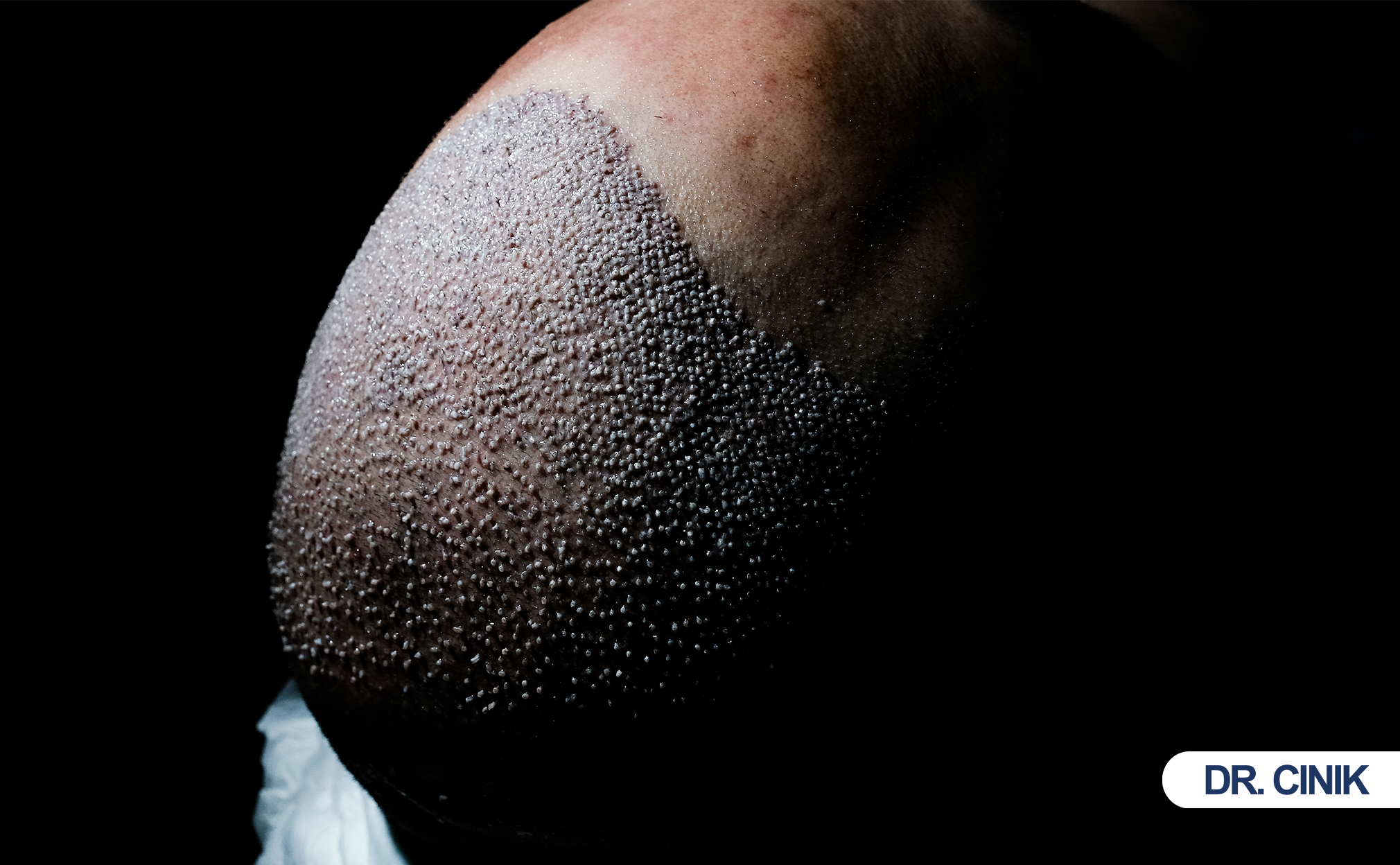
What Is Hair Transplant Pain and Why Does It Worry Patients?
Hair transplant pain is mild and temporary. Modern techniques make the procedure nearly painless for most patients.
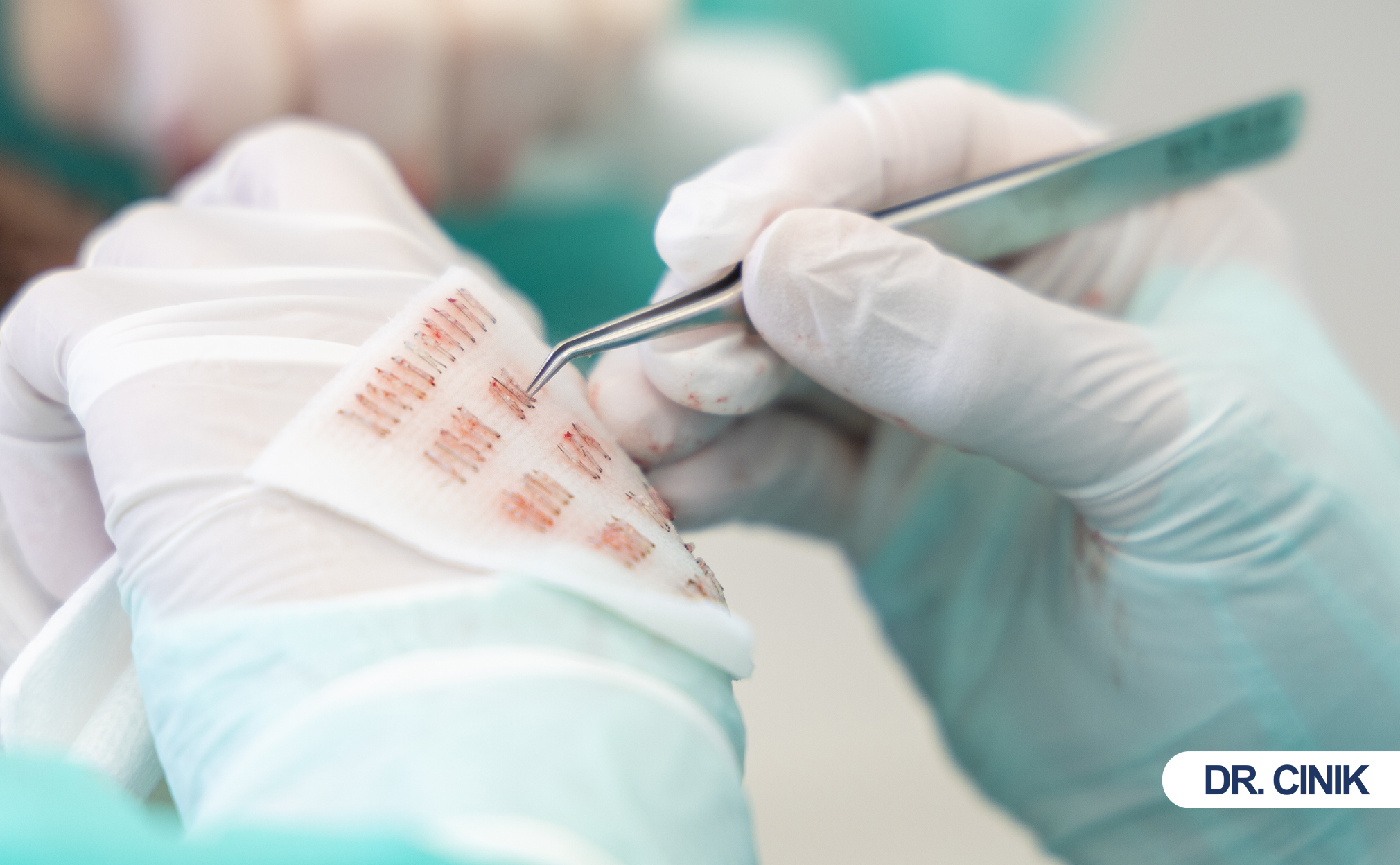
Hair transplantationHair transplantation is a surgical procedure that involves the extraction of hair follicles from a designated donor site, followed by... moves hair follicles from a donor areaThe Source of Restoration The donor area plays a critical role in hair transplantation, as it serves as the source... to a thinning or bald area. Surgeons perform this procedure using two main methods. Follicular Unit Extraction (FUE) removes individual follicles one by one. Follicular Unit Transplantation (FUT) removes a thin strip of scalp and then dissects it into grafts. Both methods require local anesthesiaEnsuring Comfort During Hair Transplants Sedation is used in hair transplantation to help patients remain calm and comfortable throughout the.... Both methods cause some degree of postoperative sensation. However, neither method causes severe or prolonged pain in the hands of a skilled surgeon.
Pain perception ranks as the top concern for patients considering hair restoration. Many prospective patients search online forums before their consultation. They read extreme stories. They watch videos. This research often amplifies fear. The clinical reality differs sharply from these fears. Scientific studies show that postoperative pain after hair transplantation is low. Most patients describe the experience as mild discomfort rather than sharp pain. Park et al. (2019) found that pain scores after FUT averaged only 2.03 out of 5 on the first postoperative day. FUE scores averaged even lower at 1.26 out of 5 (Park et al., 2019). These numbers represent mild discomfort, not agony.
The myth of extreme pain persists for several reasons. First, people confuse the brief sting of anesthesia with the entire procedure. Second, older techniques caused more discomfort than modern methods. Third, anxiety magnifies the expectation of pain. The clinical truth is simple. Modern hair transplantation is a minimally invasive outpatient procedure. Local anesthesia blocks all pain during surgery. Postoperative discomfort peaks within 48 hours. Then it fades rapidly.
What Does Pain Mean in a Surgical Context?
Pain is a subjective experience that involves nerve signals, brain interpretation, and personal perception.
What Is Nociception?
Nociception is the body’s detection of harmful stimuli through specialized nerve fibers.
Nociception forms the physical basis of pain. Special nerve endings called nociceptors detect injury, pressure, or temperature extremes. These nerves send signals through the spinal cord to the brain. The brain then interprets these signals as pain. However, nociception does not equal pain. The brain modulates these signals based on emotion, memory, and attention. Melzack and Wall (1965) revolutionized pain science with their gate control theory. They proved that the spinal cord contains a “gate” that can block or allow pain signals. This gate responds to psychological factors like anxiety and fear. When a patient feels anxious, the gate opens wider. The same physical stimulus then feels more painful. When a patient feels calm, the gate narrows. The same stimulus feels less painful. This discovery explains why two patients can undergo identical hair transplant procedures yet report very different pain levels (Melzack and Wall, 1965).
How Do Doctors Measure Pain in Hair Transplant Studies?
Doctors use the Visual Analog Scale and the Wong-Baker Faces Pain Scale to measure pain objectively.
Researchers need reliable tools to measure pain. The Visual Analog Scale (VAS) presents a straight line marked from 0 to 10. Patients mark their pain level on this line. Zero means no pain. Ten means the worst possible pain. The Numeric Rating Scale works similarly. Patients simply state a number from 0 to 10. The Wong-Baker Faces Pain Scale uses cartoon faces instead of numbers. This scale works well across language barriers. It also helps patients who struggle to translate feelings into numbers. Garra et al. (2013) validated that the Wong-Baker scale measures actual pain rather than fear or anxiety. This distinction matters because anxious patients might confuse fear with pain (Garra et al., 2013).
Clinical studies on hair transplantation rely heavily on these scales. However, subjective reporting has limitations. Pain thresholds vary genetically. Some patients rate mild pressure as a 2 out of 10. Others rate the same pressure as a 5 out of 10. Cultural factors also influence reporting. Some cultures encourage stoicism. Others encourage open expression of discomfort. Despite these limitations, standardized scales provide the best available method for comparing pain across techniques and time periods.
How Much Pain Do Patients Feel at Each Stage of a Hair Transplant?
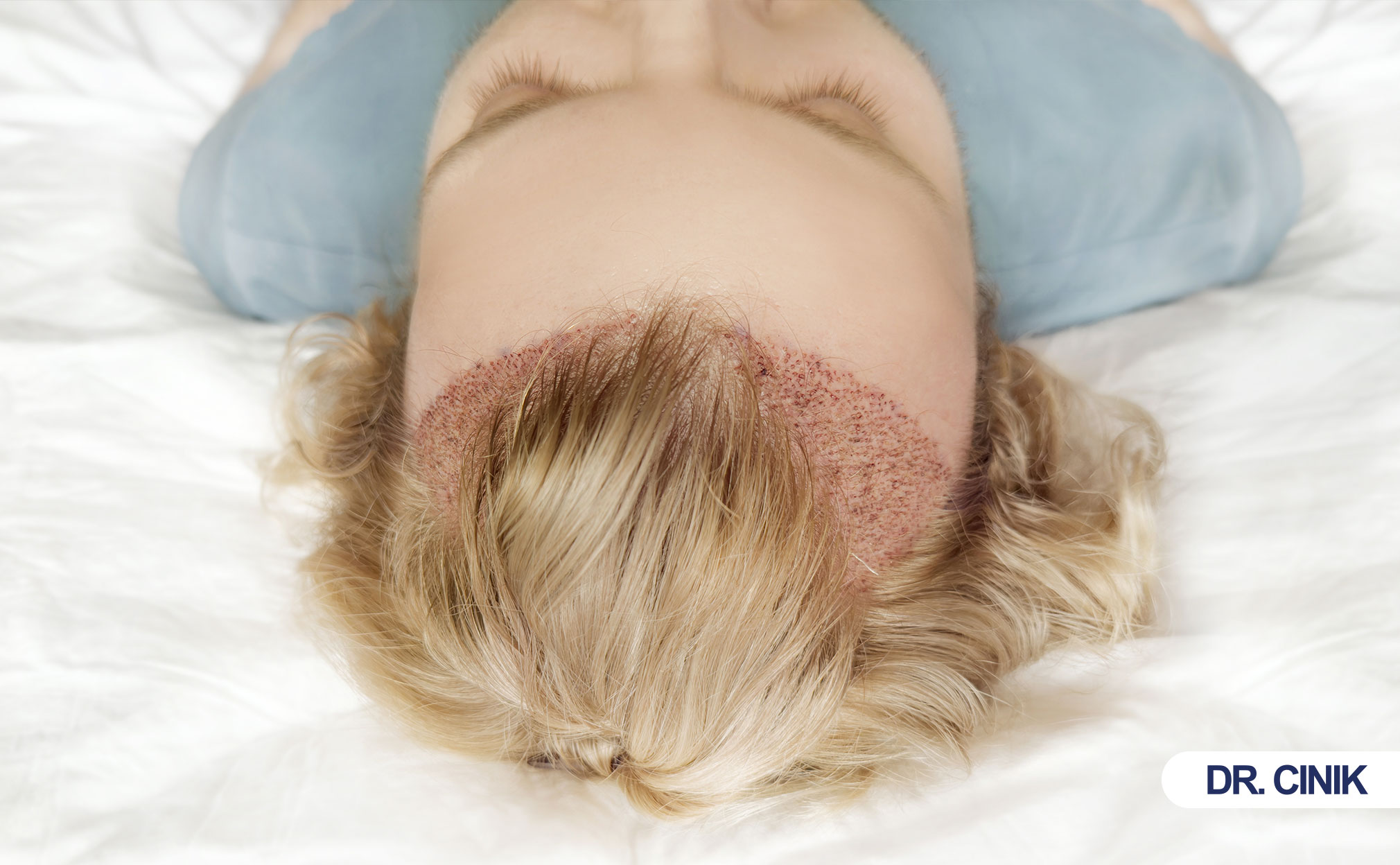
Most patients feel brief discomfort only during anesthesia. The rest of the procedure is painless.
How Painful Is the Anesthesia Injection?
The anesthesia injection causes brief discomfort that lasts 30 to 60 seconds. Patients rate it 2 to 6 out of 10.
The anesthesia phase produces the sharpest sensation of the entire hair transplant experience. Surgeons inject local anesthetic into the donor area and the recipient area. These injections create a brief sting. Patients describe it as a pinch, a rubber band snap, or a quick scratch. The sensation lasts only seconds. Numbness follows within minutes. Jimenez et al. (2021) note that surgeons can minimize this discomfort by using small-gauge needles, blunt microcannulas, and vibration devices. These tools distract nerve pathways and reduce the sting of infiltration (Jimenez et al., 2021).
The standard anesthetic solution contains lidocaine and epinephrine. Lidocaine blocks sodium channels in nerve fibers. This action stops pain signals from traveling to the brain. Epinephrine constricts blood vessels. This reduces bleeding and prolongs the anesthetic effect. Garcia Carmona and Garcia Tejeda (2025) explain that surgeons often use a ring block technique in the donor area. This technique anesthetizes the occipital nerves that run upward through the scalp. The ring block provides comprehensive numbness with fewer injections (Garcia Carmona and Garcia Tejeda, 2025).
Do Patients Feel Pain During Graft Extraction?
Patients feel pressure, vibration, and tugging. They do not feel sharp pain.
Once anesthesia takes full effect, the extraction phase is painless. FUE extraction uses a micro-punch tool. This tool rotates around each follicular unit. Patients feel a vibrating sensation. They feel gentle pressure on the scalp. They do not feel cutting or drilling. FUT extraction involves removing a strip of tissue. The surgeon cuts along the marked line. The patient feels pulling and pressure. Again, sharp pain does not occur under proper anesthesia.
Surgeons periodically add more anesthetic during long procedures. This practice is called a top-up. Top-ups prevent numbness from fading. They ensure continuous comfort throughout the session. True and Elliott (2002) compared microprocessor-controlled anesthesia delivery to conventional syringes. They found that computerized systems reduced injection discomfort. This improvement enhanced overall patient comfort during lengthy transplant sessions (True and Elliott, 2002).
Does the Implantation Phase Hurt?
Implantation is painless under proper anesthesia.
The implantation phase places grafts into tiny incisions in the recipient area. Surgeons use forceps or implanters. Each graft slides into a pre-made site or is placed directly. The patient remains fully numb in the recipient zone. Some patients report a mild awareness of manipulation. They feel the surgeon’s hands moving across the scalp. They might feel cool saline irrigation. None of these sensations qualify as pain.
Some advanced techniques use implanter pens. These pens load the graft and insert it in one motion. Implanters reduce handling of the graft. They also reduce trauma to the scalp tissue. Less tissue trauma translates to less postoperative discomfort. Jimenez et al. (2021) describe how precise recipient site creation with fine blades or needles minimizes scalp disruption. This precision supports faster healing and lower pain levels after surgery (Jimenez et al., 2021).
What Happens During the First 24 to 72 Hours After Surgery?
Mild soreness peaks within 48 hours. Then it declines rapidly.
As local anesthesia wears off, sensation returns to the scalp. Most patients experience mild soreness. Some feel tightness in the donor area. Others feel tenderness in the recipient zone. This discomfort is manageable. Over-the-counter medications like ibuprofen or acetaminophen control it effectively. Park et al. (2019) documented that 91.5% of FUT patients reported pain scores of 0 to 2 by postoperative day 3. FUE patients reached this low level even faster. Their pain scores dropped to minimal levels by day 2 (Park et al., 2019).
Peak discomfort occurs within the first 48 to 72 hours. During this window, some patients notice swelling. The swelling often appears in the forehead or around the eyes. It results from fluid migration and local inflammation. It is temporary. It resolves within 3 to 5 days. Sleeping with the head elevated at 30 to 45 degrees reduces swelling. Cold compresses applied for 10 to 15 minutes also help.
What Sensations Occur During Days 4 to 10?
Itching and minor discomfort replace pain as healing progresses.
By day 4, pain levels drop dramatically for most patients. Itching becomes the dominant sensation. This itching signals healing. It means the wounds are closing. It means new tissue is forming. Patients must resist scratching. Scratching can dislodge grafts. It can introduce infection. Surgeons recommend gentle saline spraying to relieve itch. Some patients notice crusting around grafts. These crusts are normal. They are part of the healing cascade. They fall off naturally between days 7 and 14.
FUT patients might feel tightness along the donor scar for slightly longer. The sutures or staples hold the wound edges together. This tension creates a pulling sensation. Surgeons remove sutures around day 10. After removal, tightness decreases significantly. FUE patients rarely experience prolonged tightness. Their donor sites are tiny puncture wounds. These wounds heal quickly.
Which Hair Transplant Technique Causes Less Pain?
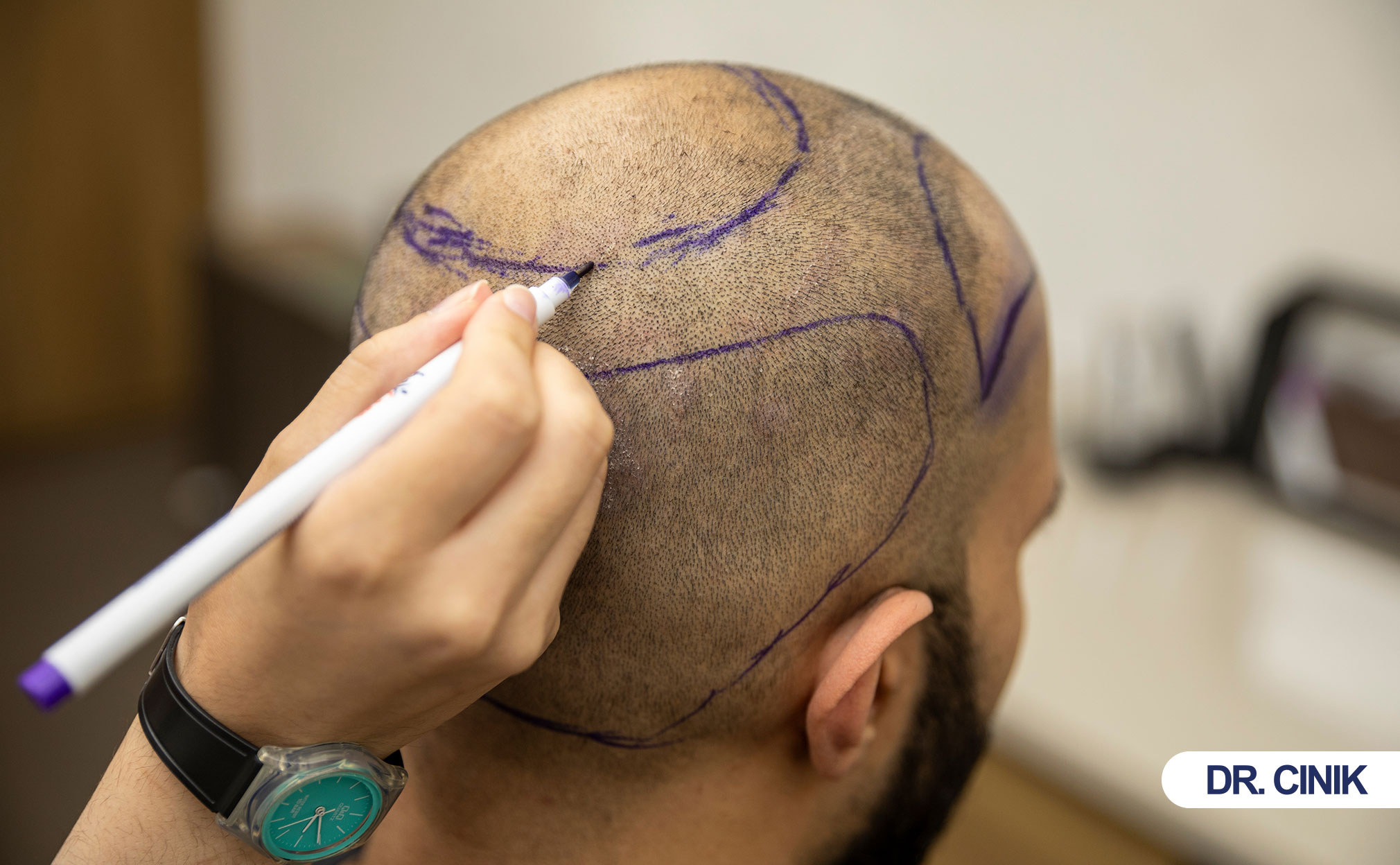
FUE causes significantly less postoperative pain than FUT.
How Much Pain Does FUE Cause?
FUE causes minimal postoperative pain. Most patients rate it 0 to 2 out of 10 after day 1.
FUE extracts individual follicular units using a punch 0.8 to 1.0 millimeters in diameter. Each extraction creates a tiny circular wound. These wounds heal independently. They do not require sutures. They do not create linear tension. Park et al. (2019) found that FUE patients averaged 1.26 out of 5 on the Wong-Baker scale on postoperative day 1. By day 2, this average dropped to 0.67. By day 3, it reached 0.31. These scores represent minimal discomfort (Park et al., 2019).
The lack of a linear incision explains the low pain profile. Nerve damage is localized to tiny points. The surrounding tissue remains intact. Patients can resume normal activities within a few days. They rarely need prescription pain medication. Over-the-counter anti-inflammatories provide sufficient relief.
Why Does FUT Cause More Discomfort?
FUT involves a linear incision and sutures. These create tension and more postoperative discomfort.
FUT removes a strip of scalp from the donor area. The surgeon then closes this wound with sutures or staples. This closure pulls the wound edges together. It creates tension across the incision line. This tension stimulates nociceptors. It produces a tight, sore sensation. Park et al. (2019) recorded FUT pain scores of 2.03 out of 5 on day 1. This score is significantly higher than the FUE score of 1.26. The difference remained significant through day 4 (Park et al., 2019).
FUT patients also face donor-site paresthesia. This condition involves numbness or tingling around the scar. It results from nerve transection during strip removal. Most cases resolve within months. However, the sensation can be unsettling. FUT also carries a higher risk of folliculitis. Park et al. (2019) noted that 19.2% of FUT patients developed scalp folliculitis. Only 4.1% of FUE patients developed this complication (Park et al., 2019). Folliculitis can cause localized pain and itching.
Despite these factors, FUT pain is still manageable. It is not excruciating. It is not disabling. By day 3, the average FUT pain score drops below 1.0. Most patients return to work within a week.
Do Advanced Techniques Like DHI and Sapphire FUE Reduce Pain?
Advanced techniques reduce tissue trauma. They improve patient comfort during and after the procedure.
Sapphire FUE uses blades made from synthetic sapphire instead of steel. These blades create finer, V-shaped incisions. The smaller incision size reduces tissue damage. It reduces bleeding. It promotes faster healing. Less tissue trauma directly correlates with less postoperative discomfort. DHI (Direct Hair Implantation) uses a specialized implanter pen. This pen allows the surgeon to create the recipient site and place the graft simultaneously. It eliminates the need for pre-made incisions. It reduces the time grafts spend outside the body. It also reduces scalp trauma.
Jimenez et al. (2021) emphasize that tool selection and surgical precision play major roles in patient comfort. Sharper blades create cleaner cuts. Cleaner cuts heal faster. Faster healing means less pain (Jimenez et al., 2021). While large-scale randomized trials comparing sapphire versus steel blades are limited, the mechanical principle is sound. Smaller wounds cause less pain than larger wounds.
Table 1: Pain Comparison by Technique
|
Technique |
Day 1 Pain Score |
Day 3 Pain Score |
Sutures Required |
Linear Scar |
|
FUE |
1.26/5 |
0.31/5 |
No |
No |
|
FUT |
2.03/5 |
0.91/5 |
Yes |
Yes |
|
Sapphire FUE |
~1.0/5 (estimated) |
~0.2/5 (estimated) |
No |
No |
Data for FUE and FUT from Park et al. (2019). Sapphire FUE estimates based on reduced tissue trauma principles described in Jimenez et al. (2021).
What Does the Day-by-Day Pain Timeline Look Like?
Pain peaks on day one. It nearly disappears by day seven.
What Happens in the First 24 Hours?
Numbness wears off. Mild pain begins. Medication controls it effectively.
The first 24 hours after surgery bring the most intense postoperative sensations. Local anesthesia fades within 6 to 8 hours. Patients then feel a dull ache in the donor area. The sensation resembles mild sunburn. It does not resemble sharp surgical pain. Some patients feel a throbbing pulse. This throbbing indicates healthy blood flow. It is a positive sign.
Surgeons recommend starting pain medication before numbness completely disappears. This proactive approach prevents pain from building. Aceclofenac and other NSAIDs are common choices. These drugs reduce inflammation and block pain signals. Patients should avoid aspirin. Aspirin increases bleeding risk.
How Do Days 2 and 3 Feel?
These days bring peak sensitivity and possible facial swelling.
Days 2 and 3 represent the peak recovery window. Some patients notice forehead or eyelid swelling. This swelling peaks around day 2. It looks dramatic. It feels puffy. It is harmless. It resolves without treatment. Sleeping with the head elevated minimizes this effect.
Pain scores continue to drop during this period. Park et al. (2019) showed that FUT pain fell from 2.03 on day 1 to 1.47 on day 2. FUE pain fell from 1.26 to 0.67. By day 3, only 0.5% of FUT patients reported extreme pain. The vast majority experienced mild or no discomfort (Park et al., 2019).
Itching intensifies during days 2 and 3. This itch signals the inflammatory phase of healing. Histamine release triggers the sensation. Patients must avoid scratching. Patting the area gently can provide relief.
What Changes Occur Between Days 4 and 7?
Pain drops rapidly. Itching becomes the main sensation.
By day 4, most patients transition out of the discomfort phase. Pain scores fall below 1.0 for both FUE and FUT patients. The scalp feels tight or slightly tender to touch. Routine activities resume. Patients return to office work. They avoid heavy exercise. They avoid direct sun exposure.
Crusts form around each graft. These crusts are dried blood and serum. They protect the wound. They should not be picked. Surgeons instruct patients to spray saline solution several times daily. This hydration softens crusts. Soft crusts fall off naturally between days 7 and 14.
How Does the Scalp Feel After One Week?
Most patients feel minimal to no pain after one week.
One week after surgery, pain is essentially gone. FUE patients often forget they had surgery. FUT patients might feel slight tightness along the scar. Suture removal typically occurs around day 10. After removal, even this tightness resolves. The recipient area might look pink. This redness is normal. It fades over the following weeks.
Some patients experience shock loss. This condition involves shedding of transplanted hairs around weeks 2 to 4. Shock loss causes no pain. It causes no bleeding. It alarms patients because it looks like failure. It is not failure. The follicles remain alive beneath the skin. New growth begins around month 3.
What Factors Influence Hair Transplant Pain Levels?
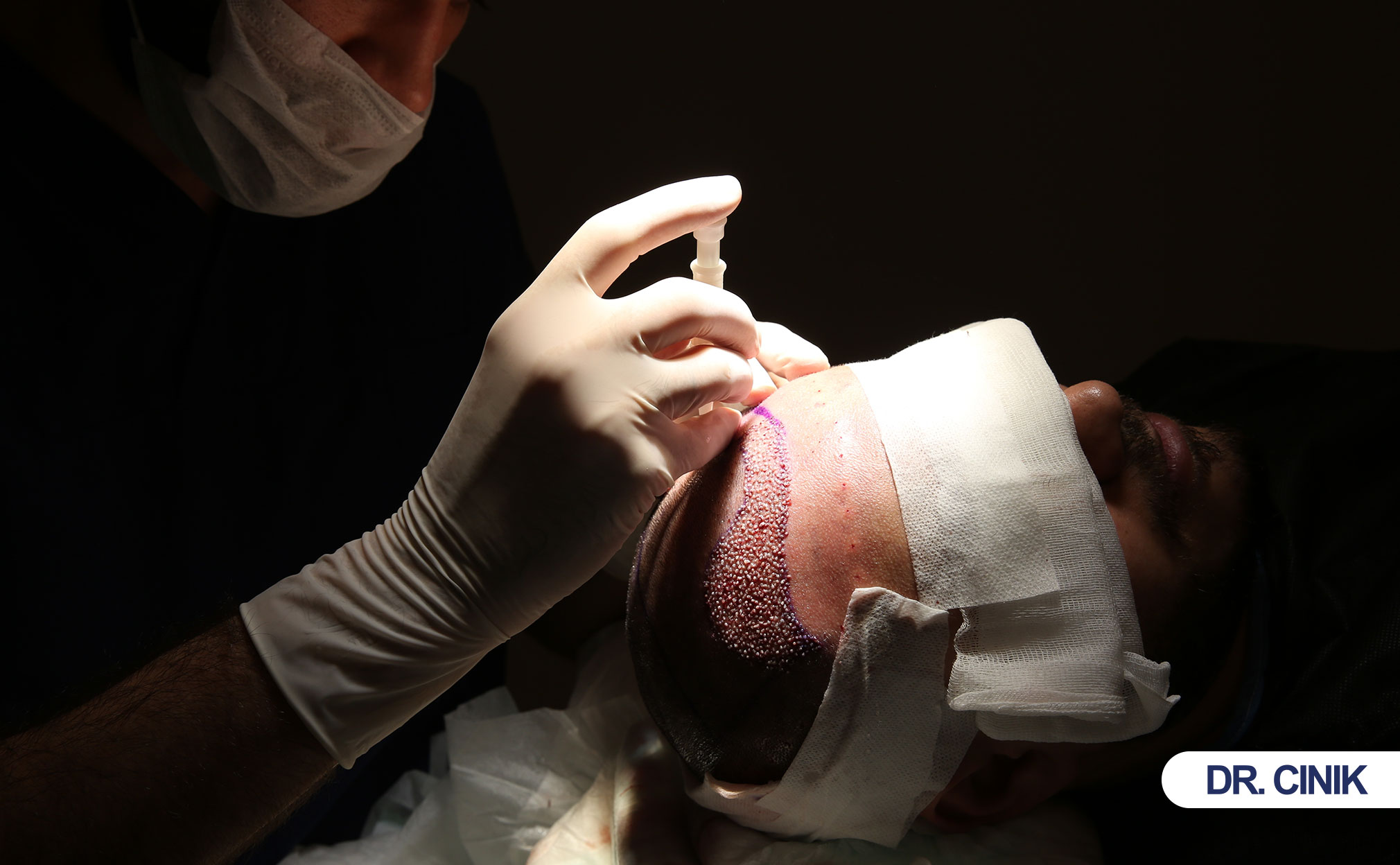
Individual pain threshold, surgeon skill, anesthesia type, graft count, and anxiety all affect pain.
Does Everyone Feel Pain the Same Way?
No. Genetics and psychology create wide variability in pain perception.
Pain thresholds differ dramatically between individuals. Some people inherit more sensitive nociceptors. Others inherit more efficient pain-modulating pathways in the brain. Psychological state also alters perception. A patient who expects severe pain will likely feel more pain. A patient who expects mild discomfort will likely feel less. Melzack and Wall (1965) demonstrated that cognitive factors directly modulate spinal gate mechanisms. Anxiety, fear, and catastrophizing open the gate. Distraction, relaxation, and positive expectation close it (Melzack and Wall, 1965).
Gender also plays a role. Park et al. (2019) found that female patients reported higher pain scores than male patients on every postoperative day. The difference was statistically significant. On day 1, women averaged 2.3 out of 5. Men averaged 1.8 out of 5. This gap persisted through day 7. Researchers attribute this difference to hormonal, psychological, and reporting factors (Park et al., 2019).
How Does Surgeon Skill Affect Pain?
Precise technique reduces tissue trauma. Less trauma means less postoperative discomfort.
Surgeon skill directly impacts pain levels. A skilled surgeon works quickly. Quick extraction reduces the time grafts sit outside the body. It also reduces the duration of tissue exposure. A skilled surgeon uses the correct punch size. An oversized punch creates unnecessary tissue damage. An undersized punch causes graft transection. Both errors increase inflammation. Both errors increase pain.
Fosko et al. (1998) showed that repetitive pinching of the skin during lidocaine infiltration reduces patient discomfort. This simple technique distracts nociceptors. It closes the pain gate. Experienced surgeons employ such tricks routinely. They also maintain consistent anesthesia depth. They monitor patient comfort throughout the procedure (Fosko et al., 1998).
Which Anesthesia Options Work Best?
Local anesthesia with lidocaine and epinephrine remains the gold standard.
Local anesthesia forms the foundation of pain-free hair transplantation. Lidocaine provides rapid onset. It blocks nerve conduction within 2 to 4 minutes. Its effect lasts 1 to 2 hours. Bupivacaine offers a slower onset but longer duration. It lasts 3 to 8 hours. Jimenez et al. (2021) recommend combining both agents. Surgeons inject lidocaine first. They add bupivacaine later. This combination provides immediate numbness and prolonged coverage (Jimenez et al., 2021).
Epinephrine accompanies both agents. It constricts blood vessels. It reduces bleeding. It slows the absorption of anesthetic. This slowing extends the numbness. It also reduces the risk of systemic toxicity. Garcia Carmona and Garcia Tejeda (2025) caution that surgeons must respect maximum dosage limits. Lidocaine with epinephrine should not exceed 7 milligrams per kilogram of body weight. Exceeding this limit risks toxicity (Garcia Carmona and Garcia Tejeda, 2025).
Some clinics offer conscious sedation. Patients take oral anxiolytics like diazepam or midazolam before surgery. These drugs reduce anxiety. They do not eliminate pain. They supplement local anesthesia. They do not replace it.
Does the Number of Grafts Matter?
Larger sessions may cause slightly more discomfort.
The total number of grafts affects procedure duration. A 2,000-graft session might last 4 hours. A 4,000-graft session might last 8 hours. Longer sessions require more anesthesia top-ups. They also create more extraction wounds. More wounds mean more cumulative inflammation. However, Park et al. (2019) found no statistically significant correlation between graft number and pain scores in FUT patients. Pain remained subjective and variable regardless of harvest size (Park et al., 2019).
Surgeons sometimes split mega-sessions into two days. This approach reduces fatigue. It reduces tissue trauma per day. It allows the scalp to recover overnight. Patients often report lower cumulative discomfort with this split approach.
Can Anxiety Make Pain Worse?
Yes. Anxiety amplifies pain perception. It increases postoperative discomfort.
Anxiety and pain share a well-documented relationship. Anxious patients report higher pain scores. They require more analgesic medication. They recover more slowly. The mechanism involves both psychological and physiological pathways. Anxiety increases cortisol levels. Cortisol sensitizes nociceptors. Anxiety also increases muscle tension. Tension in the neck and scalp amplifies the sensation of tightness after FUT.
Nusbaum (2004) reviewed techniques to reduce pain in hair transplantation. He emphasized that managing patient anxiety is as important as managing physical nociception. Preoperative education, a calm environment, and clear communication all reduce anxiety. Reduced anxiety translates directly to reduced pain (Nusbaum, 2004). Kehlet and Dahl (1993) introduced the concept of multimodal analgesia. They showed that combining multiple pain management strategies produces better outcomes than relying on drugs alone. This multimodal approach includes psychological support, physical comfort measures, and pharmacological agents (Kehlet and Dahl, 1993).
How Do Surgeons Manage Pain During Hair Transplantation?
Surgeons use local anesthesia, sedation, needle-free systems, and postoperative medications.
Why Is Local Anesthesia the Gold Standard?
Local anesthesia completely eliminates intraoperative pain. It allows patients to remain awake and comfortable.
Local anesthesia blocks all pain signals from the scalp. Patients stay awake. They can watch movies. They can listen to music. They can talk to the surgical team. This awake state eliminates the risks of general anesthesia. There is no breathing tube. There is no prolonged recovery room stay. The patient walks out of the clinic after the procedure.
Surgeons inject anesthetic in stages. They numb the donor area first. They begin extraction only after confirming complete numbness. They numb the recipient area next. They test sensitivity before making incisions. If a patient feels any sensation, the surgeon adds more anesthetic immediately.
When Do Surgeons Use Sedation?
Surgeons offer conscious sedation to anxious patients or those undergoing lengthy procedures.
Conscious sedation uses oral or intravenous medications. These drugs induce a state of deep relaxation. Patients remain conscious. They can follow instructions. They often remember little of the procedure. Diazepam, midazolam, and alprazolam are common choices. Jimenez et al. (2021) note that surgeons typically administer these agents 30 minutes before surgery. Sedation does not replace local anesthesia. It complements it (Jimenez et al., 2021).
Sedation carries its own risks. It requires monitoring of blood pressure and oxygen levels. Patients cannot drive after sedation. They need an escort. For these reasons, many surgeons reserve sedation for highly anxious patients or sessions exceeding 6 hours.
What Is Needle-Free Anesthesia?
Needle-free systems deliver anesthetic through high-pressure air. They reduce injection discomfort.
Needle-free jet injectors use pressurized gas to push lidocaine through the skin. No needle pierces the surface. This method eliminates needle phobia. It reduces the initial sting. However, Garcia Carmona and Garcia Tejeda (2025) note that needle-free systems have limitations. They may not deliver anesthetic as deeply as needles. Some patients require supplemental needle injections. The technology continues to improve. It offers a valuable option for needle-averse patients (Garcia Carmona and Garcia Tejeda, 2025).
Vibration devices offer another needle-free adjunct. These devices buzz against the skin near the injection site. The vibration stimulates large-diameter A-beta nerve fibers. These fibers activate the spinal gate mechanism. They block pain signals from smaller C-fibers. The result is a reduced perception of injection pain.
How Do Patients Control Pain After Surgery?
Patients use NSAIDs, cooling, head elevation, and proper aftercare.
Postoperative pain management starts before the patient leaves the clinic. Surgeons prescribe NSAIDs like aceclofenac or ibuprofen. Patients take these on a schedule for the first 3 days. Scheduled dosing prevents pain from building. It is more effective than waiting for pain to appear.
Cold compresses reduce inflammation. Patients apply them to the forehead or donor area for 10 to 15 minutes. They repeat this several times daily. They avoid placing ice directly on grafts. Direct contact can damage follicles.
Head elevation is crucial. Patients sleep with two pillows. This position reduces blood flow to the scalp. It minimizes swelling. It reduces throbbing sensations. It speeds up overall comfort.
Proper aftercare also prevents painful complications. Patients avoid touching grafts. They avoid strenuous exercise for one week. They avoid swimming pools and saunas. These precautions prevent infection. Infection is the most common cause of unexpected postoperative pain.
What Do Real Patient Pain Scores Show?
Clinical data shows anesthesia pain averages 2 to 6 out of 10. Postoperative pain averages 1 to 4 out of 10. It drops quickly.
What Are Average Pain Ratings for Each Phase?
Anesthesia rates 2 to 6 out of 10. The procedure rates 0 to 1 out of 10. Postoperative pain rates 2 to 4 out of 10.
Clinical studies provide clear numbers. The anesthesia injection averages 2.1 to 4.0 out of 10 on standard scales. Some patients rate it as high as 6.0. The procedure itself averages 0 to 1.5 out of 10. Most patients feel essentially nothing. Postoperative pain averages 2.0 to 3.4 out of 10 on day 1. By day 3, it falls below 1.0 for most patients.
Park et al. (2019) provide the most robust comparative data. Their study of 241 patients used the Wong-Baker Faces Pain Scale. FUT patients scored 2.03 on day 1. FUE patients scored 1.26. By day 7, FUT patients scored 0.21. FUE patients scored 0.13. These numbers confirm that hair transplant pain is mild and brief (Park et al., 2019).
Table 2: Average Pain Scores by Phase
|
Phase |
Average Pain Score |
Duration |
Management |
|
Anesthesia injection |
2–6/10 |
30–60 seconds |
Small needles, vibration, breathing techniques |
|
During procedure |
0–1/10 |
4–8 hours |
Local anesthesia top-ups |
|
Postoperative Day 1 (FUT) |
2.0/5 |
24 hours |
NSAIDs, elevation, cold compresses |
|
Postoperative Day 1 (FUE) |
1.3/5 |
24 hours |
NSAIDs, elevation, cold compresses |
|
Postoperative Day 3 |
<1.0/5 |
24 hours |
Usually none needed |
|
Postoperative Day 7 |
0.1–0.2/5 |
Minimal |
None needed |
Data adapted from Park et al. (2019).
Why Do Patient Stories Differ from Clinical Data?
Online forums amplify extreme experiences. They create anecdotal bias.
The internet contains thousands of hair transplant testimonials. Some patients claim the procedure was painless. Others describe it as torture. Both extremes are outliers. Clinical data captures the middle ground. It reflects hundreds of patients, not one.
People who have extreme experiences are more likely to post online. Satisfied patients with mild discomfort rarely write lengthy reviews. This reporting bias skews public perception. Prospective patients should rely on peer-reviewed studies rather than forum anecdotes. The science is clear. The typical experience involves brief injection discomfort, a painless procedure, and 2 to 3 days of mild soreness.
What Myths Exist About Hair Transplant Pain?
Many myths exaggerate the pain. Modern techniques make the procedure much more comfortable than people assume.
Is a Hair Transplant Extremely Painful?
No. Modern techniques keep pain levels low.
The myth of extreme pain dates back to older techniques. Decades ago, surgeons used larger punches. They used less refined anesthesia. They created more tissue trauma. Modern microsurgical tools have changed everything. Today’s punches measure less than 1 millimeter. Today’s anesthesia is precise and long-lasting. Today’s surgeons understand pain neuroscience. They apply gate control theory. They use multimodal analgesia. The result is a procedure that most patients tolerate with minimal discomfort.
Do Patients Feel Pain Throughout Surgery?
No. Effective anesthesia blocks all pain during the procedure.
Some prospective patients imagine lying on a table for hours while feeling every cut. This scenario does not happen. Local anesthesia creates complete numbness. If sensation returns, the surgeon adds more anesthetic immediately. Patients feel pressure. They feel vibration. They feel tugging. They do not feel pain. Many patients fall asleep during graft placement. Others watch movies. The experience is boring, not traumatic.
Is Recovery Very Painful?
No. Recovery discomfort is mild and short-lived.
Recovery from hair transplantation is not comparable to recovery from major surgery. There are no deep incisions through muscle. There is no bone involvement. The scalp has excellent blood supply. It heals quickly. Most patients describe recovery as a mild sunburn sensation. This sensation fades within 48 to 72 hours. It does not require strong opioids. It does not require bed rest.
How Does Hair Transplant Pain Compare to Other Procedures?
Hair transplant pain is comparable to dental work. It is less intense than many cosmetic surgeries.
Patients often ask for comparisons. They want context. They want to know if they can handle the experience. The most accurate comparison is dental work. The anesthesia injection in a hair transplant feels similar to a dental injection. The postoperative soreness feels similar to the ache after a filling. Both are manageable. Both fade quickly.
Tattoo pain exceeds hair transplant pain in most cases. Tattoo needles penetrate repeatedly over bony areas. They create continuous irritation. Hair transplants numb the area first. They then proceed painlessly. Minor dermatologic surgeries like mole removal cause similar injection pain. However, mole removal is faster. The postoperative discomfort is comparable.
Table 3: Pain Comparison Across Common Procedures
|
Procedure |
Peak Pain Score |
Duration of Discomfort |
Anesthesia Type |
|
Hair transplant (FUE) |
1–2/10 |
2–3 days |
Local |
|
Hair transplant (FUT) |
2–3/10 |
3–5 days |
Local |
|
Dental filling |
2–4/10 |
1–2 days |
Local |
|
Tooth extraction |
3–6/10 |
3–7 days |
Local |
|
Tattoo (bony area) |
4–7/10 |
During procedure only |
None |
|
Mole removal |
1–3/10 |
2–3 days |
Local |
When Should Pain Signal a Complication?
Severe or increasing pain after day 3 may indicate infection or nerve irritation.
Most postoperative pain follows a predictable downward trend. It peaks early. It improves daily. Pain that worsens after day 3 is abnormal. It requires medical attention. Possible causes include infection, excessive swelling, or nerve irritation.
Infection presents with redness, warmth, and pus. The scalp feels hot. Pain throbs intensely. Fever may develop. Prompt antibiotic treatment resolves the issue. Excessive swelling can compress nerves. This compression causes burning or shooting pain. It requires evaluation. Nerve irritation after FUT can cause persistent paresthesia. Most cases resolve spontaneously. Some require medication like methylcobalamin.
Patients should contact their surgeon if they experience any of the following: pain that increases after day 3, severe throbbing that does not respond to medication, spreading redness, fever above 38 degrees Celsius, or yellow discharge from the donor or recipient area.
Why Is Hair Transplant Pain Minimal Today?
Advances in microsurgical tools, anesthesia protocols, and patient-centered planning have revolutionized comfort.
Three major advances have transformed the hair transplant experience. First, microsurgical tools have shrunk. Punches now measure 0.8 to 1.0 millimeters. Blades are ultra-sharp. These tools create minimal tissue disruption. Second, anesthesia protocols have improved. Surgeons use ring blocks instead of random infiltration. They combine lidocaine and bupivacaine. They add epinephrine for prolonged effect. They use vibration and pinching to reduce injection discomfort. Third, patient-centered planning addresses anxiety. Clinics offer music, entertainment, and comfortable positioning. They explain each step. They set realistic expectations.
Jimenez et al. (2021) summarize these advances in their comprehensive review of hair transplantation technique. They note that modern surgical planning prioritizes patient comfort alongside graft survival. The two goals are not separate. They are intertwined. A comfortable patient moves less. A still patient allows more precise graft placement. Precise placement reduces trauma. Reduced trauma improves comfort. This positive cycle defines modern hair transplantation (Jimenez et al., 2021).
Frequently Asked Questions About Hair Transplant Pain
Does a Hair Transplant Hurt During the Procedure?
No. Local anesthesia eliminates pain during the procedure.
What Is the Most Painful Part of a Hair Transplant?
The anesthesia injection causes the most discomfort. It lasts 30 to 60 seconds.
How Long Does Pain Last After a Hair Transplant?
Pain typically lasts 2 to 3 days. Most patients feel minimal discomfort by day 3.
Is FUE Less Painful Than FUT?
Yes. Clinical studies prove FUE causes less postoperative pain. Park et al. (2019) found FUE pain scores were significantly lower than FUT scores on days 1 through 4.
Can Surgeons Completely Avoid Pain?
Surgeons cannot eliminate all discomfort. They can minimize it significantly. Modern techniques make the experience mild for the vast majority of patients.
What Is the Final Verdict on Hair Transplant Pain?
Hair transplant pain is low, temporary, and manageable. Modern techniques ensure a near pain-free experience.
The evidence is clear. Hair transplantation does not cause severe pain. The most uncomfortable moment is the anesthesia injection. This moment lasts less than one minute. The procedure itself is painless. Postoperative discomfort peaks within 48 hours. It then declines rapidly. By day 3, most patients feel minimal sensation. By day 7, pain is essentially gone.
Technique selection influences comfort. FUE produces less pain than FUT. Advanced tools like sapphire blades further reduce trauma. Surgeon skill matters. Anesthesia technique matters. Patient anxiety management matters. Together, these factors create an experience that most patients describe as far easier than expected.
Prospective patients should focus on scientific data rather than forum horror stories. They should choose experienced surgeons. They should ask about pain management protocols. They should follow aftercare instructions carefully. With these steps, hair transplantation offers a path to restored confidence without significant physical suffering.
References
Fosko, Steven W., et al. “Repetitive pinching of the skin during lidocaine infiltration reduces patient discomfort.” Journal of the American Academy of Dermatology, vol. 39, no. 1, 1998, pp. 74-78.
Garcia Carmona, Mario, and Miriam Garcia Tejeda. “Local anesthesia and its considerations in hair transplantation with the FUE technique.” Acta Bioclinica, vol. 15, no. 30, 2025.
Garra, Gregory, et al. “The Wong-Baker pain FACES scale measures pain, not fear.” Pediatric Emergency Care, vol. 29, no. 1, 2013, pp. 17-20.
Jimenez, Francisco, James E. Vogel, and Marc Avram. “Hair transplantation: Surgical technique.” Journal of the American Academy of Dermatology, vol. 85, no. 4, 2021, pp. 818-829.
Kehlet, Henrik, and Jørgen B. Dahl. “The value of ‘multimodal’ or ‘balanced analgesia’ in postoperative pain treatment.” Anesthesia & Analgesia, vol. 77, no. 5, 1993, pp. 1048-1056.
Melzack, Ronald, and Patrick D. Wall. “Pain mechanisms: a new theory.” Science, vol. 150, no. 3699, 1965, pp. 971-979.
Nusbaum, Bernard P. “Techniques to reduce pain associated with hair transplantation: optimizing anesthesia and analgesia.” American Journal of Clinical Dermatology, vol. 5, 2004, pp. 9-15.
Park, Jae Hyun, et al. “Comparison of postoperative pain according to the harvesting method used in hair restorative surgery.” Archives of Plastic Surgery, vol. 46, no. 5, 2019, pp. 458-464.
True, Richard H., and Robert M. Elliott. “Microprocessor-controlled local anesthesia versus the conventional syringe technique in hair transplantation.” Dermatologic Surgery, vol. 28, 2002, pp. 463-468.