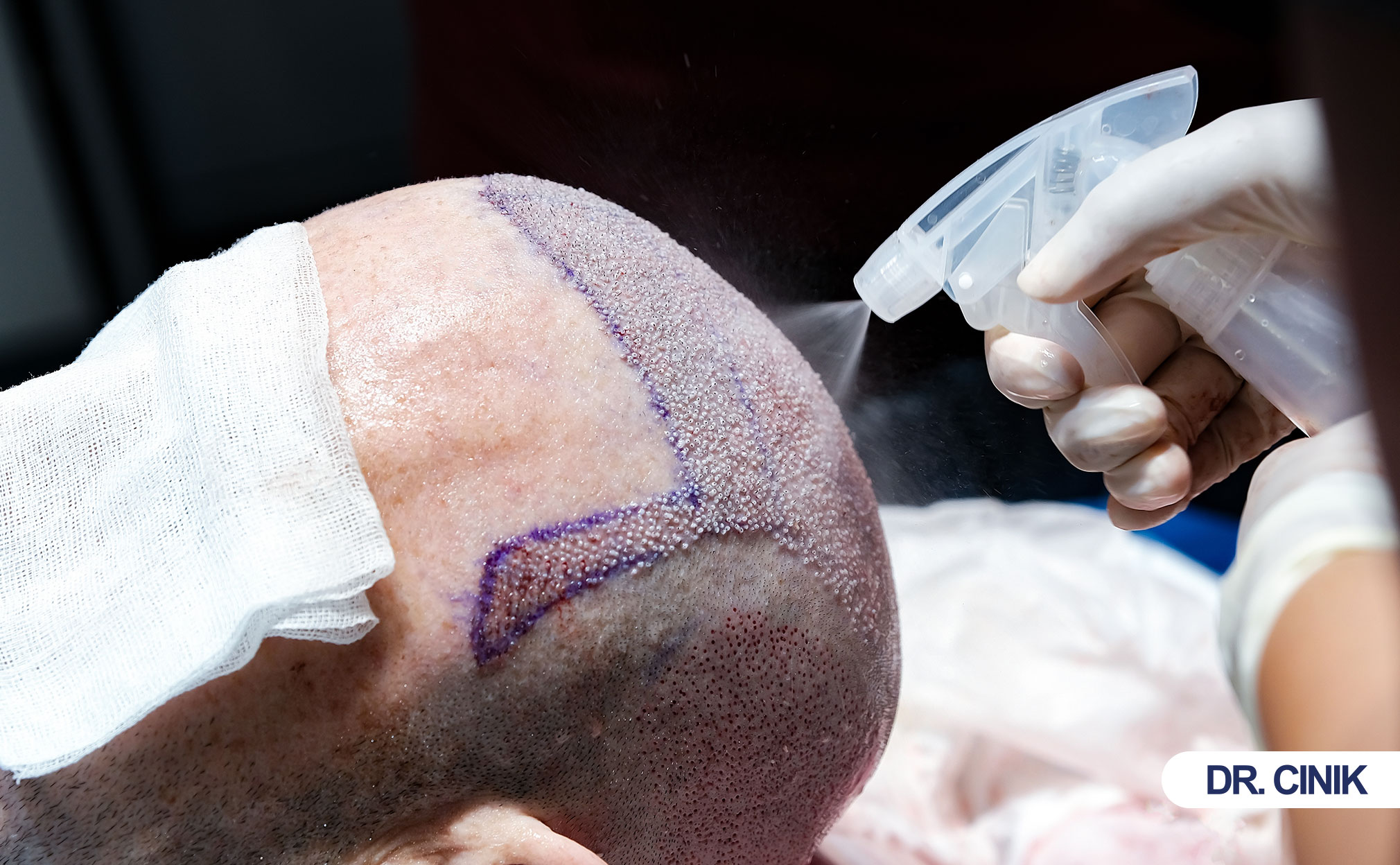
Poor instrument sterilization, excessive graft manipulation, improper wound cleaning, touching or scratching the scalp, and premature exposure to sweat or dirt drive most preventable infections.
How Do Sterilization Failures Occur?
Inadequate autoclave cycles, contaminated graft storage solutions, or non-sterile implanter pens introduce pathogens directly into viable tissue.
Accredited facilities use single-use punches, sterilized titanium tools, and laminar flow environments. Budget clinics sometimes reuse instruments without proper sterilization or perform procedures in non-medical settings. These shortcuts convert elective cosmetic surgery into high-risk interventions. Patients researching clinics should verify accreditation, surgeon credentials, and facility hygiene standards (Kolenda, 2020).
Why Does Aftercare Matter So Much?
Postoperative instructions protect wounds during the critical 72-hour period when clots stabilize and epithelialization begins.
The first three days after transplantation determine long-term infection risk. Patients must sleep with elevated heads to reduce swelling. They must avoid touching grafts, which transfers hand bacteria to vulnerable sites. They must follow prescribed washing protocols using gentle, clinic-approved techniques. Ignoring these rules causes hair plug infection in otherwise healthy patients (Unger, 2021).
|
Risk Factor Category |
Specific Threat |
Prevention Strategy |
|
Preoperative |
Uncontrolled diabetes |
Delay surgery until stable |
|
Preoperative |
Active smoking |
Quit minimum 2 weeks prior |
|
Intraoperative |
Non-sterile tools |
Choose accredited clinics |
|
Intraoperative |
Excessive graft handling |
Experienced surgical team |
|
Postoperative |
Touching grafts |
Keep hands away from scalp |
|
Postoperative |
Premature sweating |
Avoid exercise 10–14 days |
|
Postoperative |
Improper washing |
Follow clinic protocol exactly |
Table 2: Risk factors and prevention strategies across surgical phases.
What Are the Early Signs of Hair Transplant Infection?
Increasing redness after day three, spreading swelling, thick yellow or green discharge, foul odor, escalating pain, and warmth around graft sites indicate infection rather than normal healing.
How Does Normal Healing Look?
Mild redness, slight swelling, and minimal crusting peak around day two or three, then steadily improve without spreading or intensifying.
Normal postoperative inflammation remains confined to immediate transplant zones. Redness fades by day five. Swelling subsides within one week. Crusts form thin, dry layers that wash away gently during prescribed cleaning. Patients feel mild tightness or tenderness, not sharp or throbbing pain (Rose, 2019).
Which Symptoms Demand Immediate Attention?
Expanding redness, pus-filled pustules, fever above 38°C (100.4°F), chills, nausea, or headache signal progression from localized irritation to active infection.
Hair transplant infection symptoms follow a predictable timeline. Most infections declare themselves between day three and day seven. Some delayed presentations occur around day ten to fourteen, often linked to premature exercise, swimming, or scratching.
|
Symptom |
Normal Healing |
Possible Infection |
|
Redness |
Fades after 3 days |
Spreads or intensifies after day 3 |
|
Swelling |
Peaks day 2–3, resolves |
Worsens after day 3 or spreads to forehead/eyes |
|
Discharge |
Clear lymph fluid only |
Thick, colored, or foul-smelling pus |
|
Pain |
Mild, manageable |
Increasing, throbbing, or sharp |
|
Crusting |
Thin, dry, brown |
Thick, yellow-green, moist |
|
Temperature |
Normal |
Fever above 38°C |
Table 3: Distinguishing normal healing from infection symptoms.
Patients must photograph their scalp daily during the first two weeks. Comparing images helps identify subtle changes. Any deviation from expected healing warrants immediate clinic contact.
How Can Patients Tell Infection Apart from Other Complications?
Normal inflammation improves daily, folliculitis presents as scattered small pustules, allergic reactions cause widespread itching without pus, and shock loss affects native hair rather than graft sites.
What Is Postoperative Folliculitis?
Folliculitis after hair transplant manifests as small, superficial pustules around individual follicles, usually caused by Staphylococcus species and responding quickly to topical antibiotics.
Folliculitis differs from deep abscess infection. It produces multiple tiny whiteheads across transplant zones without significant spreading redness. The condition often resolves with warm compresses and topical mupirocin. Deep abscesses, conversely, form localized, painful, raised collections requiring drainage (Kolenda, 2020).
How Does Shock Loss Differ?
Shock loss causes temporary shedding of native hairs near transplant sites due to surgical trauma, presenting as diffuse thinning without redness, pus, or pain.
Patients sometimes mistake shock loss for infection-related graft failure. Shock loss occurs two to eight weeks post-surgery. Hairs fall out cleanly without inflammation. Infected graft loss, by contrast, happens earlier and accompanies obvious inflammatory signs.
What Happens If Doctors Ignore or Miss an Infection?
Untreated infections destroy grafts, create permanent scars, trigger fibrosis, and in rare cases spread to deeper tissues causing cellulitis or sepsis.
How Does Infection Destroy Grafts?
Inflammatory enzymes and bacterial toxins damage follicle bulbs and surrounding vascular supply, causing transplanted hairs to die and fall out permanently.
Each graft represents a significant investment of surgical skill and patient resources. Infection around graft sites triggers neutrophil infiltration and enzymatic tissue breakdown. If inflammation persists beyond the acute phase, fibroblasts produce scar tissue instead of normal dermal architecture. This fibrosis prevents future hair growth in affected areas (Unger, 2021).
Can Infection Become Life-Threatening?
Scalp infections rarely progress to sepsis in healthy patients, but immunocompromised individuals or those with neglected deep abscesses face genuine risk of systemic spread.
The scalp enjoys robust blood supply, which generally contains localized infection. However, facial vein drainage connects to intracranial structures through valveless communications. Although extremely rare, neglected scalp cellulitis can theoretically contribute to serious systemic complications. This possibility underscores the importance of never dismissing persistent symptoms (Rose, 2019).
|
Complication Type |
Mechanism |
Long-Term Impact |
|
Graft loss |
Bacterial toxins kill follicles |
Permanent bald patches |
|
Scarring |
Fibrosis replaces normal tissue |
Raised, shiny, or depressed scars |
|
Patchy regrowth |
Uneven graft survival |
Irregular density requiring revision |
|
Cellulitis |
Deep tissue spread |
Requires IV antibiotics, hospitalization |
|
Sepsis (rare) |
Bloodstream bacterial invasion |
Life-threatening systemic illness |
Table 4: Complications of untreated hair transplant infection.
How Do Doctors Diagnose Hair Transplant Infections?
Clinicians diagnose through visual inspection, pain assessment, and when necessary, wound culture, microscopic evaluation, or imaging for deep tissue involvement.
What Does Clinical Evaluation Involve?
Surgeons examine color, swelling patterns, discharge characteristics, odor, and pain levels, then compare findings against expected healing timelines.
Experienced hair restoration physicians recognize infection within seconds of examination. They assess whether redness extends beyond transplant margins. They check if swelling obscures graft visibility. They evaluate discharge color, consistency, and smell. Foul odor strongly suggests anaerobic bacterial involvement requiring specific antibiotic coverage (Kolenda, 2020).
When Do Doctors Order Lab Tests?
Wound culture guides antibiotic selection for severe or atypical infections, while blood tests help assess systemic involvement when patients show fever or malaise.
Culture and sensitivity testing identifies causative organisms and effective antibiotics. Staphylococcus aureus dominates most cases, but methicillin-resistant strains (MRSA) require different treatment. Fungal infections, though uncommon, need antifungal agents rather than antibacterial drugs. Microscopic examination of discharge differentiates bacterial colonies from simple inflammatory exudate (Unger, 2021).
Imaging studies such as ultrasound or MRI remain rare. Surgeons reserve these tools for suspected deep abscesses, osteomyelitis of underlying bone, or necrotizing soft tissue infections. Standard cases require no imaging.
What Treatments Resolve Hair Transplant Infections?
Oral antibiotics serve as first-line treatment, topical antiseptics support local control, abscesses require surgical drainage, and pain management plus wound care complete recovery.
Which Antibiotics Do Doctors Prescribe?
Cephalexin, clindamycin, or doxycycline typically cover common scalp pathogens, with MRSA-specific agents reserved for resistant cases.
Hair transplant infection treatment depends on severity and culture results. Mild folliculitis often responds to topical mupirocin or chlorhexidine washes. Moderate infections require seven to fourteen days of oral antibiotics. Severe cases with abscess formation need intravenous antibiotics and surgical intervention (Rose, 2019).
|
Infection Severity |
Treatment Approach |
Expected Resolution |
|
Mild folliculitis |
Topical antibiotic wash |
5–7 days |
|
Moderate localized infection |
Oral antibiotics + antiseptic care |
7–14 days |
|
Abscess formation |
Incision and drainage + oral antibiotics |
10–21 days |
|
Severe/deep tissue |
IV antibiotics + surgical debridement |
2–4 weeks |
Table 5: Treatment protocols by infection severity.
When Does Surgery Become Necessary?
Surgeons drain fluctuant abscesses and remove obviously necrotic grafts to prevent further bacterial load and allow healthy tissue to regenerate.
Abscess drainage provides immediate pain relief and removes purulent material that antibiotics cannot penetrate effectively. Graft removal in severe cases sacrifices non-viable tissue to save surrounding healthy follicles. These decisions require surgical judgment and occur only in advanced, neglected cases (Kolenda, 2020).
Supportive care includes acetaminophen or ibuprofen for pain, saline or antiseptic wound cleaning, and protective dressings if needed. Patients must continue strict aftercare protocols during treatment to prevent reinfection.
How Can Patients Prevent Hair Transplant Infection?
Prevention combines thorough clinic vetting, strict sterile technique during surgery, and disciplined adherence to postoperative washing, activity restrictions, and hygiene protocols.
What Should Patients Check Before Surgery?
Verify clinic accreditation, surgeon board certification, autoclave sterilization practices, and emergency antibiotic availability.
Selecting the right clinic prevents more infections than any postoperative measure. Accredited facilities maintain operating rooms with positive pressure, HEPA filtration, and regular microbiological testing. Surgeons should hold recognized certifications in hair restoration or plastic surgery. Staff should demonstrate clear protocols for instrument sterilization and graft handling (Unger, 2021).
International patients visiting Turkey or other medical tourism hubs must research beyond marketing photographs. They should request facility accreditation documents, surgeon CVs, and emergency contact protocols. Reputable clinics provide written aftercare instructions in the patient’s native language.
What Aftercare Rules Matter Most?
Avoid touching grafts, follow prescribed washing schedules, sleep with head elevated, avoid sweating for ten to fourteen days, and abstain from smoking and alcohol during recovery.
The first seventy-two hours determine infection risk more than any other period. Patients must resist touching grafts despite itching. They must wash according to clinic instructions, usually starting day two or three with gentle pouring rather than direct shower spray. They must avoid gyms, saunas, swimming pools, and dusty environments for specified periods (Rose, 2019).
|
Timeframe |
Key Action |
Infection Prevention Purpose |
|
Days 1–3 |
No touching grafts |
Prevents bacterial transfer from hands |
|
Days 2–5 |
Gentle saline or clinic wash |
Removes crusts and bacteria without dislodging grafts |
|
Days 1–10 |
Sleep elevated |
Reduces swelling and fluid accumulation |
|
Days 1–14 |
No strenuous exercise |
Prevents sweat-related contamination |
|
Days 1–14 |
No smoking or alcohol |
Maintains optimal blood flow and immune function |
|
Days 1–30 |
Avoid swimming/pools |
Eliminates exposure to chlorine and communal bacteria |
Table 6: Critical postoperative timeline for infection prevention.
What Is the Typical Prognosis After Infection?
Most infections resolve completely with early treatment, leaving no permanent damage. Delayed intervention may compromise cosmetic results but rarely threatens overall health.
Early-treated infections show dramatic improvement within forty-eight to seventy-two hours of antibiotic initiation. Redness recedes. Pain diminishes. Discharge dries up. Grafts survive normally. Patients complete their original hair growth timelines without modification (Kolenda, 2020).
Infections diagnosed after one to two weeks of progression may cause some graft loss. Surgeons can often replace lost grafts in subsequent sessions once infection fully clears. Severe scarring remains uncommon with modern treatment but possible in neglected cases.
Follow-up care ensures complete resolution. Patients should attend all scheduled postoperative appointments even if symptoms improve. Surgeons verify healing microscopically and adjust protocols if needed.
What Should Every Patient Know About Infection Warning Signs?
Patients must monitor for spreading redness, increasing pain, pus, fever, or any symptom worsening after day three, and contact their surgeon immediately rather than waiting.
How Do Patients Select Safe Clinics?
Choose facilities with transparent accreditation, experienced surgical teams, clear emergency protocols, and comprehensive written aftercare instructions.
Education starts before surgery. Patients should ask direct questions about infection rates, emergency antibiotic availability, and 24-hour contact access. Clinics that evade these questions or promise zero risk deserve skepticism. Every surgical procedure carries some infection potential. Honest clinics acknowledge this and demonstrate preparedness (Unger, 2021).
When Must Patients Seek Immediate Help?
Contact the clinic immediately for spreading redness after day three, any pus or foul odor, fever above 38°C, or pain not controlled by prescribed medication.
Delaying communication turns manageable folliculitis into graft-threatening abscesses. Most clinics provide WhatsApp, phone, or email support for international patients. Patients should not wait for scheduled appointments if symptoms concern them. Early photos sent to surgical teams enable rapid assessment and treatment initiation without requiring immediate travel.
What Future Innovations Will Reduce Infection Risk?
Researchers explore antimicrobial graft storage solutions, automated sterile extraction devices, improved prophylactic antibiotic protocols, and patient-specific risk stratification tools.
Current studies investigate adding dilute povidone-iodine or hypochlorous acid to graft holding solutions. These additives suppress bacterial growth without damaging follicle viability. Early data show promising reductions in culture-positive grafts (Rose, 2019).
Robotic and automated extraction systems minimize human handling errors. These devices maintain consistent sterilization and reduce graft manipulation time. As technology advances, FUE infection risk may drop even further below current benchmarks.
Prophylactic antibiotic research seeks to identify which patients benefit most from preventive medication. blanket antibiotic administration raises resistance concerns. Targeted prophylaxis based on individual risk factors offers better outcomes with less ecological impact (Kolenda, 2020).
What Is the Bottom Line for Patients Considering Hair Transplantation?
Hair transplant infection remains rare, preventable, and treatable. Success depends on choosing qualified providers, following aftercare precisely, and responding immediately to warning signs.
Hair restoration delivers life-changing cosmetic improvements for millions worldwide. The procedure maintains an excellent safety profile when performed in accredited facilities by trained professionals. Infected hair transplant cases represent avoidable exceptions rather than expected outcomes.
Patients bear responsibility for their role in prevention. They must research clinics thoroughly. They must disclose medical histories honestly. They must follow aftercare instructions without improvisation. They must communicate promptly if concerns arise.
Medical tourism patients visiting Turkey, Mexico, or Eastern Europe for cost savings can achieve outstanding results. However, distance complicates follow-up care. These patients should select clinics with robust international patient support systems. They should plan longer initial stays to allow early postoperative evaluation. They should arrange telemedicine follow-up before departing home.
Hair transplant aftercare is not optional. It is a medical extension of the surgical procedure itself. Patients who treat aftercare with the same seriousness as the surgery itself almost never experience significant infections.
References
Kolenda, Michał. “Infectious Complications in Hair Transplantation: Risk Factors, Prevention, and Management.” Journal of Cosmetic Dermatology, vol. 19, no. 4, 2020, pp. 892–898.
Rose, Paul T. “Hair Transplantation: Current Techniques and Complications.” Facial Plastic Surgery Clinics of North America, vol. 27, no. 2, 2019, pp. 205–214.
Unger, Robin H., and Walter P. Unger. “Complications and Adverse Events in Hair Restoration Surgery.” Dermatologic Surgery, vol. 47, no. 3, 2021, pp. 345–352.